Research Article - Onkologia i Radioterapia ( 2023) Volume 17, Issue 1
The effect of music therapy applied to neonatales on their pain: Systematic review
Omer Terzi1, Gulay Manav1 and Pelin Uymaz2*2Keykubat University, Turkey
Pelin Uymaz, Keykubat University, Turkey, Email: pelin.uymaz@alanya.edu.tr
Received: 23-Nov-2022, Manuscript No. OAR-22-80740; Accepted: 30-Nov-2022, Pre QC No. OAR-22-80740 (PQ); Editor assigned: 25-Nov-2022, Pre QC No. OAR-22-80740 (PQ); Reviewed: 29-Nov-2022, QC No. OAR-22-80740 (Q); Revised: 30-Nov-2022, Manuscript No. OAR-22-80740 (R); Published: 01-Dec-2022
Abstract
Pain is emotional and psychological emotional state that an individual feels as a result of a tissue injury in his/her body along with past experiences. Although individuals can express this emotional state, infants cannot. Instead, infants show pain with physiological or behavioural symptoms. Behavioural symptoms can appear as crying, facial expressions and motor movements, while physiological symptoms can appear as changes in heart rate, an increase in the number of breaths and change in the oxygen value. Various measurement tools have been developed to measure pain. In total, more than 40 scales have been developed for use in premature, new born and post mature babies. The treatment of the pain evaluated with these measurement tools is performed by pharmacological and nonpharmacological treatment methods. Pharmacologically, opioid, non-opioid and cholangitis are used; while breast milk, kangaroo care, sucrose application, massage and voice applications are used as nonpharmacological methods. Studies have recently been carried out where nonpharmacological techniques are more prominent. SES applications, which are one of the nonpharmacological methods, have become widespread in intensive care units in recent years. This study aimed to reveal the effect of this prevalence in the last 20 years (2002-2022) and determine the effect of sound applications on pain in premature infants. In the research conducted in 16 databases with keywords, a total of 9301 articles were accessed. Among them, a selection was made according to the inclusion criteria and 17 articles were selected for the study. Of these articles, 82.3% (n=14) yielded positive results in audio applications. In addition to pain assessment, positive results were obtained by increasing SpO2 value, stabilization of heart rate, decrease in respiratory rate and shortening of crying time in studies. However, metaanalysis studies need to be carried out for voice applications to be called positive or negative.
Keywords
Neonatal nursing, neonate, pain, voice application
Introduction
Pain is an emotional and psychological mood, which occurs due to harmful stimuli. We can understand that infants feel pain through physiological symptoms such as change in their heart rate, increase in the number of breaths and change in the oxygen value or behavioral symptoms such as crying, facial expressions and motor movements. However, it is not easy to measure pain in neonates [1].
There are more than 40 scales used to measure the state of pain in infants, yet four of them are widely used. These are Premature Infant Pain Profile (PIPP), Neonatal Infant Pain Scale (NIPS), CRIES and FLACC pain scales [1,2].
Treatment of pain evaluated through these measurement tools is done with pharmacological and nonpharmacological treatment methods. Pharmacological methods are opioid, non-opioid and cholangitis; while nonpharmacological methods are breast milk, kangaroo care, sucrose application, massage and music therapy. Recent research has been conducted indicating that nonpharmacological methods outweigh [3].
Music therapy, one of nonpharmacological methods is diversion of the infant’s attention by making it listen to the mother’s voice, white noise, lullaby or musical instruments [4,5]. In such an application, infants showed recovery as decrease in pain, and increase in comfort and vital findings [6]. The mother’s heartbeat sound and her own voice were used for the relief of pain in neonates and found to be effective [4]. In an RCT study conducted with 60 premature infants, the oxygen saturation value of 30 infants who listened to music during peripheral central venous catheter insertion increased, and heart rates and pain scores decreased compared to the control group. Another RCT study, using white noise, the PIPP score, heart rate and respiratory rate decreased, while oxygen saturation value increased [7 ]. In an RCT study that listened to heart rate, there was an increase in SpO2 value and a decrease in PIPP pain score of the experimental group [8].
The literature review showed that Standley (2002) conducted a meta-analysis study by scanning studies from 1964 to 1999 to examine the effect of music therapy on pain in premature infants. After the year 2002, there was neither systematic review nor meta- analysis study. In recent years, the use of voice applications in intensive care units has become prevalent. To see how effective this prevalence has been, the present study is designed to evaluate the effect of voice applications on pain in premature infants over the last 20 years (2002-2022). The study included case-control studies conducted in the last 20 years. This systematic review aimed both to determine the effectiveness of voice applications in premature infants and to be a guide to new research topics.
Premature Infant Pain Profile (PIPP)
It was developed by Steven et al. (1996) for premature infants aged 28 weeks-36 weeks. Its Turkish validity and reliability study was conducted by Akcan and Yigit (2015). It is applicable to preterm and term infants and is scored between 0 and 21. A score of 0 points-6 points indicate that there is no pain or it is minimal, 7 points-12 points indicate that there is moderate severe pain and 13 points - 21 points indicate severe pain. It is used as an assessment 15 seconds before and 30 seconds after the painful procedure (Table 1) [9].
