Research Article - Onkologia i Radioterapia ( 2026) Volume 20, Issue 2
Improving Radiotherapy Department Performance Through Lean Management : A BeforeâAfter Study
Samia KHALFI1,2,3,4*, Rodouan TOUTI4, Abdelkarim UAKKAS2, Khadija AMSSAYEF2, El Mehdi SADIKI2,4, Youssef AGHLALLOU3, Fatima, Zahra FARHANE1,2,3, Zenab ALAMI1,2,3, Mouhcine ASSALE5 and Touria BOUHAFA1,2,32Radiotherapy Department, Hassan II University Hospital, Fez, Morocco
3Cancer Research Institute (IRC), Morocco
4Advanced Materials and Applications Laboratory, Faculty of Sciences Dhar El Mahraz, Sidi Mohammed Ben Abdellah University, Fez, Morocco
5Mohammed VI International Academy of Civil Aviation, University of Casablanca, Technopole of Mohammed V Airport, Nouaceur, Casablanca 20100, Morocco
Samia KHALFI, Faculty of Medicine and Pharmacy of Fez, Morocco, Email: Samia.khalfi@gmail.com
Received: 01-Feb-2026, Manuscript No. OAR-26-186266; , Pre QC No. OAR-26-186266 (PQ); Editor assigned: 05-Feb-2026, Pre QC No. OAR-26-186266 (PQ); Reviewed: 21-Feb-2026, QC No. OAR-26-186266; Revised: 26-Feb-2026, Manuscript No. OAR-26-186266 (R); Published: 28-Feb-2026
Abstract
Objectives: Lean Management, originally developed in the Japanese automotive industry, is increasingly being applied in healthcare systems. This study aimed to describe the implementation process of Lean Management in a radiotherapy department within an African healthcare setting, to identify and eliminate waste through Value Stream Mapping (VSM), and to quantify the resulting improvements in treatment initiation delays, documentation compliance, and patient satisfaction.
Methods: A one-year before–after observational study was conducted from May 2024 to April 2025 in the radiotherapy department of Hassan II University Hospital in Fez, Morocco, including 945 patients (450 in the pre-Lean period and 495 in the post-Lean period). Value Stream Mapping was used to identify valueadded activities, necessary but non-value-added activities, and pure waste within the care pathway. Four Lean interventions were implemented: digitalization of communication between the four medical teams, improvement of patient reception procedures, optimization of appointment scheduling using a Kanban approach, and the collaborative development of standardized procedures covering the complete care pathway for the main tumor sites. Outcome indicators included the simulation-to-treatment initiation delay, the documentation non-compliance rate, and patient satisfaction scores.
Results: Among the 12 steps identified in the VSM, 7 were classified as value-added activities, 3 as necessary but non-value-added activities, and 2 as pure eliminable waste. The mean simulation-to-treatment initiation delay decreased from 28.4 ± 8.1 days to 16.0 ± 10.2 days, representing a 43.7% reduction (p = 0.043). Root cause analysis identified avoidable re-simulations as the main residual source of waste, associated with an additional delay of 14.2 days per case (30.0 vs 15.8 days). The documentation non-compliance rate decreased from 67.3% to 10.7% (84.1% reduction, p < 0.001), while complete clinical file traceability improved from 32.7% to 100%. Patient satisfaction increased by 25.8% (6.2 to 7.8/10, p < 0.001).
Conclusion: Lean Management, implemented through rigorous Value Stream Mapping and targeted interventions addressing root causes of inefficiencies, significantly improved the organizational performance of a radiotherapy department, even in a resource-constrained African healthcare setting. The identification of avoidable re-simulations as the main residual source of waste and the development of standardized procedures according to tumor site represent key contributions of this initiative. This experience provides a reproducible model for other African hospitals seeking to optimize radiotherapy care pathways.
