Research Article - Onkologia i Radioterapia ( 2021) Volume 15, Issue 7
Student's attitude toward COVID-19 vaccine in health departments at King Khalid University, Abha, Saudi Arabia
Mishari HM Alshyarba1*, Basmah Mishari H Alshyarba2, Waad Abdulwahab A Alalshaikh2, Amani Alhazmi2 and Farah Aziz32Department of Public Health, College of Applied Medical Sciences, King Khalid University, Khamis Mushait, Saudi Arabia
3Department of Basic Medical Sciences, College of Applied Medical Sciences, King Khalid University, Khamis Mushait, Saudi Arabia
Mishari HM Alshyarba, Department of Surgery King Khalid University 61421, Abha, ORCID ID: https://orcid.org/0000 0003-2697- 3591, Saudi Arabia, Tel: +966555757150, Email: mhalshyarba@kku.edu.sa
Received: 01-Jun-2021 Accepted: 30-Jul-2021 Published: 06-Aug-2021
Abstract
Objective: This study aims to investigate Student’s attitude toward COVID-19 vaccine in health departments at King Khalid University, Saudi Arabia.
Methods: A cross-sectional, self-administered questionnaire-based survey. The study includes 258 health department students (male and female) in Abha, Khamis Mushait and Muhayil of Aseer region. Statistical analysis was performed using descriptive statistical analysis.
Results: The total 258 respondents participated in the research. The female respondents were 87% and male respondents were 13%. Mean of the acceptance ± S.D was 23.45 ± 4.5. 41.1% of the respondents accepted to take free vaccine while 41.5% responded to take vaccine even if it is not free, 17.4% totally rejected to take the vaccine (either free or not).
Conclusion: This study highlights that most of the participants of this study agreed to take COVID-19 vaccine. The rest of the respondents were reluctant to receive the vaccine. They need more health and media education about the vaccine benefits.
Keywords
COVID-19, vaccine, vaccination, SARS-CoV-2, coronavirus, clinical trials, MERS-CoV, ARDS.
Introduction
In the last few decades, there have been several global viral pandemic. Recently, coronavirus disease (COVID-19) has become a viral pandemic. In December 2019, people in Wuhan, in China’s Hubei Province, reported many linked cases of unexplained pneumonia-like symptoms [1]. The etiological agent of this pneumonia was later discovered to be a virus, and was named 2019- nCoV [2]. This virus belongs to the same family of b-coronaviruses that caused the Severe Acute Respiratory Syndrome (SARS) outbreak in 2003 and the Middle East Respiratory Syndrome (MERS) outbreak in 2012 [3,4]. During 2020, the world was devastated by the overwhelming effects of the COVID-19 pandemic, with more than 1.8 million deaths and the exhaustion of healthcare systems, in addition to its negative socio-economic and psychologic impacts [5-10].
Pfizer and its German partner BioNTech applied to the Food and Drug Administration to authorize its corona-virus vaccine for emergency use on November 20, 2020. The company estimates it is 95% effective. They plan on making 50 million does available by the end of December. The United States will receive 25 million then, 30 million in January, and 35 million in February and March. Neergaard (2020) reported that Moderna will apply for emergency use of its vaccine that they state is as effective as Pfizer's within weeks [6-15].
The study showed that a surveyed 258 college students to assess why they were reluctant to be vaccinated for the H1N1 influenza. College students had one of the highest frequency rates for infection; however, 8% received the H1N1 vaccine. Yang found that most students were not knowledgeable about the basic details about H1N1 and the H1N1 vaccine. Another surveyed 735 college students to decide whether they will decide to be vaccinated for the COVID-19 coronavirus vaccine. They found that 633 (86.1%) students reported that they would be vaccinated and 102 (13.9%) indicated that they would not or were not sure [15-20].
The Kingdom of Saudi Arabia (KSA) was quick to adopt unprecedented measures to control the transmission; for instance, the KSA placed restrictions on the inbound Umrah pilgrimage on February 27, 2020. The kingdom also suspended the recently introduced e-Visa program, banned the inbound travel of persons from COVID-19-affected countries, and restricted the travel of Gulf Cooperation Council (GCC citizens who had recently travelled to COVID-19-affected countries [21]. Finally, all schools, universities, and mosques throughout the kingdom were closed [22,23]. Information does change perceptions. Steps need to be taken now to determine if college students will get the vaccine in order to design information campaigns geared towards them.