Tab. 1. Premature Infant Pain Profile-(PIPP)
| Categories | 0 | 1 | 2 | 3 |
|---|---|---|---|---|
| Gestational age | ≥ 36 weeks | 32 weeks - 35 | 28 weeks - 31 | <28 weeks |
| weeks 6 days | weeks 6 days | |||
| Behavioral status | Active/awake, eyes open, facial movements | Calm/awake, eyes open, no facial movements | Active/dormant, eyes closed, facial movements | Active/dormant, eyes closed, no facial movements |
| Max heart rate | An increase of 0- 4 heart rate per minute | An increase of 5- 14 heart rate per minute | An increase of 15- 24 heart rate per minute | An increase of 25 and more heart rate per minute |
| Min oxygen saturation | Decrease by 0- | Decrease by 2.5- | Decrease by 5- | Decrease by 7.5% and more |
| 2.40% | 4.90% |
7.40% |
||
| Wrinkling forehead | No | Slight |
Moderate |
Too much |
| Squinting | No | Slight |
Moderate |
Too much |
| Enlargement of the nose wings | No | Slight |
Moderate |
Too much |
Neonatal Infant Pain Scale(NIPS)
It was developed by Lawrence et al. (1993) and its Turkish validity and reliability study was conducted by Akdovan (1999) [10,11]. It is appropriate for the assessment of pain in premature and neonates. The obtainable score from the scale consisting of six deaths in total varies between 0 and 7. A higher score indicates more severe pain (Table 2).
Tab. 2. Neonatal Infant Pain Scale (NIPS)
| Category | 0 | 1 | 2 |
|---|---|---|---|
| Facial expression | Calm face, natural expression | Tense facial muscles, wrinkled forehead and chin | |
| Crying | Silent, no crying | Howling and intermittent crying | Screaming, constant loud crying |
| Respiration type | Regular routine respiration | Unstable and irregular respiration, sigh | |
| Arms | No muscular rigidity, frequently random arm gestures | Stretched, straight arms, hard or fast extension/flexion | |
| Legs | No muscular rigidity, frequently random leg gestures | Stretched, straight legs, hard or fast extension/flexion | |
| Wakefulness | Silent, sleeping peacefully or calm | Eager, uneasy and unappeasable | |
Cries pain scale
This scale, developed by Krechel and Bildner (1995), evaluates postoperative physiological pain [12]. It works through a system similar to Apgar score. It is used for over 32 weeks of gestational age and postoperative period infants. The lowest obtainable score is 0, while the highest is 10 points. A score of at least 4 points and over indicates pain (Table 3).
Tab. 3. Cries pain scale
| Categories | 1 | 2 | 3 |
|---|---|---|---|
| Crying | No | Loudly | Unstoppable |
| O2 need | No | < %30 | > %30 |
| Increase in vital signs | 10% | %11 - % 20 | more than %21 |
| Appearance | Good | Grimace | Grimace and howling |
| Insomnia | No | Wakes up frequently | Constantly awake |
Flacc Pain Scale
Pain measurement is carried out through evaluation of five behavioural categories developed by Merkel et al. in 1997 [13]. It is used for term, preterm and non-expressive children in the age range of 3 years-7 years (Table 4) [14].
Tab 4. Flacc pain scale
| Categories | 0 | 1 | 2 |
|---|---|---|---|
| Face | No special expression | Frowning, souring face | Grimace, clenching |
| Legs | In normal position | Stretched, disturbed | Kicking here and there |
| Activity | Calm | Roll back and forth | Twirling like a bow, tossing |
| Crying | No | Howling | Crying screaming aloud |
| Consolability | Comfort | Consoling by hugging and touching | Inconsolable |
Nursing practices and voice applications in pain management of neonates
Music has been accepted as a way of therapy for centuries [15 ]. It is believed that music is used in therapy because it affects people in many aspects and it is easy to use [16].
Music therapy is defined as “the use of music and/or musical elements (rhythm, sound melody) designed and used by a trained music therapist to optimize and improve the quality of life of a person, family or group” by the World Federation of Music Therapy [17].
Pythagoras (585 BC-500 BC) was one of the first founders of music therapy. Research has been conducted on treatment of psychiatric patients by playing rhythmic sounds. Plato (400 BC) pointed that music ensures tolerance and comfort in people [18]. In his work Kitabu-s Sifa (The Book of Healing), Avicenna referred to music in medical field as “one of the most effective ways of treatment is to increase the mental and spiritual powers of the patient, to give him/her the courage to fight the disease better, to make him listen to the best music and to bring him together with the people he loves” [19].
Nightingale described music therapy in the 1800s as a nursing initiative that increased patient comfort by reducing pain and anxiety [16]. Today, it is frequently used in the treatment of pain and anxiety particularly among the symptoms that occur in other interventional diagnosis-treatment phases applied to patients in intensive care, psychiatry, surgery, pediatrics, obstetrics, and oncology chemotherapy stage [20].
