Research Article - Onkologia i Radioterapia ( 2020) Volume 14, Issue 5
Volumetric-modulated arc therapy versus intensity-modulated radiotherapy for localized prostate cancer: a dosimetric comparative analysis of moderate hypofractionated radiation
Ramiz Abu-Hijlih1, Shatha Afifi1, Abdelatif Almousa1, Jamal Khader1, Wafa Alhajal1, Ibrahim Al Rjoub1, Sara Mheid1, Wafa Asha1, Samer Salah2, Khaled Dibs1, Sami Khatib3 and Fawzi Abuhijla1*2Medical Oncology Department, King Hussein Cancer Centre, Amman, Jordan
3Radiation Oncology, Afia Radiotherapy and Nuclear Medicine Centre, Amman, Jordan
Fawzi Abuhijla, Radiation Oncology Department, King Hussein Cancer Centre, Amman, Jordan, Email: fhijle@khcc.jo
Received: 13-Sep-2020 Accepted: 26-Sep-2020 Published: 05-Oct-2020
Abstract
Aim: To compare Intensity Modulated Radiotherapy (IMRT) and Volumetric-Modulated Arc Radiotherapy (VMAT) for patients receiving moderate hypofractionated radiotherapy. Introduction: Hypofractionated radiation has been established for localized prostate cancer; however, eligibility for this treatment depends on strict dosimetric constraints. Methods: CT simulation datasets of 23 patients with localized prostate adenocarcinoma were analysed, IMRT and VMAT plans were generated for each patient. Dose Volume Histogram (DVH) records, Monitor Units (MUs), treatment delivery times, conformality, and homogeneity indices were compared between the two techniques. Hypofractionated regimen parameters were assessed for each technique to evaluate plan eligibility for the short-course radiotherapy (60 Gy over 20 fractions). Results: Compared with IMRT plans, VMAT resulted in better PTV coverage (p=0.001) and significantly decreased bladder and rectal (D50) doses (p=0.019 and p=0.002, respectively). Both conformality and homogeneity were improved with VMAT but did not reach statistical significance. The mean MUs were lower with VMAT than with IMRT (662 vs 738). Moreover, the treatment time was shorter with VMAT than with IMRT (mean, 1.8 vs 7.1 minutes, p= 0.004). Four IMRT plans did not meet hypofractionated objectives and were deemed not eligible for short-course radiotherapy. All VMAT plans met the planning objectives. Conclusion: For hypofractionated prostate irradiation, VMAT resulted in improved PTV (D99) coverage and more sparing of surrounding tissues. VMAT used less MUs and shorter treatment time. VMAT could meet all constraints and made patients eligible for hypofractionated radiotherapy. Therefore, VMAT may be preferred for patients who undergo moderate hypofractionation scheme.
Keywords
VMAT, IMRT, prostate cancer, dosimetry
Introduction
Prostate cancer is the most frequent urological malignancy [1]. Radiotherapy forms an integral part in the management of this disease. In the last few decades, dose escalated radiation has led to improvement in biochemical control [2-4]. However, patients should commence for two months treatment. This long procedure is costly and inconvenient for both cancer patients and radiation facilities. Recently, hypofractionated radiation has been studied in multiple prospective trials, and it has proven equivalence in terms of disease control and toxicity profile [5-7]. This approach enables patients to complete their radiotherapy schedule in only 4 weeks instead of 8 weeks, nevertheless, eligibility for hypofractionated radiation requires many dosimetric objectives to be fulfilled; for example, meeting strict organs at risk constraints, if these targets are not met then treatment will be carried with standard fractionation radiotherapy [7]. Therefore, radiotherapy plan should be highly conformal in order to deliver a higher dose per fraction to the prostate while sparing nearby normal tissues, particularly rectum and bladder. Advanced radiation techniques are set to meet this goal, their superiority over conventional radiation has been acknowledged [8]. Nowadays, Intensity Modulated Radiotherapy (IMRT) and Volumetric Modulated Arc Radiotherapy (VMAT) are used in many centers to treat prostate cancer. The use of these contemporary techniques is more valuable when high dose per fraction is utilized, for instance; hypofractionated prostate irradiation.
