Research Article - Onkologia i Radioterapia ( 2026) Volume 20, Issue 2
Retrospective Analysis of CBCT-Based Repositioning During Prostate Radiotherapy
Anas Ardouz1,2*, Abdelouahab Abarane1, Youness Khobbaizi3, Mustapha Bougteb1, Mounir Mkimel1 and Redouane El Baydaoui12Tetouan Private Hospital - AKDITAL, Morocco
3Littoral Clinic Safi, Morocco
Anas Ardouz, Sciences and Engineering of Biomedicals, Biophysics and Health Laboratory, Hassan First University, Higher Institute of Health Sciences, 26000, Settat, Morocco, Email: anass.ardouz@gmail.com
Received: 01-Feb-2026, Manuscript No. OAR-26-187444; , Pre QC No. OAR-26-187444 (PQ); Editor assigned: 04-Feb-2026, Pre QC No. OAR-26-187444 (PQ); Reviewed: 20-Feb-2026, QC No. OAR-26-187444; Revised: 25-Feb-2026, Manuscript No. OAR-26-187444 (R); Published: 28-Feb-2026
Abstract
Objective: To retrospectively evaluate the effectiveness of cone-beam computed tomography (CBCT)-based repositioning during prostate radiotherapy and to assess its impact on treatment accuracy and safety margins.
Methods: This retrospective study included a cohort of patients with prostate cancer treated with external beam radiotherapy at Casablanca General Hospital. For each treatment session, a CBCT scan was acquired to quantify interfractional setup deviations along the left-right (LR), anterior-posterior (AP), and superior-inferior (SI) axes. Statistical analyses were performed to determine the mean displacements and the probability of exceeding conventional safety margins.
Results: Overall, several hundred CBCT scans were analyzed. The mean displacements were 0.31 cm along the LR axis, 0.21 cm along the SI axis, and less than 0.5 cm along the AP axis. The probability of a displacement greater than 3 mm was 41% for the LR axis, compared with 8% for the SI axis and a negligible value for the AP axis. The LR axis was identified as the most critical direction, with displacement amplitudes reaching up to 1.6 cm. The use of CBCT reduced residual setup errors to less than 3 mm in the majority of cases, thereby improving prostate target coverage and enhancing the protection of organs at risk.
Conclusion: CBCT is a reliable and effective tool for daily patient repositioning in prostate cancer radiotherapy. Our findings show that the lateral (LR) axis is the most prone to clinically significant displacements, supporting the need for appropriately adapted treatment margins. The systematic integration of CBCT into daily practice improves treatment precision and may reduce the risk of rectal and bladder toxicity, in agreement with findings reported in the international literature.
Keywords
CBCT, VMAT, Prostate Cancer, IGRT, Adaptive Radiotherapy
INTRODUCTION
Prostate cancer is among the most frequently diagnosed cancers in men and remains a major public health issue. External beam radiotherapy is one of the standard treatment options, enabling dose escalation and improved tumor control. Nevertheless, treatment accuracy is challenged by setup uncertainties and by both interactional and intrafraction prostate motion, largely related to variations in bladder and rectal filling [6].
To account for these uncertainties, safety margins are traditionally added around the clinical target volume (CTV) to generate the planning target volume (PTV). Van Herk et al. proposed widely used margin calculation formalism, showing that margins should ensure that 90% of patients receive at least 95% of the prescribed dose [1]. However, larger margins inevitably increase the irradiation of surrounding organs at risk, especially the rectum and bladder, thereby raising the likelihood of treatment-related toxicity. The development of image-guided radiotherapy (IGRT), particularly cone-beam computed tomography (CBCT), has made it possible to directly visualize the prostate and apply daily positional corrections [2,6]. Numerous studies have demonstrated that CBCT can substantially reduce the margins required in prostate radiotherapy by decreasing setup uncertainties. Létourneau et al. reported that residual errors following CBCT-guided correction were generally below 2 mm, while Ariyaratne et al. showed that daily imaging improved target coverage and reduced rectal dose [3, 5, 6]. Against this background, our study retrospectively investigates interactional displacements measured by CBCT in patients undergoing prostate cancer radiotherapy at Casablanca General Hospital. The aim was to assess the effectiveness of CBCT-guided repositioning and to determine appropriate safety margins for local clinical practice, while comparing our results with those reported in the international literature.