Methodolgy
A descriptive cross-sectional approach was for this study. The study was conducted during the period from September 2020 to January 2021. All students filled enrolled in the selected courses/levels were included in this study. Those who filled the questionnaire were included in the study. Information was gathered utilizing organized poll which created by the specialists after intensive writing survey and master's counsel. The poll information incorporated individual's sociosegment information. Board specialists looked into the survey autonomously for content legitimately and every revealed change and adjustments were applied till the last instrument accomplished. A sequential accommodation examining strategy was utilized due. Ethical endorsement was gotten from REC of the school and educated assent was taken from the members.
After information were extricated, it was overhauled, coded and taken care of factual programming IBM SPSS variant 22 (SPSS, Inc. Chicago, IL). Chi-square tests used for comparisons at 0.05 level of significance.
Results
The total 258 respondents were participated in the research. Mean ± S.D was 23.45 ± 4.5. The female respondents were 87% and male respondents were 13%. 41.1% of the respondents stated that “I’ll only take the vaccine if it’s free” 41.5% responded that “I will get the vaccine even if it is not free” 17.4% stated that “I will never get the vaccine (either free or not)” Table 1.
| COVID-19 vaccination decision | Frequency | Percent | |
|---|---|---|---|
| Valid | No, I will never get the vaccine (either free or not) | 45 | 17.4 |
| Yes, I will get the vaccine even if it is not free | 107 | 41.5 | |
| Yes, I’ll only take the vaccine if it’s free | 106 | 41.1 | |
| Total | 258 | 100 | |
Table 1: Overall survey on vaccination decision
Table 2 depicted that majority of the respondents got information from 34.5% and 33.7% social media and WHO, CDC respectively.
Table 3 depicted that 45.7% of the respondents having believe on conspiracy theories.
| Source of information | Frequency | Percent | |
|---|---|---|---|
| Valid | Internet search | 21 | 8.1 |
| Media | 31 | 12 | |
| Other | 30 | 11.6 | |
| Social media | 89 | 34.5 | |
| WHO , CDC | 87 | 33.7 | |
| Total | 258 | 100 | |
Table 2: Source of Information on vaccination
| Do you believe about conspiracy theories? | Frequency | Percent | |
|---|---|---|---|
| Valid | No | 140 | 54.3 |
| Yes | 118 | 45.7 | |
| Total | 258 | 100 | |
Table 3: Conspiracy theories on COVID vaccination
Table 4 depicted that 78.7% of the respondents agreed that they have sufficient knowledge to make decision regarding COVID-19 vaccination.
| My information about the disease is sufficient to make a decision about taking the vaccine | Frequency | Percent | |
|---|---|---|---|
| Valid | No | 55 | 21.3 |
| Yes | 203 | 78.7 | |
| Total | 258 | 100 | |
Table 4: Overall information on vaccination decision
Figure 1 depicted that conspiracy theories were the major barriers in opting the vaccination procedure.
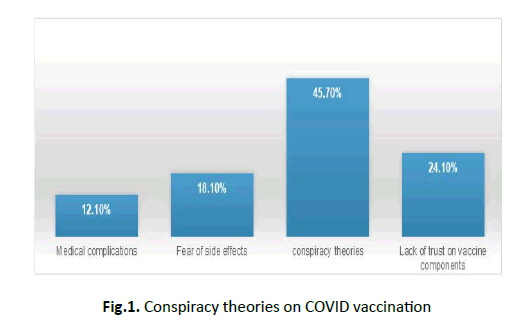
Figure 1: Conspiracy theories on COVID vaccination
Figure 2 depicted that 45% will go for vaccination to enhance immunity, 30% for back to normal life.
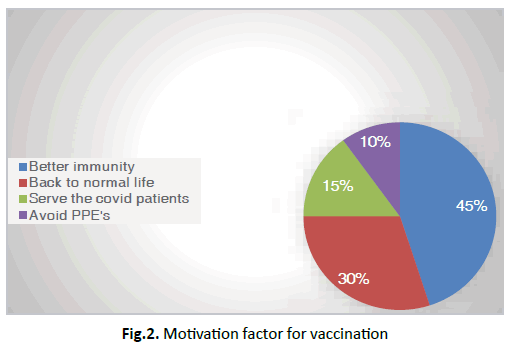
Figure 2: Motivation factor for vaccination
Table 5 depicted that we did not observe significant gender differences while comparing vaccination decisions.