Aim
The aim of this study is to perform a dosimetric comparison between VMAT and IMRT techniques in patients receiving moderate hypofractionated radiotherapy for localized prostate cancer, and to evaluate the eligibility for hypofractionated approach using each technique.
Materials and Methods
Patient population
At presentation, all patients were investigated with complete physical examination and laboratory testing (PSA and testosterone). Trans-rectal biopsy was obtained for diagnosis of prostatic adenocarcinoma. Staging work up; bone scan and Computed Tomography (CT) were performed to rule out distant metastasis. In addition, pelvic Magnetic Resonance Imaging (MRI) was acquired to evaluate loco-regional extension of the disease. Patients eligible for hypofractionated course were; low and intermediate-risk prostate cancer (T1-T2c, Gleason 6-7 and PSA<20 ng/mL) without evidence of disease spread to the lymph nodes or bone.
Treatment planning
The management strategy was discussed at the genitourinary multidisciplinary meetings. After obtaining the consent for radiation treatment, CT-simulation was performed to all cases with 2 mm slice thickness, patients were counselled for full bladder and empty rectum during all radiotherapy sessions. The whole prostate was defined as Clinical Target Volume (CTV), and the proximal 10 mm of the seminal vesicles were included if the risk of seminal vesicle involvement was>15% by Partin’s nomogram [9]. Planning Target Volume (PTV) was created with 10 mm expansion in all directions, except 7 mm posteriorly [7]. All the radiation plans were generated on Pinnacle (Pinnacle system 9.1-Koninklijke Philips N., Amsterdam, Netherlands) using VMAT. Radiotherapy was delivered in 3-Gy fractions over 20 sessions for a total radiation dose of 60 Gy. Moreover, concurrent hormonal treatment was prescribed for six months.
CT simulation data sets of 23 patients with prostate cancer who were treated with VMAT between January 2018 and February 2020 were randomly selected for this institutional review board approved study. All the plans were regenerated using step and shoot IMRT inverse planning applying the same planning objectives. The IMRT plans were performed with 6 MV energy, using Direct Machine Parameter Optimization (DMPO) technique with 7-9 beams. Of note, all VMAT plans were delivered with one arc. The planning grid used in both techniques was 35 cm in length.
According to the hypofractionated radiation protocol, the prostate tumor volumes coverages and Organs at Risks (OAR) constraints, specifically bladder and rectum, should be met before proceeding with hypofractionated regimen. If the plan is not meeting the Dose-Volume Histogram (DVH) objectives, then treatment should be carried with standard fractionation approach (75.6 Gy over 42 fraction) in reference to PROFIT trial protocol [7].
The planning objectives for target coverage were: CTV (D99) ≥ 60 Gy and PTV (D99) ≥ 57Gy, while OAR constraints were; bladder wall (D50) not more 37 Gy and (D30) not more 47 Gy. For the rectal wall (D50) should be limited to 37 Gy and (D30) not more 47 Gy, the head of femur (D5%) should be less than 43 Gy. Of note, D (volume)% refers to percent of target volume receiving a minimum of specific dose.
Furthermore, an expansion rings were created by adding 1, 2, 5 and 10 cm to the PTV, the mean doses at these contours were recorded after subtracting PTV to estimate dose fall-off in the surrounding tissues. The 10 cm expansion was limited to external body contour.
Plan homogeneity was assessed using International Commission on Radiation Units and Measurements (ICRU 83) definition of homogeneity index; defined as (D2%-D98%)/(D50%) [10]. In addition, we compared IMRT and VMAT plans conformality; defined as (Treated volume with 95% isodose-line)/(PTV volume). Monitor units for each plan were documented and compared.
The actual treatment time for VMAT was compared with IMRT treatment time; delivered in QA mode. Of note, gantry motion time was included in this estimation.
