Original Article - Onkologia i Radioterapia ( 2021) Volume 15, Issue 5
Role of FNAC in the diagnosis of ovarian tumours
Aswathi Krishnan M1*, Sheeja S2 and Lillykutty Pothen22Department of Pathology, Government Medical College, Kottayam, Kerala, India
Aswathi Krishnan M, Division of Oncopathology, Department of Clinical Lab Services and Translational Research, Malabar Cancer Centre, KeralA, India, Tel: 91 906 103 36 44, Email: aswathikm99@gmail.com, sbs.pub@gmail.com
Received: 15-Dec-2020 Accepted: 26-Feb-2021 Published: 15-Mar-2021
Abstract
Fine Needle Aspiration Cytology (FNAC) is a cost effective, minimally invasive technique which is used for diagnosing various non-neoplastic and neoplastic lesions. However, its use is restricted in ovarian cancer diagnosis due to various factors such as difficulty in sub-typing with cytology alone, fear of spillage of tumor cells to peritoneal cavity etc. In this study, we analysed 45 cases of ovarian masses and FNAC of these cases were performed Under Ultrasonography (USG) guidance. Histopathology diagnosis was compared with cytology in all these cases. For statistical analysis, 39 cases were considered. Cytological analysis detected 18 cases as malignant neoplasms and all of them were found to be malignant in histological analysis as well. In the present study, no incidence of cyst rupture or any other complication occurred during the procedure. FNAC is a safe and economic procedure with acceptable diagnostic accuracy especially in the experienced hands. False negative results of FNAC in ovarian cystic lesions were mainly due to the low cellularity of the sample and secondary degenerative changes. This can be avoided to certain extend by preparing cell blocks and hence we suggest the same. The distinction between cystadenocarcinoma and borderline tumours cannot be confidently made by cytology alone. All clinical and sonographic findings should be considered in collaboration with FNAC findings for arriving at a diagnosis.
Keywords
FNAC, ovarian neoplasm, histopathology correlation, ultrasonography guidance
Introduction
Cytological analysis of ovarian neoplasms is still a subject of debate for various reasons. The reasons are intricately related to type, nature and management of ovarian neoplasms. Ovaries have a capacity to give rise to amazingly diverse variety of neoplasms. Histogenesis of individual tumor varies widely and each of the subtypes is derived from different components of the organ. Further-more, the histogenesis of some tumours are still controversial.
With regard to the epidemiological aspects, the statistical data of ovarian neoplasms in India is rather limited [1]. Figure from the western world indicate that the incidence of carcinoma of ovary is on the rise [2, 3].
The degree of aggressiveness is an important aspect in ovarian tumours. This unfavourable outcome is attributed to the lack of early warning symptoms and lack of early diagnostic tests. Approximately 70% of patients presented when this tumor has spread beyond the pelvis [4].
Fine needle aspiration cytology is a simple and reliable method for diagnosing tumours of various organs of the body. It was not well utilized in cases of ovarian tumours because
• Large variety of tumours is difficult to subtype on cytology alone
• Fear of spillage of tumor cells into the peritoneal cavity,
• Inexperience of cytopathologist in interpreting ovarian lesions [5-9].
To over-come these problems, ancillary techniques such as immunocytochemical studies (e.g. inhibin, CA 125, WT1) [10], tumor markers [e.g.CA-125, Carcinoembryonic Antigen (CEA)] [11] in serum or cyst fluid and CT/Ultrasound Doppler findings have been used in conjunction with FNAC. There have been limited studies on FNAC in diagnosis of ovarian cancers.
However there are certain situations where FNAC has an important role to play
• In distinguishing non neoplastic cysts from true neoplasms of the ovary,
• In detecting suspected pelvic recurrences in known cases of ovarian cancers,
• In arriving at a primary diagnosis of ovarian malignancy in patients who have a high risk for surgery
• Patients already having a disseminated disease at presentation
The credibility of FNAC depends on the technique of obtaining material for smears and accuracy of interpretation of smears. The present study was undertaken to elucidate the cytomorphology of various ovarian lesions and explore the diagnostic accuracy by comparing with the subsequent histopathology.