Keywords
Lean Management; Value Stream Mapping; Radiotherapy; Hospital Waste; Quality of Care; Morocco
INTRODUCTION
Radiotherapy plays a central role in the multidisciplinary management of cancer, as it is involved in the care of nearly 60% of oncology patients during their treatment pathway. Recent technological advances, such as intensity-modulated radiotherapy (IMRT) and onboard imaging, have significantly improved treatment precision and efficacy. However, these innovations are accompanied by increasing procedural complexity and higher organizational demands. In many countries, particularly in Africa, radiotherapy departments face multiple constraints: limited human and material resources, a constantly increasing patient load, prolonged waiting times, and the need to maintain high standards of quality and safety. In this context, optimizing organizational processes becomes a strategic priority to ensure efficient and equitable patient care [1]. Lean Management, originally developed in the Japanese automotive industry (notably through the Toyota Production System), has gradually been adapted to healthcare settings. Its core principles are based on waste elimination, continuous improvement, and active team involvement in problem-solving [2]. Several studies conducted in European and North American hospitals have demonstrated that Lean approaches can reduce delays, optimize patient flow, and improve satisfaction for both patients and healthcare providers [3-5]. However, there is limited evidence on the application of Lean Management in radiotherapy departments in Morocco and, more broadly, across Africa. In this context, we initiated a Lean approach in the radiotherapy department of Hassan II University Hospital in Fez, with the primary objective of enhancing organizational performance and the quality of patient care. This article presents the results of this initiative, detailing the implemented interventions, monitored indicators, and measured impact on departmental performance.
METHODOLOGY
Study Design
This was a before–after observational study conducted in the radiotherapy department of Hassan II University Hospital in Fez over a one-year period, from May 2024 to April 2025. The primary objective was to assess the impact of implementing Lean Management on the organization and performance of the department.
Lean Implementation Steps
The methodology followed classical Lean Healthcare principles, adapted to the radiotherapy context:
Process Mapping (Value Stream Mapping, VSM):
- Identification of the patient care pathway from the initial consultation to the start of treatment.
- Analysis of critical steps: initial consultation, simulation, treatment planning, medical validation, and treatment initiation.
- Identification of bottlenecks, redundancies, and waste, including waiting times, limited access to equipment, and fragmented communication.
Waste Identification and Prioritization:
- Prolonged waiting times.
- Limited accessibility to equipment, causing time loss for physicians and technicians.
- Insufficient communication between teams.
- Lack of standardization of procedures.
Implementation of Corrective Actions:
- Logistics reorganization: improvement of workspace, storage areas, and waiting rooms.
- Schedule optimization: partial digitalization of session calendars and enhanced interdisciplinary coordination.
- Procedure standardization: harmonized communication protocols and introduction of Lean-inspired tools (5S, Kanban).
- Training and awareness: active involvement of all staff (physicians, physicists, technicians, nurses) through participatory workshops.
Performance Indicators
To assess the impact of the Lean approach, several indicators were defined and compared before and after implementation:
- Mean time from initial consultation to treatment initiation (in days).
- Organizational non-compliance rate (planning errors, lost material, delays attributable to organizational inefficiencies).
- Patient satisfaction, assessed using an internal questionnaire covering pathway understanding, perceived waiting times, and patient–caregiver relationships.
Statistical Analysis
Data were entered and analyzed using R software.
- Quantitative variables were expressed as mean ± standard deviation and compared using the Student’s t-test.
- Qualitative variables were compared using the Chi-square test.
- A p-value < 0.05 was considered statistically significant.
RÉSULTS
Value Stream Mapping: process classification and waste identification
The Value Stream Mapping (VSM) analysis identified 10 sequential steps in the radiotherapy patient pathway, from the initial consultation to treatment initiation.
