Research Article - Onkologia i Radioterapia ( 2026) Volume 20, Issue 1
From machine accuracy to clinical precision: A multilevel quality assurance approach for pelvic radiotherapy in cervical cancer
Ahlam Azalmad* and Mohamed HilalAhlam Azalmad, Laboratory of Sciences and Engineering of Biomedicals Biophysics and Health, Higher Institute of Health Sciences, University Hassan First, Settat, Morocco, Morocco,
Received: 03-Dec-2025, Manuscript No. OAR-26-184984; , Pre QC No. OAR-26-184984 (PQ); Editor assigned: 06-Dec-2026, Pre QC No. OAR-26-184984 (PQ); Reviewed: 16-Dec-2025, QC No. OAR-26-184984; Revised: 25-Jan-2026, Manuscript No. OAR-26-184984 (R); Published: 24-Feb-2026
Abstract
Background and purpose: Accurate and reproducible dose delivery in pelvic radiotherapy for cervical cancer requires both robust machine performance and rigorous patient-centered Quality Assurance (QA). While International Guidelines Define Linear Accelerator (LINAC) QA standards, limited data describe the integration of machine-level QA with workflow-based and end-to-end clinical validation in resource-constrained environments. This study aimed to implement and evaluate a comprehensive multilevel QA framework for pelvic radiotherapy in cervical cancer.
Materials and methods: A structured Quality Assurance (QA) program was implemented for an Elekta linear accelerator delivering 6 and 18 MV photon beams and 9–18 MeV electron beams to ensure compliance with clinical and international performance standards. The clinical relative dose distribution, isocenter, mechanical accuracy, and electrical safety for both the photon and electron beam were assessed using the AAPM TG-142 and IAEA TRS-398 reports. The patient workflow was verified using simulation verification, treatment plan validation, and Image-Guided Radiotherapy (IGRT).
Results: The operational parameters of the medical linear accelerator regarding the electrical, mechanical and dosimetric domains were within prescribed/ established tolerance limits. Deviation of the mechanical isocenter was 0 mm, gantry and collimator angle deviations were ≤ 0.2°, MLC positioning/dose accuracy was maintained at an average of within 1 mm throughout the entire data capture range. Relative to commissioning data, TPR20/10 (Photon beam quality indices for 6 MV (0.683) and 18 MV (0.775)) and electron depth parameters were stable. Monthly and daily output constancy measurements indicated no clinically significant drift of output for each energy.
Conclusion: By utilizing a combination of machine-based quality assurance and structured workflow controls specific to the patient, a multi-level approach allows for translating technical performance into clinical precision. This combination of tools enables the delivery of safe, replicable, and dosimetrically accurate pelvic radiotherapy treatments for cervical cancers patients and validates the integration of comprehensive quality assurance programs within public oncology facilities with limited resources.
Keywords
Quality assurance; Medical linear accelerator; External beam radiotherapy; Cervical cancer; Pelvic radiotherapy; Dosimetry; Image-guided radiotherapy
Introduction
Malignant tumors can be treated using External Beam Radiotherapy (EBRT), which utilizes increasingly complex technologies like three-dimensional conformal radiotherapy, intensity modulated radiotherapy or volumetric arc therapy. All three types of therapy require both geometric precision and dosimetric accuracy throughout the treatment process so that healthy tissue is not damaged by radiation regardless of where it is located in relation to the tumor [1,2].
The medical Linear Accelerator (LINAC) is the primary treatment delivery device used in EBRT (External Beam Radiation Therapy). The LINAC is an extremely advanced delivery system, and it is a system that is ultimately a safety critical system made up of many mechanical, electronic, and software components. When a LINAC deviates in its dosimetric accuracy, it can create a significant clinical outcome such as inaccuracy in dose delivery, decrease in tumor control probability, or increase in normal tissue damage. For this reason, it is essential that the LINAC system operates with reliability and consistency before any modern radiotherapy system can be successfully delivered to the patient.
Quality Assurance (QA) programs have therefore become an essential part of the radiotherapy department all over the world. A thorough QA program has been developed with the purpose of systematically checking whether the LINAC is operating within established tolerance limits, and is compliant with both national regulations and international guidelines (ASRT, 2000) [3]. QA programs not only aim to identify machine failures, but also to try and prevent machine failures before they occur. QA is a multidisciplinary process involving medical physicists, radiation oncologists, and radiation therapists [4].
A comprehensive quality assurance program for a medical linear accelerator usually includes three major areas are where controls related to electrical and operational safety take place to ensure that patients, employees, and the public are protected. This area of concern falls within the operational area, and includes various components that provide safety; these components include verification of interlock systems, emergency stop controls, beamon indicators, collision detection, and audio-visual monitors for patient safety [5]. Secondly, the importance of mechanical accuracy in the maintenance of the geometric integrity of the treatment delivery process cannot be overstated. Mechanical quality assurance is primarily focused on parameters that include the accuracy of the gantry, collimator, and couch position, as well as isocenter stability, optical distance indicators, lasers, and field size. Any inaccuracy in the mechanical aspects of the equipment has the potential to result in geometric inaccuracy in the treatment delivery process, especially in cases of highly conformal treatments [6]. Third, dosimetric stability ensures the accurate and repeatable administration of the prescribed dose. The dosimetric quality assurance process involves the verification of the constancy of the beam output, beam quality, symmetry, flatness, and uniformity of the photon and electron beams [7].