In a study that evaluated 29 research results, music was used to reduce pain and anxiety in patients, to eliminate the side effects of treatment and to increase patient satisfaction [21]. Loewy et al. (2013) examined the effect of music on 272 premature infants and found that their heart rate decreased, while their sleep patterns and milk absorption increased through music therapy [22]. Clacatera et al. (2014) played musical sounds to 42 infants hospitalized in the pediatric surgery unit and found a positive change in their cardiac parameters with reduced perception of pain. The mother’s heartbeat sound and voice were used for the pain relief in neonates and found to be effective [4]. In an RCT study conducted with 60 premature infants, the oxygen saturation value of 30 infants who listened to music during peripheral central venous catheter insertion increased, and heart rates and pain scores decreased compared to the control group. Another RCT study, using white noise, the PIPP score, heart rate and respiratory rate decreased, while oxygen saturation value increased [7]. In an RCT study that listened to heart rate, there was an increase in SpO2 value and a decrease in PIPP pain score of the experimental group [8]. Nine RCT studies on heel lance and circumcised infants found that pain responses reduced in infants who listened to music [23]. In another RCT study, the study group listened to white noise while the control group did not. The study results showed that the level of pain in the infants in the control group was significantly higher than in the study group [5]. In another study conducted on 60 preterm infants in the neonatal intensive care unit, the study group had listened to music for 30 minutes twice a day for seven days. There was a significant difference in physiological parameters of the study group and the control group with an increase in SpO2 level and decrease in respiratory rate and in heart rhythm [24].
This study aimed to determine the current nursing practices for the elimination of infants’ pain and to update the future practices so that nurses can develop a professional care in the pain care of neonates.
Method
The research is a systematic review.
Population and sample of the research
The population of our study consisted of randomized controlled studies published between 2002 and 2022 that examined the effect of voice application on pain in premature infants.
Data collection
We reviewed the electronic databases of Google Akademik,ULAKBİM, Clinical Key, DynaMed, Elsevier, Ebsco, Asos Index, HiperKitap, ProQuest, Sage Premier Journals, Science Direct, Scopus, Springer Nature, Turcademy, Web of Science for the present study
Data collection process
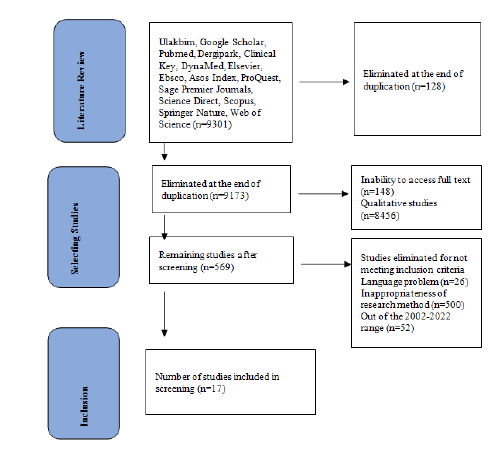
The MeSH (Medical Subjects Headings) system was used to determine the keywords. These keywords, prepared in Turkish and English were as follows: “premature”, “pain”, “music”, “white noise”, ‘‘lullaby’’, “agrı”, “muzik”, “beyaz gurultu”, “ninni’’, ‘‘anne sesi’. The keywords were searched in combinations in the keywords, title and abstract parts. The articles accessed by such screening were included in the study. This process was ended on January 1, 2022 accessing 9301 articles and including 17 of them in the study. The elimination phases of the studies are indicated in the PRISMA (Preferred Reporting Items for Systematic Reviews and MetaAnalyses) 2020 flow diagram (Figure 1).
Figure 1: PRISMA 2009 Flow Diagram
Coding the study
The coding form was created by the researcher and consisted of seven sections, including author/year, country/city, research aim, research method/randomization, sample, intervention and study results. The coding was done using Microsoft Office Word.
Ethics
The literature was reviewed and studies were found as the research was a systematic review. Therefore, no ethics committee approval was obtained because it was not necessary.
Limitations of the study
The studies were selected through participants (P: Population), interventions (I: Interventions), comparison groups (C: Comparators), results (O: Outcomes) and research methods (S: Study Designs)
• Population: Infants born before the week 37.6.
• Interventions: Voice application to the infant.
• Comparator: Infants in the control group.
• Physical vital signs (pulse, saturation, respiratory rate, etc.) and pain assessment scales (PIPP, NIPP).
• Studies with randomized control groups.
Inclusion Criteria:
• Written in Turkish or English
• Being published between 2002 and 2022
• Inability to access full text of the studies
• Using the RCT methodology
Exclusion criteria:
Congress declarations, non-experimental studies and qualitative studies.
Reporting
The systematic review and meta-analysis control list of PRISMA published in 2020 was used in the study
Findings
With the keywords determined, a total of 9301 studies were accessed between 2002 and 2022 through the screening in 16 databases. Of these studies, 128 were eliminated due to duplication,148 were not in full text, 8456 were qualitative studies, 26 did not have language compatibility, 500 were not suitable for the method and 52 were out of the specified year range, thus the study group was created with the remaining 17 studies.