Materials and Methods
Study Population
This retrospective study was conducted at Casablanca General Hospital. It included 22 patients diagnosed with prostate adenocarcinoma and treated with external beam radiotherapy. A total of 747 CBCT acquisitions obtained during treatment sessions were analyzed, allowing the assessment of interactional displacements and the estimation of appropriate safety margins [Table 1].
| Parameter | Value |
|---|---|
| Number of patients | 22 |
| Mean age | 58 years |
| Total number of CBCT scans | 747 |
| Prescribed dose | 78 Gy |
| Fractionation | 39 × 2 Gy |
| Technique | VMAT |
Table 1: General characteristics of the study population
Simulation and Treatment Planning
Patients were positioned supine and immobilized using a customized fixation device consisting of knee and foot supports to ensure setup reproducibility. Skin reference marks were drawn at the intersection of the sagittal, coronal, and transverse laser beams and protected with waterproof dressings.
A planning CT scan with millimetric slice thickness was then acquired. Target volumes were delineated in accordance with RTOG/ICRU recommendations:
- CTV: prostate with or without seminal vesicles, depending on tumor stage;
- PTV: obtained by adding an initial isotropic margin to the CTV.
Treatment planning was performed using a dedicated treatment planning system and was jointly validated by the radiation oncologist and the medical physicist. Radiotherapy was delivered using an Elekta Versa HD linear accelerator to a total dose of 78 Gy in 39 fractions of 2 Gy.
CBCT Acquisition and Repositioning
CBCT images (kV-XVI, Elekta) were acquired before each treatment session. They were registered to the simulation CT using automatic and manual matching procedures to quantify interfractional displacements along the three spatial axes:
- Left–Right (LR),
- Anterior–Posterior (AP),
- Superior–Inferior (SI).
Positional corrections were then applied through translational adjustments of the treatment couch [Figure 1].
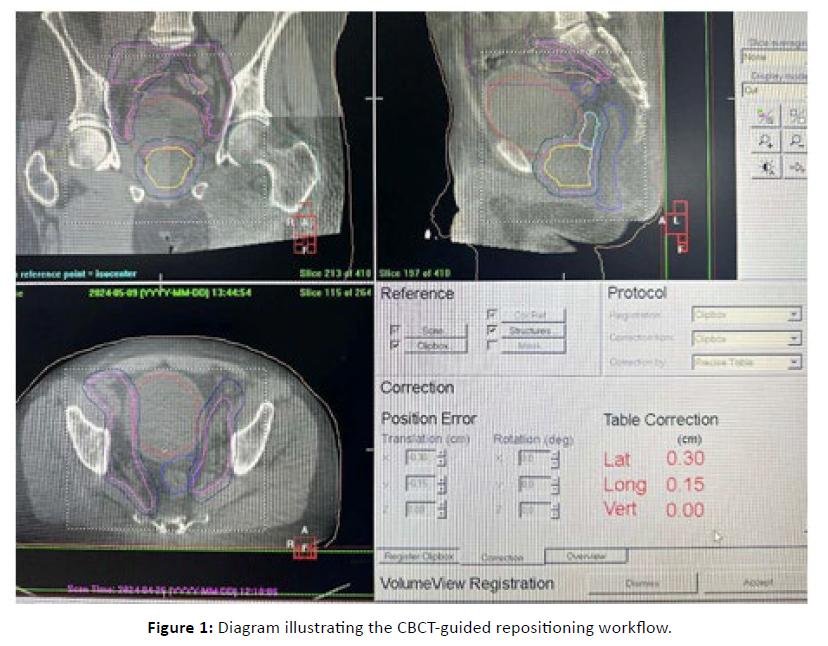
Figure 1: Diagram illustrating the CBCT-guided repositioning workflow.
Statistical Analysis
Setup displacements were recorded for each patient at every treatment session. The statistical analysis included:
- The mean and standard deviation of the measured displacements,
- The maximum observed displacement values,
- The probability of exceeding 3 mm and 5 mm thresholds along each axis.
Required treatment margins were estimated using the van Herk formalism [1]:
Margin=2,5Σ+0,7σ
Where Σ represents the systematic error (inter-patient) and σ the random error (intra-patient)..