Various organizations including the IAEA, AAPM, ESTRO, IEC, and ICRU have produced international recommendations for linear accelerator quality assurance. Clinical environments, available resources, and regulations in your area will determine how international guidelines are implemented. Local single-center QA implementation experiences are therefore valuable because they provide practical examples of implementing recommendations in practice [8-12].
This study describes the process of implementing a comprehensive quality assurance program for a medical linear accelerator at a public oncology center in Morocco. In addition to routine operational safety tests, verification of mechanical accuracy, and dosimetric testing at predetermined intervals, this study provides a summary of the results of routine QA procedures, with particular emphasis on conformance to established tolerance limits, thereby illustrating the efficacy of the QA process.
Although international guidelines define recommended QA procedures, limited data are available describing the practical implementation of a fully integrated QA program in public oncology centers within resource-constrained environments.
In order to provide effective radiotherapy treatment for patients with gynecological tumours, in addition to ensuring equipment is functioning correctly, the patient must also be a focus of attention for ongoing quality assurance throughout the entire patient care process. Because of the wide variety of pelvic anatomy and degree of motion that occur between daily treatments (due to variability in the filling of the bladder and distension of the rectum), it is vital that quality control is maintained throughout all steps involved with obtaining the treatment (simulation, planning and delivery). This includes having the patient positioned in a reproducible manner; employing standardised patient preparation protocols; delineating tumour and organ at risk accurately; and performing systematic verification of the treatment plan, as these issues can contribute to geometric uncertainty and lead to dose delivery errors. The implementation of Image-Guided Radiotherapy (IGRT) allows the daily verification and correction of setup errors, thus ensuring that the prescribed dose is delivered precisely to all designated target volumes. Integration of quality assurance for the patient with existing machine quality assurance programmes is fundamental to achieving accurate implementation of the treatment, compliance with international dose delivery standards, and optimised clinical outcomes for patients receiving external beam radiotherapy for gynecological cancers [13-15].
Materials and Methods
QA program and test frequency
QA activities were categorized by frequency: Daily (Q), Weekly (W), Monthly (M), Semiannual (SA), and Annual (A). Tolerance limits were based primarily on AAPM TG-142 recommendations [3] and the IAEA TRS-398 dosimetry protocol [16].
The evaluated LINAC delivered photon beams (6 MV and 18 MV) and electron beams (9-18 MeV).
Electrical and functional safety controls: Electrical and functional safety QA comprised daily safety testing of all electrical equipment. This included radiation warning sign verification, door interlock verification with immediate beam termination upon door opening, emergency stop button verification to ensure beam interruption within one second, beam-off console verification, anticollision system verification, audiovisual patient monitoring, and response to power failure (Figure 1). All safety interlocks were systematically tested under simulated fault conditions to confirm reliable and immediate beam interruption, ensuring full compliance with operational safety requirements.
Fig. 1. Treatment-room safety and monitoring systems for an Elekta linear accelerator: (A) Warning indicator light; (B) Treatment-room door interlock; (C) In-room emergency stop button; (D) Emergency stop button at the treatment console; (E) Anti-collision detector; (F) Handheld control pendant for an Elekta medical linear accelerator; (G–H) Audiovisual monitoring system.
Mechanical quality assurance: Mechanical QA included verification of the mechanical isocenter (tolerance ≤ 1 mm), gantry and collimator angle accuracy (tolerance ≤ 0.5°), Optical Distance Indicator (ODI) accuracy (± 1 mm), field size accuracy and jaw positioning (± 2 mm), light–radiation field coincidence (≤ 2 mm), treatment couch translational and rotational accuracy (± 2 mm/≤ 0.5°), laser alignment (≤ 2 mm), and assessment of Multileaf Collimator (MLC) positioning and leakage. Measurements were performed using calibrated mechanical tools, Gafchromic films with PMMA buildup, graph paper verification, and alignment phantoms to ensure reliable geometric accuracy and reproducibility (Figures 2 and 3). Tolerances were based on AAPM TG-142 recommendations [13].
Fig. 2. Alignment and leveling quality assurance of the Elekta medical linear accelerator, showing (I–J) Gantry and collimator alignment reference lines, (K) Treatment head and beam exit window inspection, (L) Spirit-level–based verification of vertical and lateral alignment, (M) Treatment couch flatness and longitudinal leveling check, and (N) Digital inclinometer and precision level used for angular and couch alignment measurements.