The sample group of 17 studies included in the systematic review consisted of preterm infants. The sample size ranged from a minimum of 25 to a maximum of 206. All studies selected were RCT studies. Table 4.1 shows detailed features of the studies and the detailed coding table that shows the study results (Table 5).
Tab. 5. Coding tables of the studies included in the study
| Author/Year | Country/City | Research Aim | Research Method/Randomization | Sample | Intervention | Study Results |
|---|---|---|---|---|---|---|
| Ren et al., 2022 | China | To examine the effects of white noise on cortical response due to pain, pain score, and behavioral and physiological parameters in newborns with procedural pain. | A randomized controlled trial | Sample: 60 | The radial artery was randomly assigned to listen to white noise at 50 db (experimental group) or 0 db (control group) two minutes before blood sampling. Cortical response due to pain was measured by regional cerebral oxygen saturation (rScO2) monitored by near- infrared spectroscopy, and facial expressions and physiological parameters were recorded by two video cameras. | During artery puncture, the mean rScO2, HR and SpO2 did not show difference between the groups. After the needle was taken, there was no significant difference in the rScO2, PIPP-R score, and trends for facial expression’s tendency to return to the reference line. The white noise intervention did not show a beneficial impact on pain. |
| Double blind | Experimental group: 29 | |||||
| Control group: 31 | ||||||
| Yu et al., 2022 | Taiwan | To analyze the efficiency of maternal voice in relieving pain during heel lance of premature infants and in facilitating mother- infant bonding during hospitalization. | RCT | Sample: 64 | Audio recordings of a mother reading a children’s book were created and then played for the infant during the heel lance once a day for three days in a row. Heart rate, respiratory rate, oxygen saturation and pain response were evaluated before, during after the intervention. | One minute after the intervention, heart rate (p<.001) and Neonatal Infant Pain Scale score (p<.001) were lower in the intervention group than in the control group. The intervention carried out with the mother’s voice slowed the heart rate and relieved the pain response of the premature infants. |
| Experimental group: 32 | ||||||
| Control group: 32 | ||||||
| Sharara-Chami et al., 2022 | Lebanon | To examine the effect of the adding music on pain besides the administration of combined analgesic to the infants to be circumcised. | RCT | Sample: 206 | The infants were videotaped during the intervention to assess pain by double blind and independent reviewers (face and body). | The intervention group had a significantly higher mean heart rate and increased crying time than the control group (p=0.00). Playing music sound from an Ipad in the operation room did not reduce pain during circumcision. |
| Double blind | Experimental group: 103 | |||||
| Control group: 103 | ||||||
| Karadag et al., 2022 | Turkey | To examine the effect of simulation heartbeat nest use on vital signs, pain level and comfort in preterm. | RCT | Sample: 52 | The experimental group infants were observed in their nest for 15 minutes with a heart rate device and the control group was observed for 15 minutes without any device. The heart rates and oxygen saturation were recorded. | During the intervention, the SpO2 value increased significantly (p<0.003) while the PIPP score (p=0.001) decreased in the experimental group. |
| Experimental group: 25 | ||||||
| Control group: 27 | ||||||
| Dora and Tural Buyuk, 2021 | Turkey | To examine the effect of white noise and lullabies on pain perception and vital signs of premature infants during painful interventions. | RCT | Sample: 66 | Heart rate, respiratory rate and oxygen saturation were measured and recorded before, during and after the intervention and post- procedure pain was evaluated using the PIPP. | Premature infants in the white noise group had the lowest mean PIPP score, mean heart rate and respiratory rate, and highest mean oxygen saturation rate (p<0.001). The white noise and lullabies played to premature infants during blood collection were effective in reducing pain and the pain score was lower in the white noise group than in the lullaby group. |
| Experimental group (white noise): 22 | ||||||
| Experimental group (lullaby): 22 | ||||||
| Control group: 22 | ||||||
| Sarhangi et al., 2021 | Iran | To examine the effect of the mother’s heartbeat sound on physiological parameters and pain intensity after blood sampling in neonates in the intensive care unit. | RCT | Sample: 60 | The experimental group listened to the mother’s heartbeat sound until 10 minutes ago 10 minutes after arterial blood samples were taken. The pain intensity was measured in three steps every 10 minutes using the NIPS 10 minutes before, immediately after, and 10 minutes after the intervention. | It had significant moderate to major effects on oxygen saturation and respiratory rate immediately after and 10 minutes after the intervention. Also, it had a major effect on heart rate immediately after the intervention (p<0.05). Furthermore, the intervention had significant moderate to major effects on pain intensity immediately after blood sampling and 10 minutes later (p<0.05). |
| Experimental group: 30 | ||||||
| Control group: 30 | ||||||
| Sener Taplak and Bayat, 2021 | Turkey | To examine the effect of breast milk odor, white noise and facilitated tucking on pain and physiological parameters during the endotracheal aspiration (EA) procedure. | RCT | Sample: 86 | Infants under mechanical ventilation were given breast milk odor, white noise and facilitated tucking and their effect on pain was determined. | White noise and facilitated tucking were found to be more effective in relaxing infants before the EA procedure (p<0.05). There was no significant difference between the groups in pain reduction during EA procedure (p>0.05). |