Among these steps, seven were classified as value-added activities, directly contributing to patient care, one was considered necessary but non–value-added, and two were identified as pure wastes that could potentially be eliminated [Table 1].
| Lean Waste Type | Manifestation in the Department | Measured Impact | Corrective Action Implemented |
|---|---|---|---|
| Defects (Errors) | Incomplete files, missing validation, traceability errors | 67.3% non-conformities before → 10.7% after | Shared digital traceability |
| Overproduction / Rework | Avoidable re-simulation at the CT simulator | +14.2 days delay per case | standard procedures by tumor site |
| Waiting | Overcrowded waiting room, simultaneous appointments | Waiting perception: 5.5/10 before | Kanban — schedule slot optimization |
| Information Transfer | Fragmented communication between staff | Traceability only 32.7% | Communication digitalization |
| Underutilized Skills | Patients poorly informed about the care pathway, non-standardized reception | Pathway understanding: 5.8/10 | Reception procedures + patient information |
Table 1: Taxonomy of wastes identified through the VSM and corrective actions implemented
The two main sources of waste identified were:
- Avoidable re-simulations at the CT simulator, mainly related to insufficient initial patient preparation, lack of standardized protocols, or the use of inappropriate immobilization devices.
- Administrative delays related to incomplete reimbursement or treatment authorization files, leading to postponements before treatment initiation.
These two types of waste accounted for the majority of avoidable delays within the care pathway, and were therefore defined as priority targets for Lean interventions. The VSM also revealed several systemic inefficiencies, including fragmented communication between staff members, limited traceability of documentation, and suboptimal use of consultation and waiting areas. These findings guided the implementation of targeted Lean interventions aimed at improving workflow efficiency and reducing process variability [Figure 1], [Table 1].
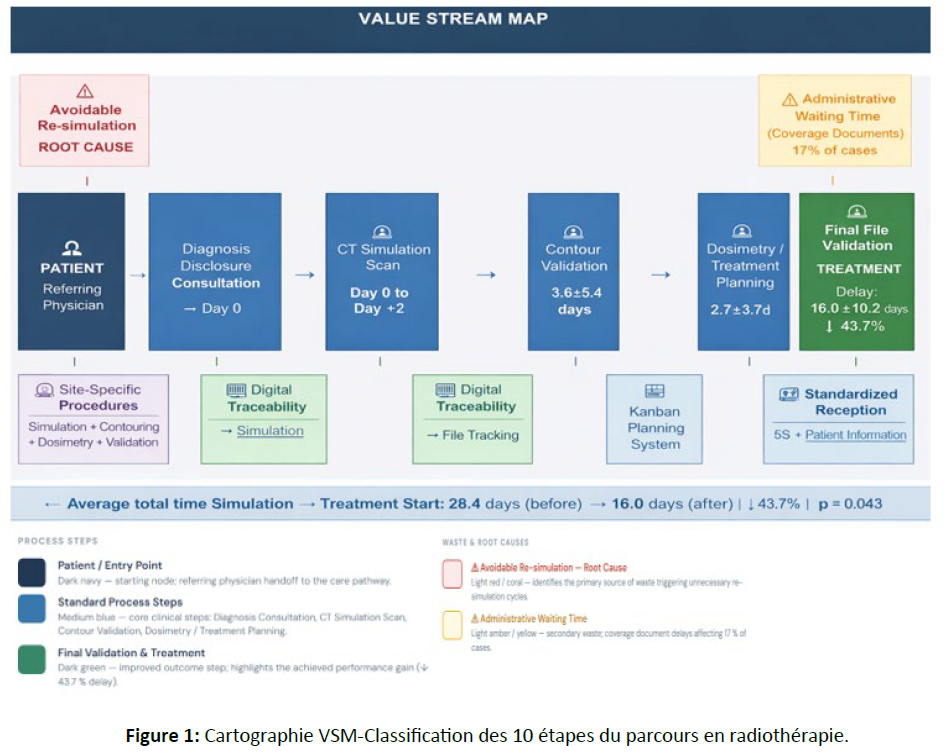
Figure 1: Cartographie VSM-Classification des 10 étapes du parcours en radiothérapie.