All the plans were reviewed by the radiation oncologist after being checked by two senior medical physicists. The deliverability of the IMRT and the VMAT plans was verified using the PTWs' OCTAVIUS 4D and the data was analysed with Verisoft S070009 software (PTW, Freiburg-Germany). Radiation was delivered using Versa HD- Elekta® linear accelerator mounted with XVI R5.0.3 (XVI, Elekta Oncology Systems Ltd., UK) [11].
Statistical Analysis
Descriptive analysis was performed; summary statistics were reported as mean and median where appropriate. Target volume coverage and DVH records were obtained automatically from Pinnacle planning system. The VMAT and IMRT plans parameters; mean volumes, homogeneity and conformality indices were compared by One-way ANOVA analysis. A statistical significant level at less than 0.05 was determined. All analyses were performed using SAS version 9.4 (SAS Institute Inc, Cary, NC).
Results
Patient’s characteristics
All patients were diagnosed with low and intermediate risk prostate cancer, Gleason score (6 in 3 patients and Gleason 7 in 20 patients). The disease was localized in the prostate for the whole cohort, and median PSA level was 11 μg/mL. Median patients’ age was 71 years. Table 1 illustrates patient’s characteristics. All patients received definitive hypofractionated radiation as 60 Gy over 20 fractions, in addition to six months of androgen deprivation therapy to all patients but one.
| Age (years) | |
| Range | 66-77 |
| Mean | 71 |
| Gleason score | |
| 6 (3+3) | 3 (13%) |
| 7 (3+4) | 11 (48%) |
| 7 (4+3) | 9 (39%) |
| T-stage (AJCC 8th edition) | |
| T1 | 2 (9%) |
| T2a | 3 (13%) |
| T2b | 10 (43%) |
| T2c | 8 (35%) |
| PSA level at presentation (µg/ml) | |
| Range | 4-18 |
| Mean | 11 |
| Risk group | |
| Low risk | 2 (13%) |
| Favorable intermediate | 11 (48%) |
| Unfavorable intermediate | 9 (39%) |
| Received 6 months of hormones | |
| Yes | 22 |
| No | 1 |
| N-stage (AJCC 8th edition) | |
| Nodal involvement | 0 |
| Non involved | 23 |
Tab. 1. Illustrates patients demographic, disease and treatment characteristics
Dosimetric comparison
All plans were optimized using same planning constraints. Meeting OARs constrains was prioritized over target coverage at time of planning using both techniques. The DVH records were analysed, all VMAT plans were meeting the objectives required for hypofractionated radiation approach. Conversely, four IMRT plans did not meet the prerequisite parameters. VMAT was superior in terms of target volume coverage and OAR sparing (Figure 1).
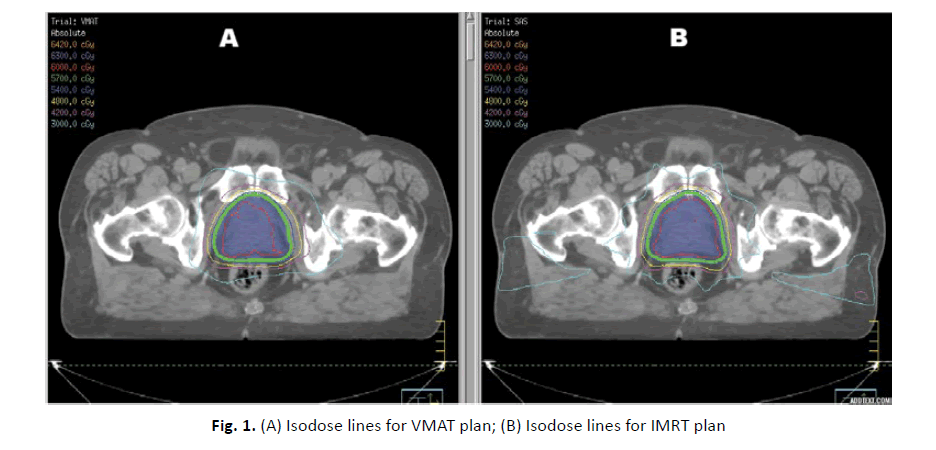
Figure 1: (A) Isodose lines for VMAT plan; (B) Isodose lines for IMRT plan
The mean PTV (D99) dose was 58.3 Gy with VMAT and 57 Gy for IMRT (p=0.001), the plan with minimum PTV (D99) coverage was 55.3 Gy for IMRT and 57.1 Gy for VMAT. Regarding OAR, VMAT met all required objectives for short course, and demonstrated more OAR sparing; (the average) rectal wall (D50) was 23.2 Gy in VMAT and 27.8 Gy in IMRT (p=0.002), similarly, bladder wall (D50) was 20.7 Gy for VMAT and 24.2 Gy for IMRT (p=0.019) (Figure 2).