| Experimental group (breast milk odor): 22 | ||||||
| Experimental group (white noise): 21 | ||||||
| Experimental group [facilitated tucking]: 21 | ||||||
| Control group: 22 | ||||||
| Barandouzi et al., 2020 | Iran | To investigate the analgesic effects of sucrose, music and their combination on pain when opening vascular tracts in preterm neonates. | RCT | Sample: 128 | Two minutes before establishing vascular access, 0.5 ml oral 24% sucrose was given to the sucrose and combination groups. The combination group listened to the same lullaby as the music group. | Pain scores during vascular access procedure were significantly lower in the sucrose and combination groups compared to the control group, but not in the music group (p=0.003, p<0.001, respectively). Thirty seconds after the vascular access procedure, the pain score in three intervention groups (sucrose, music and combination groups p<0.001, p=0.009 and p<0.001, respectively) was significantly lower than in the control group. |
| Double blind | Experimental group (sucrose) 33 | |||||
| Experimental group (music) 33 | ||||||
| Experimental group (sucrose-music): 31 | ||||||
| Control group: 31 | ||||||
| Kahraman et al., 2020 | Turkey | To examine the effects of three auditory interventions (white noise, recorded maternal voice and MiniMuffs during heel lance) on pain and comfort in premature infants in neonatal intensive care units. | RCT | Sample: 64 | During the heel lance, lancet was performed using a 19- gauge with incision depth of 1.1 mm in experimental groups. Sound interventions were performed five minutes before the intervention from a distance of 30 cm. | White noise, recorded maternal voice and the mean oxygen saturation in the MiniMuffs group were higher than in the control group. The heart rate, crying time, mean NIPS score and recorded maternal voice were significantly lower than the MiniMuffs groups control group (p<0.001). |
| Experimental group (white noise): 16 | ||||||
| Experimental group (recorded mother’s voice): 16 | ||||||
| Experimental group (MiniMuffs): 16 | ||||||
| Control group: 16 | ||||||
| Tekgunduz et al., 2019 | Turkey | To examine the effect of oral glucose and lullaby to reduce pain in preterm infants supported with nasal continuous positive airway pressure | Randomized Controlled trial | Sample: 106 | The experimental groups were applied music and glucose during the insertion and removal of the tracheal tube. PIPP score was evaluated during and post-intervention. | Evaluation of the pain intensity of preterm infants post- intervention showed that preterm infants in the lullaby and glucose groups had reduced pain and those in the control group had more pain (p<0.05). |
| Experimental group (lullaby): 35 | ||||||
| Double blind | Experimental group (glucose): 35 | |||||
| Control group: 37 | ||||||
| Uematsu and Sabue, 2018 | Japan | To examine the effect of music (Brahms lullaby) and nonnutritious sucking on heel lance in preterm infants. | RCT | Sample: 25 | The intervention in the experimental groups took place at the beginning of the intervention and lasted until 5 minutes after it began. | The mean PIPP (3.6 to 2.4) of infants during the intervention was significantly lower than the standard care duration (8.0 to 4.6) in all 10 measurement points done every 30 seconds after heel lance (p=.0039 and p<0.0001). |
| No blinding was performed. | Experimental group: 15 | |||||
| Control group: 1000 | ||||||
| Tang et al., 2018 | China | To examine the application of a music intervention (MI) during insertion procedures of peripherally inserted central catheter (PICC) in premature infants. | RCT | Sample: 60 | The MI was performed for 10 minutes before and after the intervention from the music player set at a distance of 30 cm. The sound level was set as 50-60 dB. | During PICC placement, there was a significant increase in blood oxygen saturation (p<0.05) and a decrease in heart rate (p<0.05) and cortisol accumulation in the intervention group receiving music compared to the control group. In addition, MI significantly reduced the pain score and the time required for PICC placement in the MI group compared to the control group. |
| Experimental group: 30 | ||||||
| Control group: 30 | ||||||
| Kuçuk Alemdar, 2018 | Turkey | To examine the effect of maternal voice recorded during the opening of the peripheral vascular access procedure, the breast milk odor and the incubator cover on pain and comfort, in preterm infants. | RCT | Sample: 136 | In the breast milk group, breast milk taken from the mothers was spilled into a sponge and put 5 cm away from the infants. The mother’s voice was played to the babies at a level of 45dB during the intervention and until 15 minutes after the intervention. As an incubator cover, a special white cover was used. In the control group however, routine procedures were applied. | Although there was no significant difference between PIPP scores of the control and intervention groups before peripheral vascular access procedure (p>0.05), a significant difference was found during and after the intervention (p<0.05). |
| Experimental group (mother’s voice): 34 | ||||||
| Experimental group (breast milk odor): 33 | ||||||
| Experimental group (incubator cover): 35 | ||||||
| Control group: 34 | ||||||
| Kuçuk Alemdar and Kardas Ozdemir, 2017 | Turkey | To examine the effect of covering the eyes and playing of intrauterine sounds on pain and physiological parameters of premature infants during establishment of vascular access. | RCT | Sample: 94 | While the intrauterine sound group was given sound at a level of 45dB, the closed eyes group’s eyes were closed 15 minutes before the intervention and kept closed for up to 15 minutes after the intervention. No intervention was made to the control group. | It is reported that covering the eyes of preterm infants during vascular access positively affects their pain scores after intervention. |
| Experimental group (intrauterine): 32 | ||||||
| Experimental group (closing eyes): 32 | ||||||