Quantitative outcomes after Lean implementation
Following the implementation of four targeted Lean interventions, significant improvements were observed across several organizational indicators [Table 2].
| Indicator | Before Lean | After Lean | Δ (%) | p-value |
|---|---|---|---|---|
| Simulation → treatment delay (days, mean ± SD) | 28.4 ± 8.1 | 16.0 ± 10.2 | ↓ 43.7% | 0.043 |
| • With avoidable re-simulation | — | 30.0 days (n=4) | +14.2 days | — |
| • Without re-simulation | — | 15.8 days (n=233) | Reference | — |
| Documentary non-compliance rate (%) | 67.30% | 10.70% | ↓ 84.1% | < 0.001 |
| Complete file traceability (%) | 32.70% | 100% | ↑ +67.3 pts | < 0.001 |
| Standardized procedures by tumor site | 0 | 8 (complete care pathways) | Innovation | — |
| Patient satisfaction (/10) | 6.2 ± 1.4 | 7.8 ± 1.2 | ↑ +25.8% | < 0.001 |
| Monthly volume (patients/month) | 75 | 82 | ↑ +9.3% | — |
Table 2: Quantitative results before and after the Lean approach
Reduction in treatment initiation delay
The mean delay between CT simulation and treatment initiation decreased significantly from 28.4 ± 8.1 days before Lean implementation to 16.0 ± 10.2 days afterward, representing a 43.7% reduction (p = 0.043). Stratified analysis according to the presence of re-simulation highlighted the impact of this specific source of waste. Patients requiring avoidable re-simulation experienced a mean delay of 30.0 days, compared with 15.8 days in patients without re-simulation, corresponding to an additional 14.2 days per affected case. This finding illustrates the substantial organizational cost associated with this type of waste.
Improvement in documentation quality and traceability
The rate of documentary non-compliance decreased markedly from 67.3% before Lean implementation to 10.7% afterward (χ² = 319.5, p < 0.001). Simultaneously, complete file traceability improved from 32.7% to 100%, reflecting the positive impact of digital traceability tools and standardized communication procedures.
Patient satisfaction
Patient satisfaction scores improved significantly, increasing from 6.2 ± 1.4 to 7.8 ± 1.2 out of 10, corresponding to a 25.8% increase (p < 0.001). This improvement was mainly related to better understanding of the care pathway, improved communication with healthcare professionals, and reduced perceived waiting times.
Organizational capacity
Finally, the monthly patient throughput increased from 75 to 82 patients per month, corresponding to a 9.3% increase in activity, without additional resources [Table 2].
Workspace Reorganization Based on 5S Principles
As part of the Lean approach, a reorganization of the department's workspaces was carried out based on the principles of the 5S methodology (Sort, Set in order, Shine, Standardize, Sustain). This reorganization covered several areas of the department, including equipment storage spaces, patient preparation areas, waiting rooms, as well as three specifically redesigned spaces: the dosimetry room, the physicians' training room, and a dedicated pediatric waiting room. The objective was to improve accessibility to equipment required at the various stages of the care pathway, reduce time losses associated with material searching, and enhance the overall patient experience. The dosimetry room underwent a major restructuring with the addition of new contouring and treatment planning workstations, bringing the simultaneous working capacity to 10 stations. This increase was made possible through an optimized spatial reorganization, enabling improved staff circulation and better accessibility to equipment. The training room was entirely redesigned to accommodate a larger number of participants under improved ergonomic conditions, with standardized storage of educational materials and training equipment.
The implementation of this visual organization resulted in:
- improved structuring of storage spaces,
- faster identification of required equipment,
- increased simultaneous contouring capacity,
- smoother circulation of staff and patients throughout the department [Figure 2].