| Gender | Does the availability of the vaccine free of charge affect your decision? | Total | |||
|---|---|---|---|---|---|
| No, I will never get the vaccine (either free or not) | Yes, I will get the vaccine even if it is not free | Yes, I’ll only take the vaccine if it’s free | |||
| Gender | Female | 41 | 97 | 86 | 224 |
| Male | 4 | 10 | 20 | 34 | |
| Total | 45 | 107 | 106 | 258 | |
Table 5: Gender does the availability of the vaccine free of charge affect your decision? Cross tabulation
Discussion
Our results showed that the large number of respondents is accepting to be vaccinated. it's clear from the students' responses. Limitations to this that their main concern is fear of the presumptive inadequate clinical trials on the vaccines and hence the adverse effects of all vaccines are not well elaborated. The lack of confidence about the vaccine benefits has been observed in the quarter of the study sample (24.1%). This could be attributed to the lack of scientific true information that the benefits of the vaccine overweigh its risks.
Many high-profile people locally, statewide, and nationally are vaccinated publicly on television, within the newspapers and social media. This is often important for the giant parts of the population. Unfortunately, college students get their news online [24, 25] which have no scientific basis. Additionally, students who provided comments mentioned vaccine politicization. The need for information transparency is the pillar of positive vaccine attitude [26-29]. Our study suggested that we did not observe significance difference between gender regarding the vaccination decision. Bassetti M et al. observed no gender difference in vaccine attitude [30].
A group of researchers conducted a cross-sectional survey study about COVID-19 with adults in the US in May 2020 (about two months after COVID-19 was declared a pandemic). Eligibility criteria included being age 18 or older and currently living in the US. They utilized a convenience sample from this online panel for this study. They found that nearly 70% of adults in the US would be willing to get a COVID-19 vaccine if one becomes available, where 59%-75% of US adults indicated a willingness to get vaccinated [31]. Their finding represents one of the first estimates of acceptability of a COVID-19 vaccine in the US and can be used to guide projections of future vaccine uptake [32].
Vaccine acceptability was lower among several demographic groups, including participants who were non-Latinx black, had lower incomes, had no health insurance, or were conservative in their political leaning. The pattern among non-Latinx black participants is concerning since early data suggest that non- Latinx blacks have among the highest COVID-19 incidence and mortality rates in the US [33-35]. Study includes the crosssectional design and self-reported data.
Conclusion
This study highlights that most of the participants of this study agreed to take COVID-19 vaccine. The rest of the respondents were reluctant to receive the vaccine. They need more health and media education about the vaccine benefits.
Acknowledgement
We acknowledged the services of Mr. Muhammad Abid Khan for data analysis.
References
- World Health Organization. Rolling updates on coronavirus disease (COVID-19). 2020.
- World Health Organization. Report of the WHO-China Joint Mission on coronavirus disease 2019 (COVID-19). 2020. Significant account of fatality rates and comorbidities in reports from China related to COVID-19 infection.
- Barry M, Al Amri M and Memish ZA. COVID-19 in the shadows of MERS-CoV in the Kingdom of Saudi Arabia. J Epidemiol Glob Health. 2020;10:1-3.
- Guo YR, Cao QD, Hong ZS, Tan YY, Chen SD, et al. The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak-an update on the status. Mil Med Res. 2020;7:11.
- Jahanshahi AA, Dinani MM, Madavani AN, Li J, Zhang SX. The distress of Iranian adults during the Covid-19 pandemic- More distressed than the Chinese and with different predictors. Brain Behav Immun. 2020;87:124-125.
- Morgantini LA, Naha U, Wang H, Francavilla S, Acar O, et al. Factors contributing to healthcare professional burnout during the COVID-19 pandemic: A rapid turnaround global survey. PLoS ONE. 2020;15:e0238217.
- Bandyopadhyay S, Baticulon RE, Kadhum M, Alser M, Ojuka DK, et al. Infection and mortality of healthcare workers worldwide from COVID-19: A systematic review. BMJ Glob Health. 2020;5:e003097.
- Mukaetova-Ladinska EB, Kronenberg G. Psychological and neuropsychiatric implications of COVID-19. Eur Arch Psychiatry Clin Neurosci. 2021;271:235-248.
- Nicola M, Alsafi Z, Sohrabi C, Kerwan A, Al-Jabir A, et al. The socio-economic implications of the coronavirus pandemic (COVID-19): a review. Int J Surg. 2020;78:185-193.
- Worldometer. COVID-19 Coronavirus Pandemic.