| Control group: 30 | ||||||
| Shah et al., 2017 | Australia | To examine the trial of music, sucrose and combination therapy to relieve pain during heel lance in neonates. | RCT | Sample: 35 | Every newborn went through all three interventions randomly during consecutive heel lance. A video camera in silent mode recorded facial expressions starting two minutes before to seven minutes after the heel lance. The videos were then analyzed once per minute by two independent evaluators, who were blind to the intervention, using the PIPP revised scale. | The PIPP revised scores were significantly lower at all time points after the combination therapy compared to the groups applied only music or sucrose. There was no difference between the PIPP revised scores of the music and sucrose groups. |
| Blind cross randomized | Experimental group: 35 | |||||
| Qiu et al., 2017 | China | To examine the effect of combined music and touch intervention (CMT) on pain response in premature infants. | RCT | Sample: 62 | Painful interventions in the infants hospitalized for two weeks were recorded. Of the 3707 painful interventions, 1913 were applied to the control group and 1794 were applied to the experimental group. There was no significant difference between these painful interventions. During these entries, the experimental group received combined music and touch intervention, while the control group received standard care. | CMT can significantly improve the concentration of β-endorphins and reduce the pain response of preterm neonates. |
| Experimental group: 30 | ||||||
| Control group: 32 | ||||||
| Kuçukoglu et al., 2016 | Turkey | To examine the effect of white noise in relieving procedural pain arising from vaccination in premature infants. | RCT | Sample: 75 | Premature infants in the study group were exposed to white noise using MP3 players placed next to their cradles one minute before vaccination. The white noise continued until one minute after vaccination. | Pain level of the control group (PIPP ¼ 14.35 ± 2.59) was significantly higher than that of the study group (PIPP ¼ 8.14±3.14) (p<0.05). The white noise was found to be effective. |
| Experimental group: 35 | ||||||
| Control group: 40 |
Of the studies obtained, 46.9% were conducted in Turkey, 17.7% in China, 11.8% in Iran, 5.9% in Taiwan, 5.9% in Lebanon, 5.9% in Japan and 5.9% in Australia. While 58.8% of the studies used a single voice and a single experimental group, 41.2% used more than one voice and experimental group.
In total, there were 19 voice applications in 28 experimental groups. Of the sound interventions used, 26% were white noise, 16% were mother’s voice, 21% were lullabies, 10.7% were heartbeats, 21% were music and 5.3% were intrauterine sounds. While the positive effect rate in voice interventions was found to be 88.2%, the studies that were negative or had no effect were determined as 11.8%.
Discussion
This study was conducted to reach scientific generalizations about the use of voice interventions in pain in premature infants in order to examine their effect on pain in premature infants by synthesizing the findings of RCT between 2002 and 2022. The results of 17 studies were included in the discussion of the study
Considering publication years of the studies included in this research, most studies have been conducted in 2022, followed by the year 2021 and others (Table 5). The reason that there have been more studies recently can be the desire to support pain management in premature infants using non-pharmacological methods.
Three studies in voice interventions applied to the experimental groups among the included research showed no benefit in pain reduction [25-27 ]. Sharara-Chami et al. (2022) played music besides analgesic administration given to infants to be circumcised. In this research with 206 samples, there were 103 experimental groups [25]. The infants were subject to pain assessment of two blind and independent observers. An increase was found in heart rate and crying time of the experimental group. However, the played music did not affect pain. In another study by Ren et al. (2022), white noise was given during radial artery blood sampling [26]. From the sample group of 60 people, the experimental group of 29 people listened to white noise at 50 dB and the control group at 0 dB. There was no difference in pain levels between the two groups during and after the intervention. Therefore, white noise did not have any effect on pain. Sener Taplak and Bayat (2021) conducted a study examining the effect of the breast milk odor, white noise and facilitated tucking on pain and physiological parameters during EA in infants under mechanical ventilation [27]. The sample group was divided into 22, 21 and 21, respectively and control group. Infants who underwent white noise and facilitated tucking were found to be more effective at relaxation before the EA intervention than the other groups. However, no difference was found between the groups in pain reduction.
In 14 studies included in our research, voice applications applied to the experimental groups were found to be have positive effects on pain [4 -8, 28-35]. Sound interventions applied to experimental groups in the studies that our research included simulation of the heartbeat, maternal heartbeat, maternal voice, white noise, lullaby, music and intrauterine sounds.
In the study conducted by Karadag et al. (2022), heartbeat simulation was applied to the experimental group. The PIPP score showed a significant result in the control group (p=0.001) [8]. In a study conducted by Sarhangi et al. (2021), the experimental group listened to their mother’s heartbeat during blood collection. In pain assessment measured immediately after the intervention and 10 minutes later, there was a significant result compared to the control group (p<0.05). In their study, Kuçuk Alemdar and Kardas Ozdemir (2017) played intrauterine sounds to the experimental groups [31,34]. There was a significant difference after the NIPS pain assessment (p<0.05).