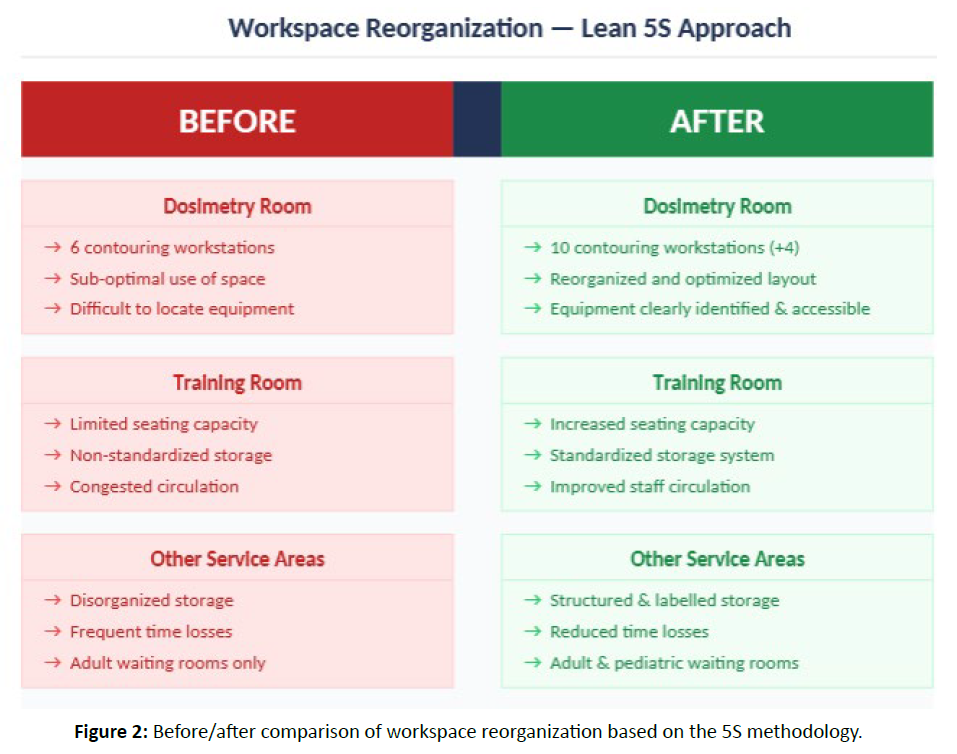
Figure 2: Before/after comparison of workspace reorganization based on the 5S methodology.
These organizational adjustments contributed to reducing certain inefficiencies identified during the VSM mapping and to improving patient satisfaction.
DISCUSSION
This study demonstrates that a structured Lean Management approach, guided by Value Stream Mapping (VSM), can generate significant and measurable improvements in the organization of a radiotherapy department operating under resource-constrained conditions. The results obtained at Hassan II University Hospital of Fez are consistent with those reported in the international Lean Healthcare literature, while also providing original contributions adapted to the context of African healthcare systems. Taken together, these findings highlight the potential of Lean methodologies to improve both operational efficiency and quality of care, even in healthcare environments characterized by limited infrastructural and financial resources.
VSM findings and process classification
To begin with, the VSM analysis identified 10 sequential steps in the care pathway, of which 7 were classified as value-added, 1 as necessary but non-value-added, and 2 as pure waste. These proportions are comparable to those reported by Al-Balushi and Al-Mandhari in a radiation oncology department in Oman, where 6 of 13 steps were considered value-adding [3].
More broadly, the systematic identification of waste sources through VSM is widely recognized as a fundamental prerequisite for any effective Lean intervention [6,7]. In the present study, avoidable re-simulations and administrative authorization delays emerged as the two main sources of pure waste within the care pathway. This observation is consistent with the findings of Kim et al., who similarly identified inefficiencies related to patient preparation as a major contributor to delays in radiotherapy workflows [4].
Beyond merely identifying process inefficiencies, value stream mapping also played a critical role in fostering a shared understanding of the patient care pathway among staff members. In turn, this collective visualization of the workflow contributed to strengthening team engagement in the improvement process. Such participatory approaches represent a core component of Lean philosophy, which emphasizes the active involvement of healthcare professionals in continuous quality improvement initiatives [2].
Reduction in treatment initiation delay
A second key finding of this study concerns the substantial reduction in treatment initiation delays. Specifically, the 43.7% reduction in the mean delay between simulation and treatment initiation (from 28.4 to 16.0 days) represents one of the most clinically meaningful outcomes of the Lean intervention.