Aims and Objectives
The objectives of the study are to analyse and study the cytomorphology of ovarian lesions and to correlate the findings of cytology smears with that of histopathological findings. It aims to assess the diagnostic accuracy of fine needle aspiration cytology and to identify possible pitfalls in the cytological diagnosis of ovarian lesions.
Materials and Methods
The study was conducted at Kottayam Medical College during the period of April 2008-December 2009 after obtaining necessary permissions from Institutional Ethical Committee at Government Medical College Kottayam on 45 patients diagnosed as having an ovarian mass clinically and/or ultra-sonographically. Serum CA-125 was done by radioimmunoassay in some of the patients. The technique involved aspiration of material from ovarian lesions under ultrasonography guidance using 10 cc disposable syringe and appropriate gauge needle (21 gauge/22 gauge) or lumbar puncture needle.
Air dried smears and wet smears fixed in 95% ethanol were prepared from aspirate. A minimum of 3-4 smears were prepared for each case. Giemsa staining was done on air dried smears while those fixed in alcohol were stained in Papanicolaou’s method.
All cases which showed inflammatory cells only and one which showed mucinous material with benign cells were considered as non-malignant cases. All the 45 patients on whom FNAC of ovary was done underwent surgery in gynecology department of Government Medical College Kottayam. The specimens were received in the department of pathology, Government Medical College Kottayam. Paraffin blocks are prepared after the formalin fixation. . Sections were subsequently stained with Hematoxylin and Eosin. Histopathologic typing of tumors was done according to the WHO classification of ovarian tumors. Cytological diagnosis was compared to the histopathological diagnosis. Sensitivity, specificity, positive predictive value and negative predictive value were calculated.
Obesrvations and Results
A total of 45 fine needle aspirations of ovarian lesions were done during the period of April 2008-December 2009.
Age range varied from 20 years to 90 years with majority of the cases occurring in the 6th decade and mean age was 53 years (Table 1).
Tab. 1. Demographic distribution of patients
| Age | Frequency | Percent |
|---|---|---|
| 20-29 | 4 | 8.9 |
| 30-39 | 4 | 8.9 |
| 40-49 | 10 | 22.2 |
| 50-59 | 12 | 26.7 |
| 60-69 | 11 | 24.4 |
| 70-79 | 3 | 6.7 |
| 90-99 | 1 | 2.2 |
| Total | 45 | 100 |
The table 2 shows the cytological analysis (FNAC) results of the 45 ovarian lesions that were analysed during the study period. 18 cases were malignant and in 20 cases there were only inflammatory cells. 6 cases which showed scanty cellularity and/or blood only were considered as inconclusive. One case showed only a few benign cells in a mucinous background. Cases in which inflammatory cells and only mucinous material with a few benign cells were obtained are included in the non-malignant category.
Tab.2. Result of cytological evaluation of all 45 cases
| FNAC Diagnosis | No: of cases |
|---|---|
| Malignant | 18 |
| Inflammatory cells | 20 |
| Mucinous background with a few benign cells | 1 |
| Inconclusive | 6 |
| TOTAL | 45 |
All the three malignant papillary serous neoplasm showed large sheets and Papillaroid clusters of malignant epithelial cells (Figures 1 and 2). In some smears psammoma bodies (Figure 3) were also seen. Cases in which a diagnosis of malignant epithelial neoplasm was given, the smears showed clusters of highly atypical cells. Papillary formations were not seen.