Yu et al. (2022), Kahraman et al. (2020) and Kuçuk Alemdar (2018) played mother’s voice to the experimental groups [28, 31, 34]. In these studies, there was a significant difference in the results of pain assessment in the experimental groups versus control groups (p<0.001, p<0.001 and p<0.05, respectively) [6].
Dora and Tural (2021), Kahraman et al. (2020) and Kuçukoglu et al. (2016) used white noise as sound intervention in their studies. They found that pain decreased after the intervention applied in the experimental groups (p<0.001, p<0.001 and p<0.05, respectively) [5-7].
Barandouzi et al. (2020), Tang et al. (2018), Uematsu and Sabue (2018), Qiu et al. (2017), and Shah et al. (2017) played music to the experimental groups [29,32,33,35-37]. The results from their studies showed a significant difference in pain scores of the experimental groups compared to the control groups (p=0.009, p<0.05, p<0.0001, p<0.05 and p<0.05, respectively).
Dora and Tural (2021), and Tekgunduz et al. (2019) played lullaby to the experimental groups as sound intervention. There was a significant difference in pain scores of the groups listening to lullaby compared to the groups that did not listen (p<0.001 and p<0.05, respectively) [ 7,30].
Conclusion
We found 9301 studies related to our topic and published between 2002 and 2022 examining the effect of voice interventions on pain in premature infants. Upon elimination, a total of 17 studies using RCT method were included in our research. In three of these studies, voice intervention did not give positive results on pain, while in 14 of them gave positive results. In premature infants, voice applications had a positive effect on pain with a rate of 82.3%. Besides pain assessment, positive results were obtained with the increase in SpO2 value, stabilization in heart rate, decrease in respiratory rate and shortening of crying times. However, meta-analysis studies should be conducted to clearly deem sound applications positive or negative.
Pain management is pointed as one of the independent tasks of a nurse. Therefore, the nurse should evaluate the severity of the infant’s pain, and plan and implement pharmacological and non-pharmacological pain management strategy developed with the health team. Among non-pharmacological pain procedures, there are a limited number of evidence-based studies for voice interventions (music, lullaby, white noise, mother voice, etc.). The results of the current study can be considered an evidence-based study in pediatric nursing and can contribute to its use in nonpharmacological pain management.
Suggestions
• The frequency of studies with much evidence can be increased. Further double blind studies can be conducted.
• Sample size can be increased.
• Multi-centred studies can be carried out.
Acknowledgements
The research received no external or grant funding. All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by G.M., O.T. and G.M., O.T., and P.U. participated in conceiving the design of the study, collecting the data and the data analysis The first draft of the manuscript was written by O.T., and supervision was made by G.M., and P.U. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. The authors have declared that they have no competing or potential conflicts of interest.
References
- Walker SM. Neonatal pain. Ped Anes 2014; 24:39- 48.
- Collados-Gómez L, Camacho-Vicente V, González-Villalba M, Sanz-Prades G, ve Bellón- Vaquerizo B. Neonatal nurses’ perceptions of pain management. Enfer Intens, 2018;29:41-47.
- Eroglu A, Arslan S. Perception, evaluation and management of neonatal pain. Duzce Univ J Heal Sci Inst, 2018;8:52-60.
- Sarhangi F, Azarmnejad E, Javadi M, Tadrisi SD, Rejeh N, et al. The effect of the mother’s heartbeat sound on physiological parameters and pain intensity after blood sampling in neonates in the intensive care unit: A randomized controlled clinical trial. J Neon Nurs, 2021;27:123-128.
- Kuçukoglu S, Aytekin A, Celebioglu A, Celebi A, Caner Ä° et al. Effect of white noise in relieving vaccination pain in premature infants. Pain Mana Nurs 2016;17:392- 200.
- Kahraman A, Gumus M, Akar M, Sipahi M, Bal Yılmaz H, et al. The effects of auditory interventions on pain and comfort in premature newborns in the neonatal intensive care unit; a randomized controlled trial. Intensive and Critical Care Nursing, 2022;61.
- Dora O, Buyuk ET. Effect of white noise and lullabies on pain and vital signs in ınvasive ınterventions applied to premature babies. Pain Management Nursing, 2021;22:724-729.
- Karadag OE, Kerimoglu Yildiz G, Akdogan R, Yildiz S, Hakyemez Toptan H. The effect of simulative heartbeat nest used in preterm new-born on vital signs, pain, and comfort in Turkey: A randomized controlled study . J Pedia Nurs, 2022;62: e170-e177.
- Akcan E, Yigit R. Turkish reliability ve validity study of premature ınfant pain profile. Fır J Heal Sci 2015;29:97-102.
- Lawrence J, Alcock D, McGrath P, Kay J, MacMurray SB, Dulberg C. The development of a tool to assess neonatal pain. Neon net 1993; 12:59-66.
- Akdovan T, Yıldırım Z. Evaluation of pain in healthy newborns, examining the effect of pacifier giving and cuddling. J Perin. 1999; 7:107-107.