From a clinical perspective, this reduction is particularly relevant. In radiation oncology, delays in treatment initiation have been associated with reduced local tumor control and decreased overall survival, especially in rapidly proliferating malignancies such as head and neck squamous cell carcinomas [8].
In this regard, the results observed in the present study are consistent with the broader literature. A systematic review conducted by Tlapa et al. demonstrated that Lean healthcare interventions consistently lead to reductions in patient flow times, with improvements ranging from 18% to 65% depending on the clinical context [5]. The magnitude of improvement observed in our department therefore falls well within the range reported in previous studies conducted in high-income healthcare systems.
Furthermore, the stratified analysis provided additional insights into the mechanisms underlying these delays. In particular, avoidable re-simulations resulted in an additional mean delay of 14.2 days per patient (30.0 days versus 15.8 days). This finding clearly confirms that this category of waste represents a high-priority target for intervention. The implementation of standardized preparation protocols according to tumor site, combined with the digitalization of inter-team communication, appears to have played a central role in mitigating this specific source of inefficiency.
Taken together, these results also underscore the importance of close multidisciplinary coordination between radiation oncologists, medical physicists, and radiation therapists, in order to anticipate technical constraints prior to simulation and thereby avoid unnecessary repetition of procedures.
Documentary compliance and traceability
Another important outcome of the Lean intervention relates to improvements in documentary compliance and clinical traceability. More specifically, the reduction in documentary non-compliance (from 67.3% to 10.7%, p < 0.001) and the achievement of 100% complete file traceability through digitalization represent major gains in terms of patient safety [9]. In the field of radiotherapy, incomplete or missing documentation constitutes a well-recognized safety risk, potentially leading to treatment errors, duplicated examinations, or unjustified delays in patient management [10]. The high baseline rate of non-compliance observed in our study therefore reflects a structural vulnerability that remains common in many African healthcare institutions, where information systems are often fragmented and predominantly paper-based [11]. Importantly, the digitalization of communication between clinical teams, combined with the implementation of standardized checklists according to tumor localization, proved particularly effective in improving both traceability and coordination of care. In addition, the development of comprehensive standardized care pathway procedures constitutes a sustainable institutional asset that may facilitate staff onboarding and contribute to the harmonization of clinical practices over time.
Patient satisfaction and organizational capacity
Beyond operational metrics, the Lean intervention was also associated with significant improvements in patient experience. Indeed, patient satisfaction increased from 6.2 to 7.8/10 (+25.8%, p < 0.001). This improvement appears to be primarily driven by better patient understanding of the care pathway, enhanced communication with healthcare professionals, and reduced perceived waiting times. Such findings are consistent with the patient-centered philosophy underlying Lean Healthcare, which seeks to simultaneously improve patient experience and organizational efficiency [12]. Moreover, the creation of a dedicated pediatric waiting area, together with the standardization of reception procedures, addressed the waste category identified as “underutilized skills.” By clarifying the role of reception staff in guiding patients through the care pathway, these interventions contributed to improving both patient orientation and overall care experience [13]. These measures are particularly relevant in the African context, where low levels of health literacy and sociocultural barriers may exacerbate the anxiety associated with cancer diagnosis and oncological treatments [14]. Importantly, the simultaneous increase in monthly patient throughput (+9.3%) without additional resources demonstrates that improvements in quality of care and organizational efficiency are not mutually exclusive. On the contrary, these results suggest that Lean interventions may create synergistic gains in both productivity and patient-centered outcomes.
Workspace reorganization and the 5S methodology
In addition to process-level interventions, the Lean initiative also included a reorganization of workspaces based on the 5S methodology, thereby addressing the physical environment as a potential source of operational inefficiency. Notably, the number of simultaneous contouring workstations increased from 6 to 10, achieved solely through spatial reorganization without structural modification of the facilities. This example illustrates how the 5S method can effectively unlock latent organizational capacity within existing infrastructures. More broadly, the 5S methodology is widely recognized as a foundational Lean tool that improves team efficiency, reduces errors, and optimizes the work environment [15]. In radiation oncology departments, where contouring and treatment planning frequently represent critical workflow bottlenecks, increasing workstation availability at these stages may have a direct and measurable impact on reducing treatment initiation delays.