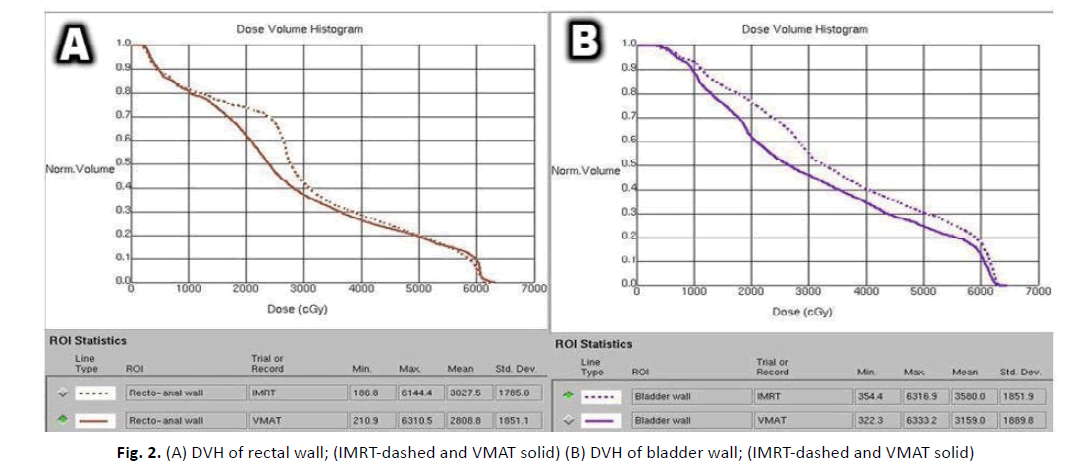
Figure 2: (A) DVH of rectal wall; (IMRT-dashed and VMAT solid) (B) DVH of bladder wall; (IMRT-dashed and VMAT solid)
Moreover, VMAT plans showed better conformality index (mean; 1.09 versus 1.13) and improved homogeneity, but the difference was not statistically significant. Notably, some IMRT plan did not meet rectal and bladder (D30) dose constraints.
The treatment time was also less with VMAT (mean; 1.8 vs 7.1 minutes, p=0.004). Furthermore, the monitor units used in VMAT were less than IMRT. Table 2 illustrates dosimetric parameters for IMRT and VMAT plans.