- Krechel SW, Bildner J. CRIES: a new neonatal postoperative pain measurement score. Initial testing of validity ve reliability. Pedia anes, 1995;5:53-61.
- Merkel SI, Voepel-Lewis T, Shayevitz JR, Malviya S. The FLACC: A behavioral scale for scoring postoperative pain in young children. Ped nurs, 1997;23:293-297.
- Emir S, Cin S. Pain in children: assessment and approach. Ankara Uni Fac Med J, 2004:57:153-160.
- Lok N ve Bademli K. The effectiveness of music therapy in Alzheimer's patients: systematic review. Current Appr Psych, 2016;8:266-274.
- Tagtekin Sezer B. What do we know about musicotherapy? Konur Med Jour 2015;7:167-171.
- Cigerci Y, Kurt H, Çelebi S (2016). Opinions of health professionals about music therapy, which is a complementary care and alternative treatment method. J Acad Music Stud, 2016;2:13-26.
- Birkan I. The history of music therapy and its applications. Ankara Journal of Acupunc Comp Med 2014;1:37-49.
- Koç E. Nourishing your soul and body: music and medicine from past to present. Konuralp Med J, 2016;8:51-55.
- Imseytoglu D, Yıldız S. Music therapy in neonatal intensive care units. Istanbul Univers Flor Nightin Nurs J, 2012;20:160-165.
- Parlar Kilic S, Karadag G, Oyucu S, Kale O, Zengin S, et al. Effect of music on pain, anxiety, ve patient satisfaction in patients who present to the emergency department in turkey. Japan J Nurs Sci, 2014;12:44-53.
- Loewy J, Stewart K, Dassler AM, Telsey A, Homel. The effects of music therapy on vital signs, feeding and sleep in premature infants. Pediatrics, 2013;131:902-918.
- Bellieni, CV, Tei M, Coccina F, Buonocore G. Sensorial saturation for infants pain. J Mat-Fet Neo Med 2012; 25:79-81.
- Sasikala T, Kamala S. Therapeutic effects of music therapy on preterm neonates-pilot study report. Int J Nurs Edu Res, 2016;4: 42-44.
- Sharara-Chami R, El-Hout Y, Lakissian Z, Hafez B, Abi-Gerges C, et al. Music as an adjunct to combination analgesia for neonatal circumcision: A randomized controlled trial. J Pedia Urol 2022;18: 184.e1-184.e6.
- Ren X, Li L, Lin S, Zhong C, Wang B. Effects of white noise on procedural pain-related cortical response and pain score in neonates: A randomized controlled trial. Int J Nurs Sci 2022;9:269-277.
- Taplak AS, Bayat M. Comparison the effect of breast milk smell, white noise and facilitated tucking applied to turkish preterm ınfants during endotracheal suctioning on pain and physiological parameters. J Pedi Nurs 2021;56:e19-e26.
- Yu WC, Chiang MC, Lin KC, Chang CC, Lin KH, et al. Effects of maternal voice on pain and mother-Infant bonding in premature infants in Taiwan: A randomized controlled trial. J Ped Nurs 2022;63:e136-e142.
- Barandouzi ZA, Keshavarz, M, Montazeri, A, Ashayeri, H, Rajaei, Z (2020). Comparison of the analgesic effect of oral sucrose and/or music in preterm neonates: A double-blind randomized clinical trial. Comp Ther Med. 2020;48:102271.
- Tekgunduz KS, Polat S, Gurol A, Apay SE. Oral glucose and listening to lullaby to decrease pain in preterm ınfants supported with ncpap: a randomized controlled trial. Pain Mana Nurs 2019;20:54-61.
- Alemdar DK. Effect of recorded maternal voice, breast milk odor, and incubator cover on pain and comfort during peripheral cannulation in preterm infants. Appl Nurs Res 2018; 40:1-6.
- Tang L, Wang H, Liu Q, Wang F, Wang M. Effect of music intervention on pain responses in premature infants undergoing placement procedures of peripherally inserted central venous catheter: A randomized controlled trial. Eur J Integ Med 2017;105-109.
- Uematsu H, Sobue I. Effect of music (brahms lullaby) and non-nutritive sucking on heel lance in preterm infants: A randomized controlled crossover trial. Paed Child Hea. 2019;24: E33-E39.
- Alemdar DK, Ozdemir FK. Effects of covering the eyes versus playing ıntrauterine sounds on premature ınfants′ pain and physiological parameters during venipuncture. J Pedia Nurs. 2017;37:e30-e36.
- Qiu J, Jiang YF, Li F, Tong QH, Rong H, et al. Effect of combined music and touch intervention on pain response and β-endorphin and cortisol concentrations in late preterm infants. BMC Pediatr 2017;17:1-7.
- Shah SR, Kadage S, Sinn J. Trial of music, sucrose, and combination therapy for pain relief during heel prick procedures in neonates. J Pedia 2017;190:153-158.e2.
- Akcan E, Polat S The role of the nurse in pain and pain management in newborns. J Acıb Uni Heal Sci 2017;2;64-69.