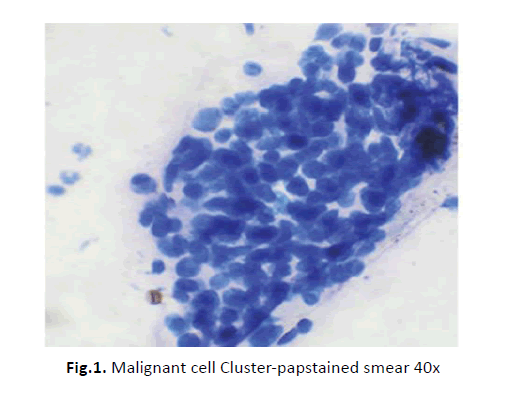
Figure 1: Malignant cell Cluster-papstained smear 40x
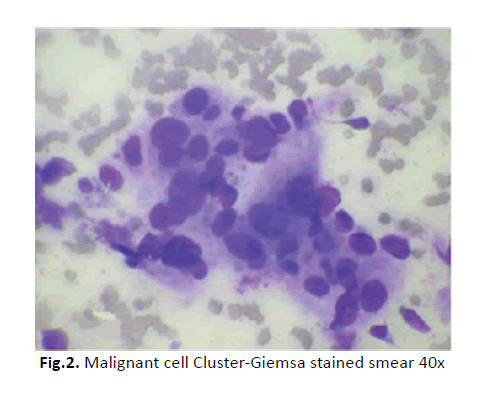
Figure 2: Malignant cell Cluster-Giemsa stained smear 40x
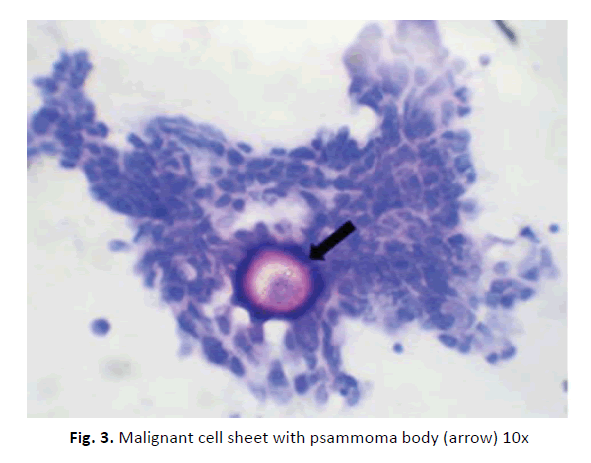
Figure 3: Malignant cell sheet with psammoma body (arrow) 10x
The total 18 cases of malignant neoplasms found during cytological analysis were further sub-classified. All of these cases were found to be malignant in histological analysis also. High grade serous carcinoma (Figures 4 and 5) constituted majority of the cases. The cytology sub-types and corresponding histology sub-types are tabulated in Table 3.
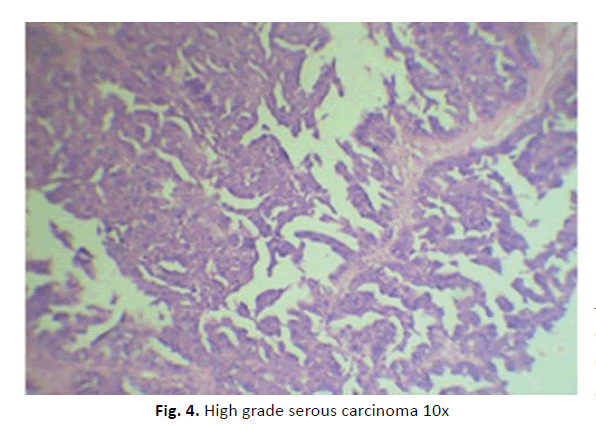
Figure 4: High grade serous carcinoma 10x
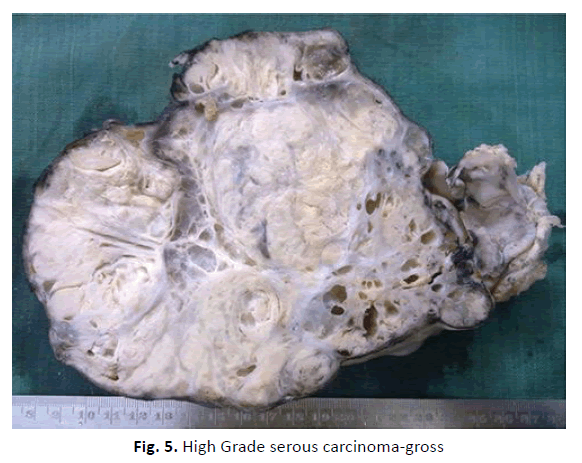
Figure 5: High Grade serous carcinoma-gross
Tab. 3. FNAC sub-classification of malignant cases and corresponding histology sub-types
| Cytology/Histology | Malignant Epithelial Neoplasm | Malignant Papillary Serous Tumor | High Grade Malignant Tumor |
|---|---|---|---|
| High grade serous carcinoma | 10 | 1 | - |
| Endometroid adenocarcinoma | 1 | - | - |
| Residual neoplasm showing poorly differentiated carcinoma | 2 | - | - |
| Residual Neoplasm Showing Papillary Serous Adenocarcinoma | - | 2 | - |
| Transitional Cell Carcinoma | 1 | - | - |
| Germ Cell Tumor | - | - | 1 |
In one case a diagnosis of high grade malignant neoplasm was made. In this case, the neoplastic cells were dis-cohesive with a few clusters. Nuclei were of high grade with most of them showing nucleoli. Necrotic debris was also seen in the background. The patient was 20 years old. Subsequent histopathology showed malignant germ cell tumor-dysgerminoma. During the histological analysis of the 20 cases of FNAC smears that showed only inflammatory cells 11 cases were proven to be benign lesions. Malignant lesions constituted 6 cases. For statistical analysis, 39 cases were considered. Six cases in which inconclusive material obtained were omitted. In the present study 27 malignant neoplasms (including the 3 borderline neoplasms) and 12 nonmalignant lesions were diagnosed in histopathology.
• True positive: Of the 27 malignant neoplasms 18 were correctly diagnosed as malignancy by FNAC.
• True negative: Of the 12 non-malignant lesions 12 cases were diagnosed as non-malignant by FNAC.
• Predicted positive: FNAC predicted 18 of the 39 cases to be positive.
• Predicted negative: FNAC predicted 21 of the 39 cased to be negative