| Reference endpoint | IMRT | VMAT | p-value | |
| Number of beam angles/arcs Prostate CTV (D99) | 7-9 | 1 | ||
| Mean | ≥ 60 Gy | 59.7 | 60.2 Gy | 0.22 |
| Range | (57.9-60.6) | (60-60.5) | ||
| PTV (D99), | ||||
| Mean (Gy) | ≥ 57 Gy | 57 | 58.3 Gy | 0.001 |
| Range | (55.3-59.1) | (57.1-59.4) | ||
| Homogeneity Index | ||||
| Mean | 0.07 | 0.04 | 0.332 | |
| Range | (0.03-0.11) | (0.01-0.08) | ||
| Conformality Index | ||||
| Mean | 1.13 | 1.09 | 0.798 | |
| Range | (0.96-1.28) | (1.01-1.14) | ||
| Rectal wall dose, D50 | <37 | |||
| Mean (Gy) | 27.8 | 23.2 | 0.002 | |
| Range | (21.4-33.9) | (18.9-29.4) | ||
| Rectal wall dose, D30 | <46 | |||
| Mean (Gy) | 43.2 | 38.2 | 0.12 | |
| Range | (31.2-53.1) | (31-45.1) | ||
| Bladder wall dose, D50 | <37 | |||
| Mean (Gy) | 24.2 | 20.7 | 0.019 | |
| Range | (17-31.1) | (12-29.2) | ||
| Bladder wall dose, D30 | <46 | |||
| Mean (Gy) | 41.3 | 35.8 | 0.189 | |
| Range | (30.5-51.1) | (26.8-46.2) | ||
| Femoral head dose, D5 | ||||
| Mean (Gy) | <43 | 23.3 | 22.2 | 0.301 |
| Range | (14.5-30.2) | (15-26.2) | ||
| Monitor Units (MU) | ||||
| Mean | 738 | 662 | 0.101 | |
| Range | (549-872) | (594-760) | ||
| Dose fall-off, at (Gy) | ||||
| 1 cm (mean) | 52.1 | 49.4 | 0.82 | |
| Range | (49.2-53.5) | 47.8-52.4 | ||
| 2 cm (mean) | 38.2 | 37.5 | 0.048 | |
| Range | (34.2-41.7) | (35.6-42.6) | ||
| 5 cm (mean) | 18.2 | 17.9 | ||
| Range | (14.6-22.8) | (15.2-22.6) | 0.32 | |
| 10 cm (mean) | 10.9 | 12.3 | ||
| Range | (9.2-17.60) | (10.6-19.3) | 0.41 |
Tab. 2. Dosimetric comparison of target coverage and OARs between IMRT and VMAT
Additionally, radiation dose fall-off was improved with VMAT, the doses at 1 cm, 2 cm and 5 cm from PTV were less, but the difference was statistically significant only at 2 cm (p=0.048). On the contrary, mean dose at 10 cm was less with IMRT, but difference was not significant. Noteworthy, radiation dose to penile bulb was significantly less in the VMAT plans (mean doses; 27 Gy vs 30.5, p=0.002).
Discussion
A recent consensus guidelines from American Society for Radiation Oncology (ASTRO), American Society for Clinical Oncology (ASCO) and American Urology Association (AUA) have endorsed the use of moderate hypofractionated radiation in patients with localized prostatic adenocarcinoma [12]. This approach has proven equivalence with standard fractionation in terms of biochemical control and radiotherapy related toxicity. Moreover, implementation of hypofractionated radiation would improve treatment cost-effectiveness; and decrease additional costs such as residence and transportation, and for the radiation facility two patients can be treated at the same time of one patient. However, irradiating normal nearby organs is a matter of concern when higher dose per fractions is utilized because, in general, it can be associated with increased toxicities.
The radiation techniques have evolved dramatically in the last few decades, introduction of IMRT revolutionized radiation delivery and improved conformality, and therefore it was widely adopted [13]. VMAT is a newer tool for radiation delivery using arcs, some reports suggested superiority of VMAT over IMRT, while other studies did not find a meaningful difference [14-16].
A small series compared these two techniques in prostate cancer patients who received standard fractionation (2 Gy per fraction), VMAT demonstrated better bladder and rectum sparing and less monitor units, however, target volume coverage was similar [17].
A recent meta-analysis looked at published studies comparing IMRT and VMAT in prostate cancer, they analysed 110 plans and found that VMAT significantly decreased rectal dose with less monitor units and treatment time [18]. A study by Quan et al. compared eleven VMAT and IMRT plans, generated using in-house-developed automatic inverse planning algorithm. VMAT was superior in term of rectal sparing, monitors units and treatment time [15]. Another study by Mellon et al investigated 32 plans and revealed better homogeneity and shorter-radiotherapy time with VMAT, this was associated with reduced intrafraction motion [19]. Our results came in concordance with these reports, VMAT manifested better OAR sparing and improved treatment time and workflow in patients receiving short course scheme.
To the best of our knowledge, this is the first study in the literature comparing IMRT and VMAT expressly for moderate hypofractionated prostate irradiation. In this series, 23 plans were optimized using both step and shoot IMRT and VMAT. Four out of ten IMRT plans failed to meet plan objectives, those patients deemed not eligible for hypofractionated regimen using IMRT, although the same patients would be eligible for hypofractionation using VMAT.