Lean Healthcare in the African context
Finally, one of the most important contributions of this study lies in demonstrating that Lean Management can be successfully implemented in a radiotherapy department located in a low- and middle-income country. To date, the Lean Healthcare literature has been largely dominated by studies conducted in North American and European healthcare systems, while evidence from African contexts remains scarce [16]. Against this backdrop, the present findings challenge the assumption that Lean implementation necessarily requires substantial financial investment or highly sophisticated digital infrastructure. In fact, all interventions implemented in this study were carried out without additional financial or human resources, relying primarily on staff engagement, process redesign, and organizational innovation. In this respect, the approach adopted in this study aligns closely with the principles of frugal innovation in healthcare, which aim to develop effective, context-appropriate solutions in resource-constrained settings [17]. Consequently, the experience of Hassan II University Hospital of Fez may represent a replicable model for other radiotherapy departments across Africa facing similar operational challenges.
CONCLUSION
This study demonstrates that the implementation of a structured Lean Management program, grounded in Value Stream Mapping analysis and supported by targeted organizational interventions, can significantly improve the operational performance of a radiotherapy department operating under resource-constrained conditions.
Over a 12-month period, the Lean approach led to a 43.7% reduction in the mean simulation-to-treatment initiation delay, a substantial decrease in documentary non-compliance, and the achievement of complete clinical file traceability through digitalization. These improvements were accompanied by a significant increase in patient satisfaction and a 9.3% rise in monthly patient throughput, all achieved without additional financial or human resources.
Importantly, the identification of avoidable re-simulations as a major source of residual waste, associated with a mean additional delay of 14.2 days per patient, highlights a key operational target for future optimization. The implementation of standardized care pathway procedures according to tumor localization, together with improved multidisciplinary communication, played a central role in mitigating this inefficiency.
Beyond the immediate organizational benefits, this study provides evidence that Lean Healthcare principles can be successfully applied in radiotherapy departments within low- and middle-income countries. The experience of Hassan II University Hospital of Fez suggests that meaningful improvements in efficiency, patient safety, and care quality can be achieved through process optimization and team engagement rather than through costly technological investments.
Future research should focus on evaluating the long-term sustainability of these improvements, extending Lean interventions to additional stages of the oncology care pathway, and assessing their potential impact on clinical outcomes and health system performance in similar healthcare settings.
LIMITATIONS
Several limitations should be acknowledged in this study. First, the before–after observational design precludes causal inference; although improvements were observed after the Lean interventions, we cannot definitively attribute all changes solely to the implemented measures. Second, the study was conducted in a single center, which may limit the generalizability of the findings to other radiotherapy departments, especially in different resource settings or healthcare systems. Third, the long-term sustainability of the observed improvements remains unassessed; continuous monitoring will be required to ensure that gains in efficiency, compliance, and satisfaction are maintained over time. Finally, the small number of avoidable re-simulation cases limits the statistical power of analyses regarding this specific source of waste
ETHICS
All authors declare that the study was conducted in accordance with the ethical principles of the Declaration of Helsinki. The patients who participated in this study provided written informed consent.
CONFLICTS OF INTEREST
The authors declare no conflicts of interest related to this study.
FUNDING
This research is funded by cancer research institute of Morocco (IRC), www.irc.ma» (project n° 1317/ AmP 2023),
DATA AVAILABILITY STATEMENT
Data available upon request.