As seen from table 4, the overall diagnostic accuracy of FNAC in this series is 76.9% with a sensitivity of 66.7% and specificity of 100% for detecting malignancy. Statistical tool used was SPSS version 24.
Tab. 4. Statistical results
| Parameters | Value |
|---|---|
| Sensitivity | 66.70% |
| Specificity | 100% |
| Positive predictive value | 100% |
| Negative predictive value | 57.10% |
| Accuracy | 76.90% |
Discussion
In the present study, 45 ovarian lesions were included which were followed up with subsequent histopathology. The study lasted over a period of 18 months from April 2008 to December 2009. In this study the age range of patients with ovarian tumors was 20-90 years, with a mean age of 53 years. Six out of 45 aspirates (13%) were inconclusive. Other studies have reported different frequencies of inadequate smears ranging from 18% to 80% [6,10,12,13]. In the present study, only acellular smears were considered non-diagnostic, whereas other studies have included smears showing only macrophages and or inflammatory cells as inadequate [6, 10]. This probably resulted in a false-negative outcome as the aspirate did not yield any epithelial cells. This is a pitfall of FNAC, as the absence of epithelial cells precludes a correct diagnosis. In another study, 43% of cases were found to be inadequate and these included all types of ovarian cysts, even malignant ones [6].Therefore, it is concluded that in an unsatisfactory sample malignancy cannot be ruled out, and a combination of Ultrasonography findings, clinical features and serum levels of tumor markers should therefore be sought to reach a definitive diagnosis.
Most studies in the literature have centered on the sensitivity, specificity and diagnostic accuracy of benign versus malignant lesions where the non-neoplastic benign lesions are included along with various benign tumors in a single category. In the present study, the diagnostic accuracy of cytology in the pre-operative management of ovarian tumors was studied. The reports in the literature indicate that cytological distinction of benign from malignant ovarian cysts is fraught with variable sensitivity (26%-100%) but high specificity (67%-100%) [14-16]. This extent of variation in sensitivity and specificity may be related to the fact that some studies refer to distinction of follicular cysts from non-follicular cysts [17], others aim for a specific subclassification [14] and still other authors include patients of diverse ages with cysts of varying histological and sonographic types. Also, the pathologist’s experience is variable and rarely stated.