Aforementioned, VMAT employed less monitor units than IMRT, although the difference was not significant. Additionally, treatment time was less with VMAT with significant p value, this fact would potential decrease intra-fractional random errors and make radiotherapy more convenient because patients are required to maintain their bladder full during the session and the urinary system is usually irritated with radiation. Moreover, less treatment time may translate in improved workflow within radiotherapy facility.
Furthermore, VMAT showed better conformality and homogeneity along with superior dose fall-off profile, this conveys to decrease radiation dose to surrounding tissues and diminish radiation associated side effects.
Sexual function is a major concern for many prostate patients, the erectile dysfunction is usually influenced by age, in addition to other factors such as cancer treatment; radiotherapy and hormones. Many studies have shown that the dose received by penile bulb is predictive for erectile dysfunction [20, 21]. Moreover, this effect is increased when hypofractionated radiotherapy is employed [22]. For this reason, one of the radiotherapy planning targets is decreasing the dose to the bulb as possible. Notably, in our study the dose to penile bulb was statistically significantly lower with VMAT when compared with IMRT.
This study suffers retrospective nature and associated potential selection bias. It is known that planning outcomes can be influenced by the treatment planning system and planner experience, for this reason our plans optimization was performed by the same experienced physicist. We acknowledge that dosimetric comparative studies are subject to multiple factors that may influence the results, for example; planning tools, comparative methods and other factors like patient’s anatomy. The effect of these factors cannot be entirely excluded, even with optimal balancing between both techniques. Accordingly, some of the outcomes may result from this confounding effect. Comparing our results with other series in the literature, may help to extract more consistent conclusions about the best planning method. In addition, comparing these techniques in multi-institutional prospective fashion, would provide a proper insight on the advantages and disadvantages of each technique.
Nowadays, higher doses per fraction (SBRT) are delivered using more sophisticated platforms, yet longer follow up is required to establish the role of such techniques [23].
Conclusion
In conclusion, a dosimetric comparison was performed between 23 IMRT plans and 23 VMAT plans for patients receiving moderate hypofractionated radiotherapy for localized prostatic adenocarcinoma. VMAT revealed a statistical significant improvement in PTV (D99) coverage and OAR sparing; specifically the rectum and bladder wall (D50), in addition to penile bulb. VMAT expressed superior conformality with less monitor units and shorter treatment time. Interestingly, four IMRT plans failed to meet the required hypofractionated objectives and were not eligible for this approach, VMAT showed ability meeting constraints and made patients eligible for hypofractionated radiotherapy. Interpretation of results should take into consideration limitations of such studies and potential influence of these factors on the conclusions.
References
- Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, et al. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87-108.
- Dearnaley DP, Sydes MR, Graham JD. Escalated-dose versus standard-dose conformal radiotherapy in prostate cancer: first results from the MRC RT01 randomised controlled trial. Lancet Oncol. 2007;8:475-487.
- Pollack A, Zagars GK, Starkschall G, Antolak JA, Lee JJ, et al. Prostate cancer radiation dose response: results of the MD Anderson phase III randomized trial. Int J Radiat Oncol Biol Phys. 2002;53:1097-1105.
- Peeters ST, Heemsbergen WD, Koper PC. Dose-response in radiotherapy for localized prostate cancer: results of the Dutch multicenter randomized phase III trial comparing 68 Gy of radiotherapy with 78 Gy. J Clin Oncol. 2006;24:1990-1996.
- Dearnaley D, Syndikus I, Mossop H, Khoo V, Birtle A, et al. Conventional versus hypofractionated high-dose intensity-modulated radiotherapy for prostate cancer: 5-year outcomes of the randomised, non-inferiority, phase 3 CHHiP trial. Lancet Oncol. 2016;17:1047-1060.
- Aluwini S, Pos F, Schimmel E, Krol S, Tooran P, et al. Hypofractionated versus conventionally fractionated radiotherapy for patients with prostate cancer (HYPRO): Late toxicity results from a randomised, non-inferiority, phase 3 trial. Lancet Oncol. 2016;17:464-474.