Results
Validation of the Normal Distribution
The histograms of the measured displacements along the three axes (LR, AP, and SI) showed good agreement with the corresponding Gaussian curves, thereby confirming the assumption of a normal distribution of the data [Figure 2-4].
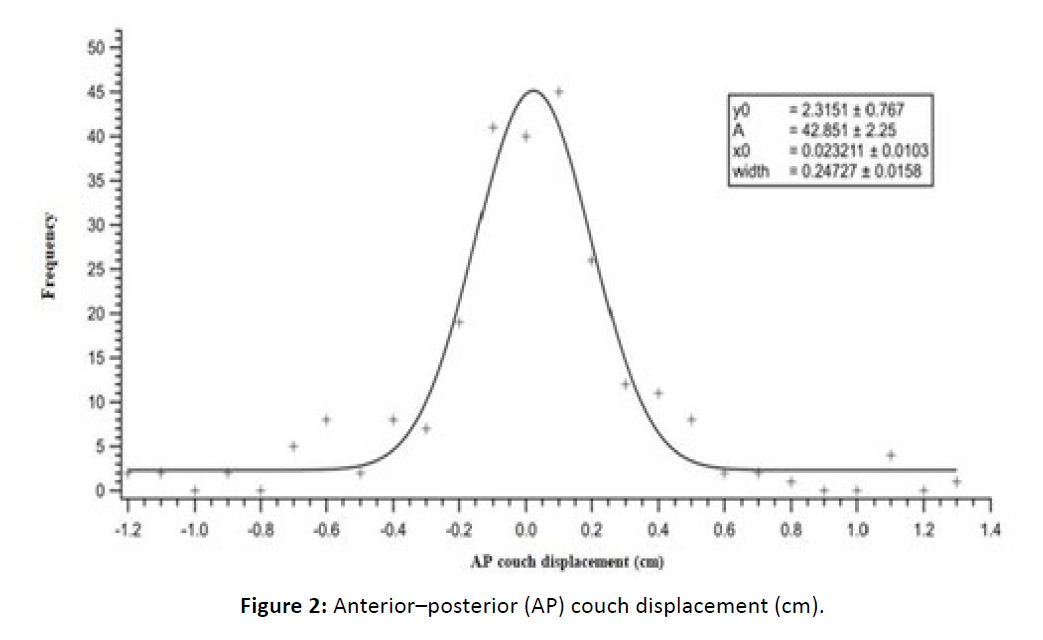
Figure 2: Anteriorâposterior (AP) couch displacement (cm).
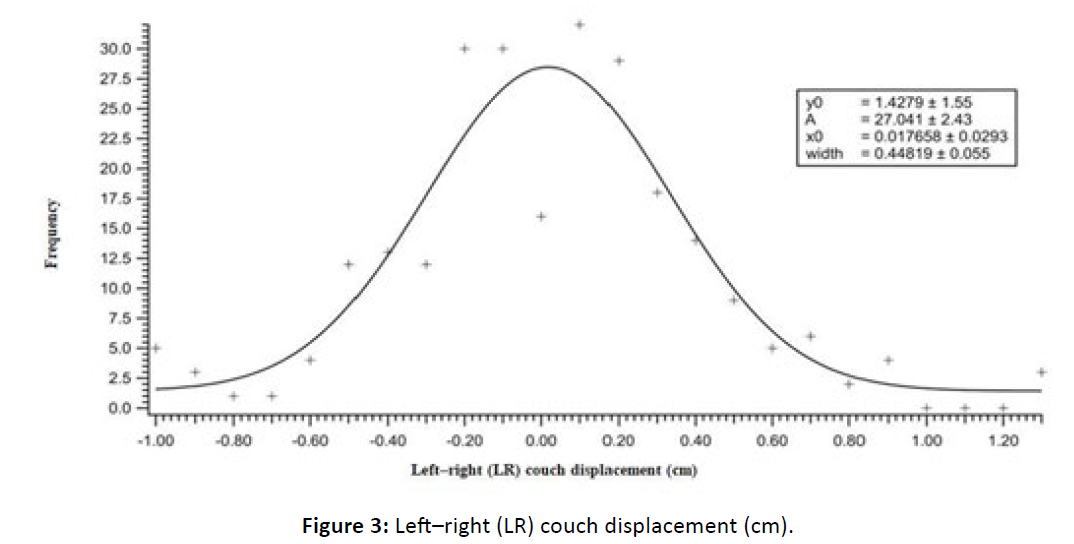
Figure 3: Leftâright (LR) couch displacement (cm).