Six cases of benign serous cystadenoma showed only inflammatory cells. In the previous studies, 44%-52.5% of serous cystadenomas were correctly diagnosed [10, 18]. Similar to our observations, in other studies too, serous adenocarcinoma was easily diagnosed on cytology [6, 10, 18]. One case of mucinous cystadenoma showed mucinous material and bland epithelial cells. Other four cases showed inflammatory cells and/or blood only. Sensitivity was 20%. This was similar to some of the previous studies which showed sensitivity of 20%-38% [6, 10]. Even though not a single case of teratoma could be diagnosed by our study, other studies have shown results varying from 30%-100% [5]. Results from previous studies are tabulated in table 5. In the present study, no case of Borderline Ovarian Tumor (BOT) was diagnosed on cytology. The two criteria of utmost importance used in their diagnosis are presence of nuclear atypia and absence of stromal invasion. The role of FNAC is limited because of its inability to establish the absence of stromal invasion and also because tissue patterns are not preserved in aspirate smears.
Tab. 5. Tabulation of results from existing literature
| Author | Year | No. of FNAs | No. of histology | Sensitivity (%) | Specificity (%) |
|---|---|---|---|---|---|
| Moran [20] | 1992 | 118 | 118 | 26 | 100 |
| Dordoni [21] | 1993 | 204 | 53 | 40 | 100 |
| Ganje [19] | 1995 | 81 | 74 | 75 | 100 |
| Mulvany [10] | 1995 | 32 | 23 | 69 | 100 |
| Pinto [5] | 1997 | 31 | 31 | 20-66 | 62-100 |
| Hemlatha [23] | 2005 | 105 | 105 | 85.7 | 94 |
| Uguz [24] | 2005 | 62 | 62 | 95.1 | 90 |
| Sood [25] | 2005 | 51 | 51 | 80 | 100 |
| This study | 2009 | 45 | 45 | 66.7 | 100 |
Various authors have reported a low cellularity or total absence of epithelial cells as a common reason for false-negative results [6, 8, 19-25].
In the present study, no incidence of cyst rupture or any other complication occurred during the procedure. The patients were followed for two years and no case of seeding of tumor or dissemination of malignancy was seen. A few case reports and studies are available in the literature where there have been diagnostic problems with cytological assessment compounded by spread of the cancer subsequent to the procedure [9, 22]. While others recommend that USG guided FNAC is relatively safe, simple and cost effective procedure in diagnosing ovarian neoplasms [7, 26]. The principal causes of diagnostic error were inadequate aspirate, improper sampling and lack of experience in interpreting the smears. Cell block preparation can help in overcoming this and also helps in subtyping ovarian neoplasms in certain situations [27].
Conclusion
FNAC is a safe and economic procedure with acceptable diagnostic accuracy especially in the experienced hands. Acellular fluid should not be considered non-diagnostic because it represents benign cysts in majority of cases. False negative results of FNAC in ovarian cystic lesions are usually due to the low cellularity of the sample and secondary degenerative changes. This can be avoided to certain extend by preparing cell blocks and hence we suggest the same. The distinction between cyst adenocarcinoma and borderline tumors cannot be confidently made by cytology alone. USG guided FNAC of ovarian cyst is an easy, fairly sensitive and specific technique and should be done as a routine. Therefore all clinical and sonographic findings should be considered in collaboration with FNAC findings in arriving at a diagnosis.
References
- Weiss NS, Peterson AS. Racial variation in the incidence of ovarian cancer in United States. Am J Epidemiol. 1978;107:91-95.
- Berrino F, Capocaccia R, Esteve J, Gatta G, Hakulinen T, et al. Survival of cancer patients in Europe: The EUROCARE 2 study. IARC scientific publication No 151. International Agency for Research on Cancer: Lyon. 1999.
- Parazzini F, Fransuschi S. Epidemiology of ovarian cancer review: Gyn Oncol. 1991;43:9-23.
- Marsden DE, Friedlander M, Hacker NF. Current management of epithelial ovarian carcinoma: A review. Semin Surg Oncol. 2000;19:11-19.
- Pinto MM, Greenebaum E, Simsir A. CA-125 and carcinoembryonic antigen assay vs. cytodiagnostic experience in the classification of benign ovarian cysts. Acta Cytol. 1997;41: 1456-1462.
- Martinez-Onsurbe P, Villaspesa AR, Anquela JMS, Ruiz PLV. Aspiration cytology of 147 adnexal cysts with histologic correlation. Acta Cytol .2001; 45:941-947.