- Ebrahim S, Memish Z. Saudi Arabia’s drastic measures to curb the COVID-19 outbreak: temporary suspension of the Umrah pilgrimage. J Travel Med. 2020;27:taaa029.
- Ministry of Education. 2020.
- The official Saudi Press Agency. Spa.gov.sa. 2020.
- Hassan B, Shati AA, Almari A, Patel A, Asseri AA. Online assessment for the final year medical students during COVID-19 pandemics; the exam quality and students' performance.Onkologia I Radiotrapia. 2020;14:1-6.
- National Academies Release Framework for Equitable Allocation of a COVID-19 Vaccine for Adoption by HHS, State, Tribal, Local, and Territorial Authorities. 2020.
- Larson HJ, Jarrett C, Schulz WS, Chaudhuri M, Zhou Y, et al. SAGE Working Group on Vaccine Hesitancy. Measuring vaccine hesitancy: the development of a survey tool. Vaccine. 2015;33:4165-4175.
- Kernéis S, Jacquet C, Bannay A, May T, Launay O, et al. Vaccine education of medical students: a nationwide cross-sectional survey. Am J Prev Med. 2017;53:e97-e104.
- Afonso NM, Kavanagh MJ, Swanberg SM, Schulte JM, Wunderlich T, et al. Will they lead by example? Assessment of vaccination rates and attitudes to human papilloma virus in millennial medical students. BMC Public Health. 2017;17:35.
- Betsch C, Wicker S. E-health use, vaccination knowledge and perception of own risk: drivers of vaccination uptake in medical students. Vaccine. 2012;30:1143-1148.
- Fisher KA, Bloomstone SJ, Walder J, Crawford S, Fouayzi H, et al. Attitudes toward a potential SARS-CoV-2 vaccine: a survey of U.S. adults. Ann Intern Med. 20;173:964-973.
- Dror AA, Eisenbach N, Taiber S, Morozov NG, Mizrachi M, et al. Vaccine hesitancy: the next challenge in the fight against COVID-19. Eur J Epidemiol. 2020;35:775-779.
- Reiter PL, Pennell ML, Katz ML. Acceptability of a COVID-19 vaccine among adults in the United States: how many people would get vaccinated? Vaccine. 2020;38:6500.
- National Vaccine Advisory Committee Recommendation from the National Vaccine Advisory Committee: standards for adult immunization practice. Public Health Rep. 2014;129:115-123.
- Edwards KM, Hackell JM. Committee on infectious diseases, the committee on practice and ambulatory medicine. Countering vaccine hesitancy. Pediatrics. 2016;138:2016-2146.
- Schaffer DeRoo S, Pudalov NJ, Fu LY. Planning for a COVID-19 vaccination program. JAMA. 2020;323:2458-2459.
- Onello E, Friedrichsen S, Krafts K, Simmons J, Diebel K, et al. First year allopathic medical student attitudes about vaccination and vaccine hesitancy. Vaccine. 2020;38:808-814.
- Chen N, Zhou M, Dong X, Qu J, Gong F, et al. Epidemiological and clinical characteristics of 99 .23 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descrip- tive study. Lancet. 2020;395:507-513.
- Giovanetti M, Benvenuto D, Angeletti S, Ciccozzi M. The first two cases of 2019-nCoV in Italy: where they come from? J Med Virol. 2020;92:518-521.
- Shigemura J, Ursano RJ, Morganstein JC, Kurosawa M, Benedek DM. Public responses to the novel 2019 coronavirus (2019-nCoV) in Japan: mental health conse- quences and target populations. Psychiatry Clin Neurosci. 2020;74:281.
- Bassetti M, Vena A, Giacobbe DR. The novel Chinese coronavirus (2019- nCoV) infections: challenges for fighting the storm. Eur J Clin Invest. 2020;50:e13209.
- JCH Impact. New Yorkers and COVID-19 (week 7). 2020.
- Kelly B, Bann C, Squiers L, Lynch M, Southwell B, et al. Predicting willingness to vaccinate for COVID-19 in the US. JHC Impact. 2020.
- Webb Hooper M, Napoles AM, Perez-Stable EJ. COVID-19 and racial/ethnic disparities. JAMA. 2020;323:2466-2467.
- APM Research Lab. The color of coronavirus: COVID-19 deaths by race and ethnicity in the U.S. 2020.
- Gross CP, Essien UR, Pasha S, Gross JR, Wang S, et al. Racial and ethnic disparities in population level COVID-19 mortality. 2020;35;3097-3099.