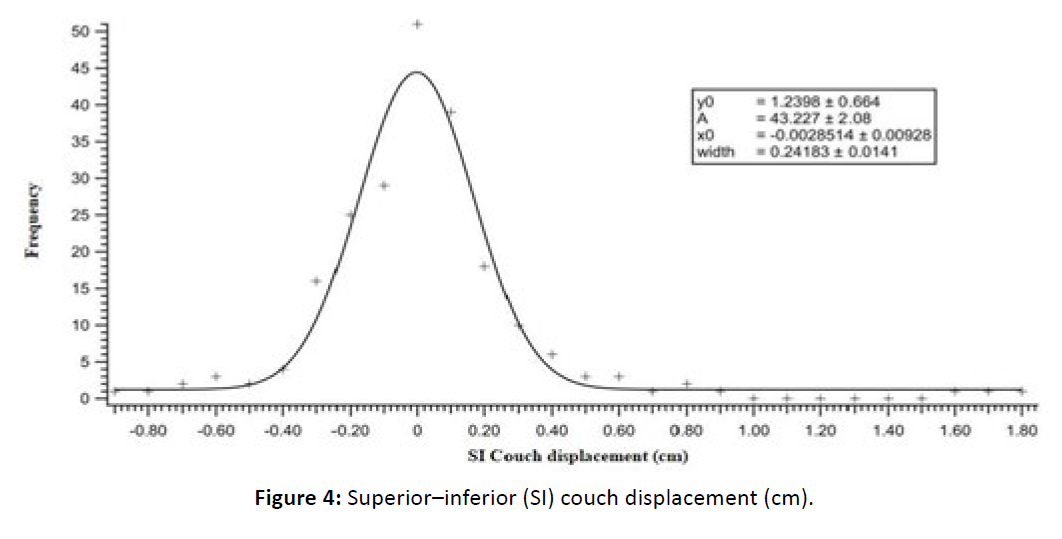
Figure 4: Superior–inferior (SI) couch displacement (cm).
Interfractional Displacements
The mean displacements were 0.31 cm along the left–right (LR) axis, less than 0.5 cm along the anterior–posterior (AP) axis, and 0.21 cm along the superior–inferior (SI) axis. The maximum observed displacement reached 1.6 cm along the LR axis [Table 2].
| Axis | Mean (cm) | Minimum (cm) | Maximum (cm) |
|---|---|---|---|
| LR | 0.31 | –0.81 | 1.6 |
| AP | <0.5 | –0.76 | 0.93 |
| SI | 0.21 | –0.84 | 0.8 |
Table 2: Mean and maximum interfractional setup displacements
Histograms of interfractional couch displacements along the LR, AP, and SI axes, together with their corresponding Gaussian fits, are shown below [Figure 5].
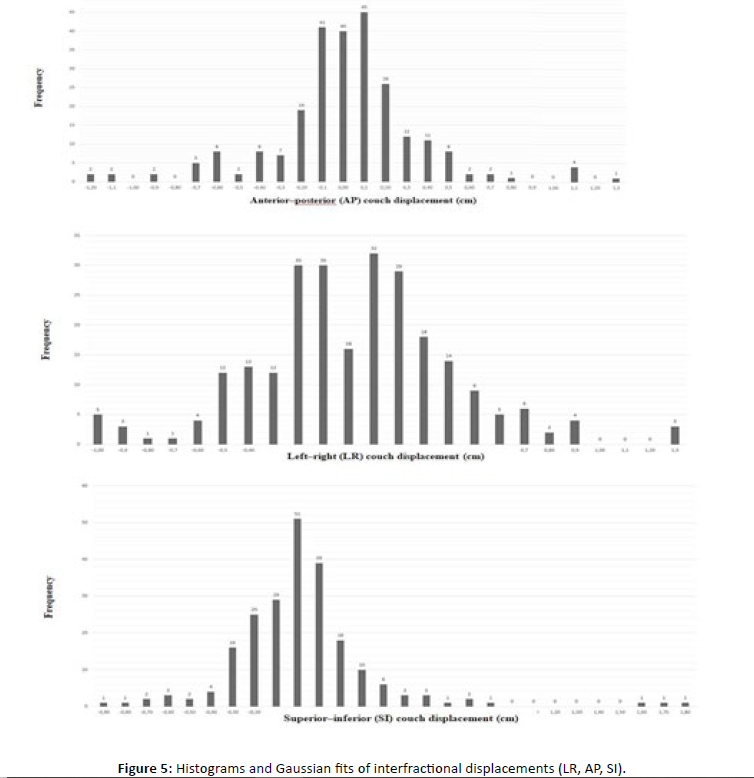
Figure 5: Histograms and Gaussian fits of interfractional displacements (LR, AP, SI).
