Case Report - Onkologia i Radioterapia ( 2023) Volume 17, Issue 5
Sister mary joseph's nodule: An important physical finding
Parit Cai*, Joviale Christelle Maffo, Mbachan Masoeli Takere and Elroy Patrick WeledjiParit Cai, Department of Radiotherapy, Fudan University, Shanghai, China, Email: Paritke081@sina.com
Received: 10-Nov-2022, Manuscript No. OAR-22-79434; Accepted: 01-May-2023, Pre QC No. OAR-22-79434 (PQ); Editor assigned: 14-Nov-2022, Pre QC No. OAR-22-79434 (PQ); Reviewed: 11-Apr-2022, QC No. OAR-22-79434 (Q); Revised: 27-Apr-2023, Manuscript No. OAR-22-79434 (R); Published: 04-May-2023
Abstract
Background: Sister Mary Joseph’s nodule is a rare but important physical pending as it is a sign of an advanced stage of malignancy.
Case presentation: This is a case of an apparently clinically well but immune- deficient 62-year-old African woman whose main complaint was an enlarging violaceous discharging umbilical nodule. A focused history and physical examination complemented by an abdominal Computerized Tomography (CT) scan was sug-gestive of an umbilical cutaneous manifestation (Sister Mary Joseph’s nodule) of an underlying disseminated ovarian malignancy. This was confirmed histologically by an excision biopsy of the umbilical nodule.
Conclusion: Sister Mary Joseph’s nodule is an important differential diagnosis for an umbilical nodular lesion as it is a sign of advanced malignancy with a generally poor prognosis.
Keywords
Computerized Tomography (CT); Sister Mary Joseph (SMJ); Human Immunodeficiency Virus (HIV); Magnetic Resonance Imaging (MRI); Paraneoplastic syndromeAbbreviations
SMJ: Sister Mary Joseph HIV; Human immunodeficiency virus; HAART: Highly Active Antiretroviral Treatment
Introduction
Sister Mary Joseph (SMJ) nodule is an eponymous term referring to a malignant umbilical nodule. It was first described in the literature in 1864 and, was named after Sister Mary Joseph Dempsey (1851–1939) a surgical assistant to Dr. William James Mayo who first noticed the association between abdominopelvic malignancies and metastatic umbilical nodules. It is a rare but important physical pending as it is a sign of an advanced stage intra-abdominal malignancy [1]. A clinical presentation of Sister Mary Joseph’s nodule as an umbilical cutaneous manifestation of a disseminated ovarian carcinoma in a Highly Active Antiretroviral Treatment (HAART)-compliant Human Immunodeficiency Virus (HIV) infected patient is reported herein [2].
Case Presentation
A 62-year-old African woman presented at the outpatient clinic with a 4 week history of a rapidly progressing umbilical nodular lesion that was associated with some discomfort and a clear fluid discharge. She felt generally well except for gradual weight loss and anorexia in the past months [3]. She was an Human Immunodeficiency Virus (HIV) infected patient but compliant to Highly Active Antiretroviral Treatment (HAART). On examination she was thin and listless with abdominal bloatedness and discomfort. The abdomen was tense and with a shifting dullness on percussion suggestive of ascites and, a tender 5 cm hepatomegaly. She had a violaceous non-tender 4 cm umbilical nodule which was firm in consistency and irreducible [4]. The working diagnosis of an SMJ nodule with an underlying intrabdominal malignancy was made
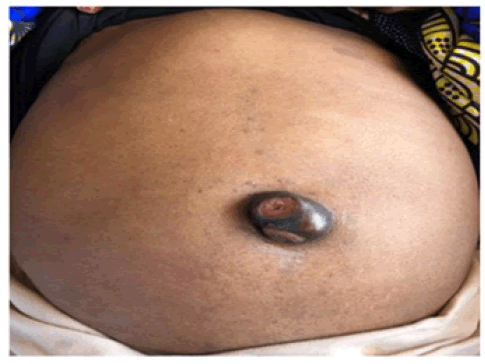
The differential diagnosis included a complicated umbilical or paraumbilical hernia being not reducible and had no associated cough impulse, a primary umbilical neoplasm which may be indistinguishable from a SMJ nodule, umbilical endometriosis but occurs in females of reproductive age and presents with a bleeding umbilical nodule especially during menstruation, a pyoderma gangrenosum but typically associated with inflammatory bowel disease, rheumatoid arthritis and myeloproliferative disorders (Figure 1) [5]. A foreign body but usually associated with an identical foreign body, an omphalith and a keloid. Blood tests revealed a microcytic anaemia with a hemoglobin level of 8 g/dl. A Computed Tomog-raphy (CT) contrast scan of the abdomen and pelvis demonstrated a large ovarian tumour, an umbilical nodule measuring 4 cm in diameter, some ascites and, segment IV liver metastases (Figure 2). She underwent an excision biopsy of the umbilical nodule under local anaesthesia [6]. The tumour tapered intraperitoneally, thus allowed a gush of ascitic fluid following its excision. While awaiting a definitive histopathological report the macroscopic appearance was suggestive of a metastatic ovarian adenocarcinoma (Figure 3).