- Ray S, Gangopadhyay M, Bandyopadhyay A, Majumdar K, Chaudhury N. USG guided FNAC of ovarian mass lesions: A cyto-histopathological correlation, with emphasis on its role in pre-operative management guidelines. J Turk Ger Gynecol Assoc. 2014; ;15:6-12.
- Athanassiadou P, Grapsa D. Fine needle aspiration of borderline ovarian lesions. Is it useful? Acta Cytol. 2005; 49:278-285.
- Trimbos JB, Hacker NF. The case against aspirating ovarian cysts. Cancer. 1993;72: 828-831.
- Mulvany N, Ostor A, Ten G. Evaluation of estradiol in aspirated ovarian cystic lesions. Acta Cytol. 1995;39:663-668.
- Daunter B. Tumour markers in gynaecologic oncology. Gynecol Oncol. 1990;39:1-15.
- Wojcik EM, Selvaggi SM. Fine Needle Aspiration Cytology of Cystic Ovarian Lesions. Diagn Cytopathol. 1994;11: 9-14.
- Higgins RV, Matkins JF, Marroum MC. Comparison of fine needle aspiration cytologic findings of ovarian cysts with ovarian histologic findings. Am J Obstet Gynecol. 1999;180:550-553.
- Kjellgren O, Angstrom T, Bergman F, Willkund D. Fine needle aspiratin biopsy in diagnosis and classification of ovarian carcinoma. Cancer. 1971; 28: 967-976.
- Dietrich M, Osmers RGW, Grobe G. Limitations of the evaluation of adnexal masses by its macroscopic aspects, cytology and biopsy. Eur J Obstet Gynecol Reprod Biol. 1999;82: 57-62.
- Anderson WA, Nichols GE, Avery SR, Taylor PT. Cytologic diagnosis of ovarian tumors: factors influencing accuracy in previously undiagnosed cases. Am J Obstet Gynecol. 1995;173:457-464.
- Mulvany N, Pickel H, Schneeweiss D, Purstner P. Diagnostic value of gonadal steroid hormones and gonadotropin in ovarian cystic lesions. Diagn Cytopathol. 1995;12:323-326.
- Kreuzer GF, Paradowski T, Wurche KD, Flenher H. Neoplastic or non- neoplastic cysts? The role of cytology. Acta Cytol. 1995; 39: 882-886.
- Ganjei P, Dickinson B, Harrison TA. Aspiration cytology of neoplastic and non neoplastic ovarian cysts : is it accurate ? Int J Gynaecol Pathol. 1996;15:94-101.
- Moran O, Menczer J, Ben- Barauch G. cytologic examination of ovarian cyst fluid for the distinction between benign and malignant tumors. Obstet Gynaecol. 1993;82:444-446.
- Dordoni D, Zaglio S, Zucca S, Favalli G. The role of sonographically guided aspiration in the clinical management of ovarian cysts. J Ultrasound Med. 1993;12:27-31.
- Nicklin JL, VanEijkeren M, Athanasatos P, Wain GV, Hacker NF. A comparison of ovarian cyst aspirate cytology and histology: the case against aspiration of cystic pelvic masses. Aust NZ J Obstet Gynaecol. 1994;34:546-549.
- Hemlatha AL, Divya P, Mamatha R. Image directed percutaneous FNAC of ovarian neoplasms. Indian J Pathol Microbiol. 2005;48:305-309.
- Uguz A, Ersoz C, Bolat F, Gokdemir A, Vardar MA. Fine needle aspiration cytology of ovarian lesions. Acta Cytol. 2005;49:144-148.
- Sood T, Handa U,Mohan H and P. Goel. Evaluation of aspiration cytology of ovarian masses with histopathological correlation. Cytopathol. 2009;21:176-185
- Pooja K. FNAC: Is it useful in diagnosis and classification of ovarian lesions? Nat J Lab Med. 2015;4:13-18.
- Mathew EP, Nair V. Role of cell block in cytopathologic evaluation of image-guided fine needle aspiration cytology. J Cytol. 2017;34:133-138.