Probabilities of Threshold Exceedance
Probabilistic analysis demonstrated that the left–right (LR) axis was the most unstable, with 41% of measurements exceeding ±3 mm. For the superior–inferior (SI) axis, 8% of measurements exceeded ±3 mm, whereas the anterior–posterior (AP) axis remained relatively stable, with a negligible probability of displacements greater than ±5 mm [Table 3].
| Axis | P(|Δ| > 3 mm) | P(|Δ| > 5 mm) |
|---|---|---|
| LR | 41% | 12% |
| AP | 5% | 1% |
| SI | 8% | 2% |
Table 3: Probability of displacement exceeding predefined thresholds
Overall Analysis
Analysis of the full dataset of 747 displacements confirmed that the left–right (LR) axis was the most variable direction [Table 4].
| Axis | Mean (cm) | Standard deviation (cm) | Maximum displacement (cm) |
|---|---|---|---|
| LR | 0.31 | 0.43 | 1.6 |
| AP | <0.5 | 0.38 | 0.93 |
| SI | 0.21 | 0.35 | 0.8 |
Table 4: Summary of overall interfractional displacements
PTV Margin Calculation
Systematic (Σ) and random (σ) errors were calculated using the van Herk formalism. The resulting optimal margins were 6.71 mm in the AP direction, 6.62 mm in the LR direction, and 6.35 mm in the SI direction, yielding an average margin of approximately 6.5 mm [Table 5].
| Axis | Σ (mm) | σ (mm) | PTV margin (mm) |
|---|---|---|---|
| LR | 3,59 | 0,0037 | 6,71 |
| AP | 3,50 | 0,0026 | 6,62 |
| SI | 3,22 | 0,0039 | 6,35 |
Table 5: Systematic (Σ) and random (σ) errors and corresponding calculated PTV margins
DISCUSSION
Our findings highlight the importance of CBCT in reducing interfractional uncertainties in prostate radiotherapy. The left–right (LR) axis was identified as the most variable direction, with displacements reaching up to 1.6 cm, whereas the anterior–posterior (AP) axis remained the most stable. This directional variability may be explained by differences in patient setup reproducibility and anatomical constraints, particularly the influence of rectal filling and lateral positioning.
These results are consistent with previous studies. Létourneau et al. reported residual errors below 2 mm following CBCT-guided correction [2], while Ariyaratne et al. demonstrated that daily imaging improves target coverage and reduces rectal dose [3]. In comparison with the margins currently used at Casablanca General Hospital (10 mm in the LR and SI directions and 5 mm in the AP direction), our data suggest that margins could be reduced to approximately 6–7 mm in the LR and SI directions, while a slight increase may be warranted in the AP direction. These findings support the validity of the van Herk formalism [1] and are consistent with ESTRO-ACROP recommendations for prostate IGRT [5].
The routine use of CBCT is particularly relevant in the context of modern radiotherapy techniques. The HYPO-RT trials have demonstrated the non-inferiority of hypofractionated regimens and stereotactic body radiotherapy (SBRT) compared with conventional fractionation, with comparable toxicity profiles [7-9]. However, these approaches rely on daily image guidance and reduced treatment margins (3–5 mm), highlighting the clinical relevance of our results.
Furthermore, soft tissue–based alignment strategies described by Kupelian et al. [4], together with the MIRAGE trial results demonstrating reduced gastrointestinal and genitourinary toxicity with MRI-guided SBRT [10], reflect the ongoing shift toward adaptive and MRI-guided radiotherapy.