Figure 1: Sister Mary Joseph’s nodule
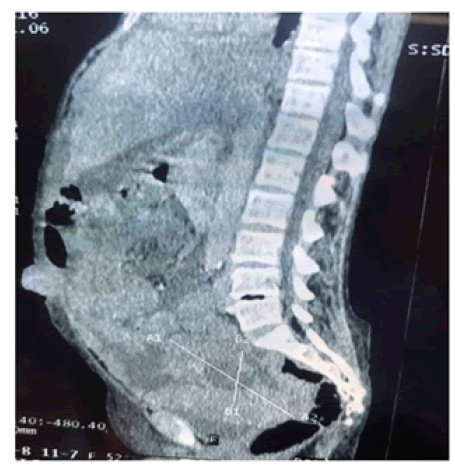
Figure 2: A CT scan of Abdomen demonstrating pelvic tumour and an umbilical nodule.
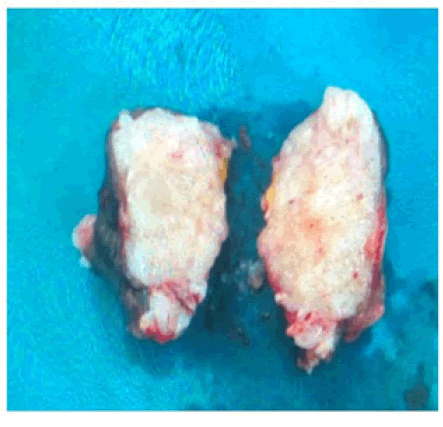
Figure 3: Macroscopic appearance of excised nodule with the consistency of a carcinoma.
Results and Discussion
This case report demonstrated that SMJ nodule although uncommon is a sign of advanced malignancy. Similar umbilical cutaneous metastases from ovarian carcinoma have been reported by Touraud, et al. in 2000, Calongos, et al. in 2016 and Carrey, et al. in 2018 [7]. SMJ nodule is uncommon with an estimated 1–3% cases of abdominopelvic malignancy. Of these 35–65% involves primary carcinomas of the gastrointestinal tract and 12–30% involves genitourinary tract carcinomas. Other reported sites include lung, pancreas, oesophagus, stomach, liver, gallbladder, caecum, breast, uterus, kidney, penis, testicles and prostate. However, the source of the primary neoplasm may not be found in up to 30% of patients [8-10]. The mechanism of metastatic spread to the umbilicus remains unclear but include contiguous, lymphatic or haematogenous spread. It typically presents as an umbilical or paraumbilical nodule with a firm consistency varying in size between 0.5-15 cm [11,12]. The nodule may be painful and discharging fluid and, may be the only complaint by the patient as in this case. Other patients can present in a poor clinical state with additional physical signs such as ascites and pleural effusion [13-15]. A focused history and examination of the chest, abdomen and regional lymph nodes may suggest and reveal the source of the primary neoplasm. Patients who present with SMJ nodule following treatment of a known neoplasm raises the possibility of tumour recurrence, thus acting as part of a paraneoplastic syndrome. Imaging with CT and/or Magnetic Resonance Imaging (MRI) scan will establish the extent of the malignancy (i.e. tumour staging) [16]. Biopsy of the umbilical nod-ule will provide tissue sample for histological diagnosis of the type of malignancy prior to treatment. The management of the disease should take into account patient preference, the clinical state of the patient and the aetiology of the primary malignancy. Palliative treatment may be the only treatment for some patients, whereas carefully selected patients may benefit from more aggressive treat-ment with surgery, chemotherapy and radiotherapy [17,18].
Conclusion
Sister Mary Joseph’s nodule is an important physical pending being a sign of advanced intra-abdominal malignancy with usually a poor prognosis. It is a differential diagnosis to consider in a patient with an umbilical nodule.
Ethics Approval and Consent to Participate
Not required as being a case report.
Consent for Publication
Written informed consent was obtained from the patient for publication of this case report. A copy of this written consent is available for review by the editor-in-chief of this journal.Availability of Data and Materials
Not applicable.
Competing Interests
The authors declare that they have no competing interests.
Funding
None.