- Catton CN, Lukka H, Chu-Shu G. A randomised trial of a Hypofractionated radiation regimen for the treatment of localized prostate cancer. J Clin Oncol. 2017;35:1884-1890.
- Alongi F, Cozzi L, Fogliata A. Hypofractionation with VMAT versus 3DCRT in post-operative patients with prostate cancer. Anticancer Res. 2013;33:4537-4543.
- Partin AW, Kattan MW, Subong EN. Combination of prostate-specific antigen, clinical stage, and Gleason score to predict pathological stage of localized prostate cancer. a multi institutional update. JAMA. 1997;277:1445-1451.
- Hodapp N. The ICRU Report 83: prescribing, recording and reporting photon-beam Intensity-Modulated Radiation Therapy (IMRT). Strahlenther Onkol. 2012;188:97-99.
- Jaffray DA, Siewerdsen JH, Wong JW, Martinez AA. Flat panel cone-beam computed tomography for image-guided radiation therapy. Int J Radiat Oncol Biol Phys. 2002;53:1337-1349.
- Morgan SC, Hoffman K, Loblaw DA, Buyyounouski MK, Patton C, et al. Hypofractionated radiation therapy for localized prostate cancer: an ASTRO, ASCO, and AUA evidence-based guideline. J Clin Oncol. 2018;36:JCO1801097.
- Mell LK, Mehrotra AK, Mundt AJ. Intensity modulated radiation therapy use in the US, 2004. Cancer. 2005;104:1296-1303.
- Taggar AS, Graham D, Kurien E, Gräfe JL. Volumetric-modulated arc therapy versus intensity-modulated radiotherapy for large volume retroperitoneal sarcomas: A comparative analysis of dosimetric and treatment delivery parameters. J Appl Clin Med Phys. 2018;19:276-281.
- Quan EM, Li X, Li Y, Wang X, Kudchadker RJ, et al. A comprehensive comparison of IMRT and VMAT plan quality for prostate cancer treatment. Int J Radiat Oncol Biol Phys. 2012;83:1169-1178.
- Chen BB, Huang SM, Xiao WW, Sun WZ, Liu MZ, et al. Prospective matched study on comparison of volumetric-modulated arc therapy and intensity-modulated radiotherapy for nasopharyngeal carcinoma: dosimetry, delivery efficiency and outcomes. J Cancer. 2018;9:978-986.
- Onal C, Arslan G, Parlak C. Comparison of IMRT and VMAT plans with different energy levels using Monte-Carlo algorithm for prostate cancer. Jpn J Radiol. 2014;32:224-232.
- Ren W, Sun C, Lu N, Xu Y, Han F, et al. Dosimetric comparison of intensity-modulated radiotherapy and volumetric modulated arc radiotherapy in patients with prostate cancer: a meta-analysis. J Appl Clin Med Phys. 2016;17:254-262.
- Mellon EA, Javedan K, Strom TJ, Moros EG, Biagioli MC, et al. A dosimetric comparison of volumetric modulated arc therapy with step-and-shoot intensity modulated radiation therapy for prostate cancer. Pract Radiat Oncol. 2015;5:11-15.
- Thor M, Olsson C, Oh J. Radiation dose to the penile structures and patient-reported sexual dysfunction in long-term prostate cancer survivors. J Sex Med. 2015;12:2388-2397.
- Roach M 3rd, Nam J, Gagliardi G, El Naqa I, Deasy JO, et al. Radiation dose-volume effects and the penile bulb. Int J Radiat Oncol Biol Phys. 2010;76:S130-S134.
- McDonald AM, Baker CB, Shekar K, Popple RA, Clark GM, et al. Reduced radiation tolerance of penile structures associated with dose-escalated hypofractionated prostate radiotherapy. Urology. 2014;84:1383-1387.
- Ricco A, Hanlon A, Lanciano R. Propensity score matched comparison of intensity modulated radiation therapy vs stereotactic body radiation therapy for localized prostate cancer: a survival analysis from the national cancer database. Front Oncol. 2017;7:185.