Although CBCT-related imaging dose is generally low and clinically justified, it should be carefully monitored and optimized using low-dose acquisition protocols [6].
This study has several limitations. It is a single-center retrospective analysis with a relatively small cohort (22 patients) and is restricted to translational corrections (three degrees of freedom), without CBCT-based dosimetric recalculation or precise assessment of imaging dose.
Future multicenter studies incorporating six-degree-of-freedom (6D) corrections, low-dose imaging protocols, and MR-Linac technology are warranted to validate these findings, refine margin definitions, and further support the implementation of hypo fractionation and SBRT in prostate cancer management.
Conclusion
This retrospective study, including 22 patients and 747 CBCT acquisitions, demonstrates that daily CBCT improves the accuracy of prostate radiotherapy. The estimated optimal margins (~6.5 mm) support the use of anisotropic, axis-specific margin adaptation, reducing dose to organs at risk while maintaining adequate target coverage. These findings reinforce the clinical value of routine CBCT integration and support the implementation of advanced treatment strategies, including hypo fractionation, stereotactic body radiotherapy (SBRT), and adaptive radiotherapy.
References
- Van Herk M, Remeijer P, Rasch C, Lebesque JV. The probability of correct target dosage: Dose-population histograms for deriving treatment margins in radiotherapy. Int J Radiat Oncol Biol Phys. 2000; 47: 1121-1135.
[Crossref], [Google Scholar], [PubMed]
- Létourneau D, Martinez AA, Lockman D, Yan D. Assessment of residual error for online cone-beam CT-guided treatment of prostate cancer patients. Int J Radiat Oncol Biol Phys. 2005; 62: 1239-1246.
[Crossref], [Google Scholar], [PubMed]
- Ariyaratne H, Chesham H, Pettinger T, Alonzi R. Image-guided radiotherapy for prostate cancer with cone-beam CT: dosimetric effects of imaging frequency and PTV margin. Radiother Oncol. 2016; 121: 103-108.
[Crossref], [Google Scholar], [PubMed]
- Kupelian PA, Lee C, Langen KM, Zeidan OA, Mañon RR, et al. Evaluation of image-guidance strategies in the treatment of localized prostate cancer. Int J Radiat Oncol Biol Phys. 2008; 70: 1151-1157.
[Crossref], [Google Scholar], [PubMed]
- Ghadjar P, Fiorino C, Munck af Rosenschöld P, Pinkawa M, Zilli T, et al. ESTRO-ACROP consensus guideline on the use of image-guided radiation therapy for localized prostate cancer. Radiother Oncol. 2019; 141: 5-13.
[Crossref], [Google Scholar], [PubMed]
- Dang A, Kupelian PA, Cao M, Agazaryan N, Kishan AU. Image-guided radiotherapy for prostate cancer. Transl Androl Urol. 2018; 7: 308-320.
[Crossref], [Google Scholar], [PubMed]
- Widmark A, Gunnlaugsson A, Beckman L. HYPO-RT-PC: ultra-hypofractionated vs conventional RT-5-year outcomes. 2019; 394: 385-395.
[Crossref], [Google Scholar], [PubMed]
- Fransson P, Nilsson P, Gunnlaugsson A. HYPO-RT-PC: patient-reported QoL outcomes. Lancet Oncol. 2021; 22: 235-245.
[Crossref], [Google Scholar], [PubMed]
- Tree AC, Ostler P, Van der Voet H. PACE Trial Investigators. PACE-B: 2-year toxicity, IMRT vs SBRT. Lancet Oncol. 2022; 23: 1308-1320.
[Crossref], [Google Scholar], [PubMed]
- Kishan AU, Ma TM, Lamb JM. MIRAGE: MRI-guided vs CT-guided SBRT for prostate cancer. JAMA Oncol. 2023;9: 365-373.
[Crossref], [Google Scholar], [PubMed]
- Janssen TM, Remeijer P, Van der Heide UA, Sonke JJ, Van der Bijl E. A margin recipe for intra-fraction target motion in radiotherapy. Radiother Oncol. 2022;177: 139-147.
[Crossref], [Google Scholar], [PubMed]