References
- Imazgal Y. L’application du Lean Management dans les hôpitaux marocains : Enjeux, défis et perspectives d’amélioration. African Scientific Journal. 2025. [Google Scholar]
- Alogla A. Revisiting lean healthcare: adopting value stream mapping from manufacturing. Front Health Serv. 2025;5:1613756. [Crossref], [Google Scholar], [PubMed]
- Al-Balushi MM, Al-Mandhari Z. Implementing Lean Management Techniques at a Radiation Oncology Department. Sultan Qaboos Univ Med J. 2018;18: e362-e366. [Crossref], [Google Scholar], [PubMed]
- Kim CS, Hayman JA, Billi JE, Lash K, Lawrence TS. The application of lean thinking to the care of patients with bone and brain metastasis with radiation therapy. J Oncol Pract. 2007;3: 189-193. [Crossref], [Google Scholar], [PubMed]
- Tlapa D, Zepeda-Lugo CA, Tortorella GL, Baez-Lopez YA, Limon-Romero J, et al. Effects of Lean Healthcare on Patient Flow: A Systematic Review. Value Health. 2020;23: 260-273. [Crossref], [Google Scholar], [PubMed]
- Womack JP, Jones DT. Lean Thinking: Banish Waste and Create Wealth in Your Corporation. 2nd ed. New York: Free Press; 2003. [Crossref], [Google Scholar]
- Toussaint JS, Berry LL. The promise of Lean in health care. Mayo Clin Proc. 2013;88: 74-82. [Crossref], [Google Scholar], [PubMed]
- Huang J, Robertson JM, Saxena A, Kanabus-Kaminska M, Das IJ. Time course of cause-specific mortality and local control in head-and-neck cancer treated by radiotherapy. Int J Radiat Oncol Biol Phys. 2003;56(3):798-809. doi:10.1016/s0360-3016(03)00084-4. [Google Scholar]
- Khalfi S, Malih T, Abiza ELM, Sadiki ELM, Chenfour N, et al. AI-driven radiotherapy appointment optimization: A lean management approach. Onkologia i Radioterapia. 2025; 19. [Google Scholar]
- Shafiq J, Barton M, Noble D, Lemer C, Donaldson LJ. An international review of patient safety measures in radiotherapy practice. Radiother Oncol. 2009;92: 15-21. [Crossref], [Google Scholar], [PubMed]
- Gouda HN, Charlson F, Sorsdahl K, Ahmadzada S, Ferrari AJ, et al. Burden of non-communicable diseases in sub-Saharan Africa, 1990-2017: results from the Global Burden of Disease Study 2017. Lancet Glob Health. 2019;7: e1375-e1387. [Crossref], [Google Scholar]
- Mazzocato P, Savage C, Brommels M, Aronsson H, Thor J. Lean thinking in healthcare: a realist review of the literature. Qual Saf Health Care. 2010;19: 376-382. [Crossref], [Google Scholar], [PubMed]
- KHALFI S, ABDELLI FZ, SADIKI El M. Revolutionizing pediatric radiotherapy reception: Implementing Kaizen for a child-friendly treatment journey. Onkologia i Radioterapia. 2025; 19. [Google Scholar]
- Cazap E, Magrath I, Kingham TP, Elzawawy A. Structural barriers to diagnosis and treatment of cancer in low- and middle-income countries: the urgent need for scaling up. J Clin Oncol. 2016;34: 14-19. doi:10.1200/JCO.2015.61.5761. [Crossref], [Google Scholar], [PubMed]
- Gapp R, Fisher R, Kobayashi K. Implementing 5S within a Japanese context: an integrated management system. Manag Decis. 2008;46: 565-579. doi:10.1108/00251740810865067. [Crossref], [Google Scholar]
- Burgess N, Radnor Z. Evaluating Lean in healthcare. Int J Health Care Qual Assur. 2013;26: 220-235. [Crossref], [Google Scholar], [PubMed]
- Bhatti Y, Taylor A, Harris M, Wadge H, Escobar E, Prime M, et al. Global lessons in frugal innovation to improve health care delivery in the United States. Health Aff (Millwood). 2017;36: 1912-1919. [Crossref], [Google Scholar]