Authors' Contributions
EPW is the main author and surgeon, MMT contributed to literature search, JCM referred the patient and contributed to literature search.
Acknowledgement
I acknowledge the nursing staff of the surgical unit of the regional hospital Limbe for the concern and care given to the patient.
References
- Quenu L. Du cancer secondaire de l’ombilic Secondary cancer in the umbilicus. Rev. Chir. 1896; 16:97.
- Tso S, Brockley J, Recica H, Ilchyshyn A. Sister Mary Joseph’s nodule: an unusual but important physical pending characteristic of widespread internal malignancy. Br. J. Gen. Pract. 2013; 63:551–2.
[Crossref] [Google Scholar] [PubMed]
- Touraud JP, Lentz N, Dutronc Y, Mercier E, Sagot P, et al. Umbilical cutaneous metastasis (or Sister Mary Joseph’s nodule) disclosing an ovarian adenocarcinoma. Gynecol. Obstet. Fertl. 2000; 28:719–22.
[Crossref] [Google Scholar] [PubMed]
- Calongos G, Ogino M, Kimita T, Hori M, Moeeeri T. Sister Mary Joseph’s nodule as a first manifestation of a metastatic ovarian cancer. Case. Rep. Obstet. Gynecol. 2016; 1087513.
[Crossref] [Google Scholar] [PubMed]
- Carrey MT, Beru CV, Hage R. Case of Sister Mary Joseph’s nodule in a high grade serous carcinoma. Cureus. 2018; 10:e3757.
[Crossref] [Google Scholar] [PubMed]
- Gabriele R, Conte M, Egidi F, Borghese M. Umbilical metastasis: current view point. World. J. Surg. Oncol. 2005; 3:13.
- Minlescu R, Balaban DV, Sandru F, Jung M. Cutaneous manifestations in pancreatic diseases-a review. J. Clin. Med. 2020; 9:2611.
[Crossref] [Google Scholar] [PubMed]
- Chiang CH, Lim MH. Sister Mary Joseph nodule associated with pancreatic adenocarcinoma. J. Formos. Med. Assoc. 2015; 114:92–3.
[Crossref] [Google Scholar] [PubMed]
- Jain G, Kumar C, Damie N, Kumar M, Ramjan A, et al. Oesophageal squamous cell carcinoma metastatic to umbilicus: A case report with review of literature. J. Gastrointest. Cancer. 2019; 50:1018–21.
[Crossref] [Google Scholar] [PubMed]
- Mangla A, Lu P, Mullane MR, Laid TE. Gastric cancer in a patient with laparoscopic adjustable gastric band: Case report and review of literature. J. Gastrointest. Cancer. 2019; 50:695–8.
[Crossref] [Google Scholar] [PubMed]
- Salemis NS. Umbilical metastasis or Sister Mary Joseph’s nodule as an early sign of an occult ceacal adenocarcinoma. J. Gastrointest. cancer. 2007; 38:131–134.
[Crossref] [Google Scholar] [PubMed]
- Petch S, Sobota A, Abu Saadeh F. Sister Mary Joseph nodule: an unusual site for endometrial cancer metastasis. BMJ. Case. Rep. 2019; 12:e229187.
[Crossref] [Google Scholar] [PubMed]
- Deb P, Rai RS, Rai R, Gupter E, Chander Y. Sister Mary Joseph nodule as the presenting sign of disseminated prostate carcinoma. J. Cancer. Res. Ther. 2009; 5:127–9.
[Crossref] [Google Scholar] [PubMed]
- Mudugul R, Beniwal R, Singh S, Khera S. Violaceous papules and nodules over the umbilicus: The harbinger of occult intraabdominal malignancy. Indian. Dermatol. Online. J. 2020; 11:852–3.
[Crossref] [Google Scholar] [PubMed]
- Dar IH, Kamita MA, Dar SH, Kucha FA. Sister Mary Joseph nodule- a case report with review of literature. J. Res. Med. Sci. 2009; 14:385–7.
[Google Scholar] [PubMed]
- Mun JH, Kim JM, Ko CH, Kim BS, Kim MB. Dermoscopy of a Sister Mary Joseph nodule. J. Am. Acad. dermatol. 2013; 68:e190-2.
[Crossref] [Google Scholar] [PubMed]
- Weledji EP. Weledji’s clinicopathological classification of perianal Paget’s disease. Int. J. Surgery. Short. Reports. 2017; 2:21-3.
- Baillard DH, Mazaheri P, Oppenheimer DC, Lubner MG, Menas CO, et al. Imaging of abdominal wall masses, mass-like lesions and diffuse processes. Radiographics. 2020; 40:684–706.
[Crossref] [Google Scholar] [PubMed]