Fig. 3. Mechanical and geometric quality assurance tests of the medical linear accelerator, illustrating (O) Collimator and field aperture inspection, (P) Light field–radiation field coincidence test using graph paper, (Q) Gantry–collimator isocenter verification setup, (R) Laser alignment and isocenter check, (S) Optical Distance Indicator (ODI) verification, and (T) Gantry angle and mechanical accuracy assessment.
Dosimetric quality assurance: Dosimetric reference conditions: Dosimetric QA included annual absolute dose calibration under standard reference conditions (SAD=100 cm, 10 × 10 cm² field size, and 200 monitor units) using a water phantom, calibrated ionization chamber(s), and an electrometer, with appropriate temperature–pressure corrections (Figure 4). Absolute calibration was performed according to the IAEA TRS-398 absorbed-dose-towater protocol, with a target tolerance of ± 1% to ensure accurate and traceable dose delivery (Figure 3). Routine dosimetric QA comprised daily output constancy checks (± 3%), weekly trend monitoring, and monthly output verification (± 2%), together with evaluation of beam symmetry and flatness (± 2%), photon beam quality index (TPR20/10), and electron beam depth parameters (R80/R50). Routine measurements were performed using dedicated QA devices and software, and all results were systematically compared against commissioning reference values to confirm long-term dosimetric stability and consistent beam performance.
Fig. 4. Experimental setup for beam data acquisition and dosimetric quality assurance of the medical linear accelerator, showing (U) The 3D water phantom system, (V) Ionization chamber and accessories, (W) Data acquisition and analysis software interface, and (X) The electrometer used for dose measurements.
Results
All electrical safety systems of the medical linear accelerator operated correctly throughout daily quality control. Emergency stop buttons, door interlocks, beam-off systems, anticollision devices, and audiovisual patient monitoring functioned reliably, with immediate beam termination triggered by door opening, emergency stop activation, or power interruption. No electrical or safety-related faults were observed (Table 1).
| Test | Conditions/Check | Result (Yes/No) |
| Indicator lights (Q) | Accelerator/Room door /Control console | Yes |
| Emergency stop (Q) | Verify emergency stop during irradiation | Yes |
| Beam interrupt/irradiation stop (Q) | Verify beam stops immediately | Yes |
| Anticollision system (Q) | Collision limit → immediate stop of equipment | Yes |
| Surveillance system (Q) | Audio and video verification | Yes |
| Door interlock (Q) | Open/close door during irradiation → beam stop | Yes |
| Radiation beams (Q) | Select radiation type and energy | Yes |
| Status lights during irradiation (Q) | Red=irradiation, Green=stop | Yes |
| Door test during irradiation (Q) | Open/close door: Green=beam latency, Red=beam operation | Yes |
| Power cut (Q) | Power off → beam stops | Yes |
| Accessories (Q) | Accessories in good condition | Yes |
| Monitor energy (Q) | Verification | Yes |
Tab. 1. Electrical safety system quality control (Daily, Q).
As summarized in Table 2, mechanical quality control confirmed excellent geometric accuracy and stability. The mechanical isocenter deviation was 0 mm (tolerance ± 1 mm), and the optical distance indicator (ODI) remained within ± 1 mm across the clinical range. Gantry and collimator angle deviations were small (0.2° and 0.1°, respectively) and below the 0.5° tolerance. Field size constancy, jaw positioning, beam axis–collimator axis coincidence, and light field–radiation field agreement all met specifications (≤ 1 mm). Treatment couch performance was highly consistent, with translational errors ≤ 0.2 mm and rotational error 0.3°, while laser alignment was maintained within 1 mm. Multileaf collimator checks showed reproducible leaf positioning with no clinically significant interleaf leakage.
| Test (Frequency) | Setup/Conditions | Equipment | Measured result | Tolerance |
Validity |
| Mechanical isocenter (M) | Gantry 0°, Collimator 0°, SSD 100 cm | Phantom + radiographic film | 0 mm | ≤ 1 mm |
Yes |
| ODI/Telemetric distance (M) | Gantry 0°, Collimator 0°, SSD 80–120 cm | Graduated rod | 0 mm | ± 1 mm |
Yes |
| Gantry angle (M) | Gantry 0°–270°, Collimator 0°, SSD 100 cm | Spirit level | 0.2° | <0.5° |
Yes |
| Collimator angle (M) | Gantry 90° or 270°, Collimator 0°, SSD 100 cm, max field | Spirit level | 0.1° | <0.5° |
Yes |
| Field size (M) | Gantry 0°, Collimator 0°, SSD 100 cm; fields 5 × 5 / 10 × 10 / 20 × 20 | Graph paper | 0.3 mm | ± 2 mm |
Yes |
| Collimator jaws (M) | Gantry 0°, Collimator 0°, SSD 100 cm; field 40 × 40 | Graph paper | 1 mm | ± 2 mm |
Yes |
| Collimator axis vs. beam axis (M) | Gantry 0°, SAD then SAD 40 | Graph paper | 0.2 mm | ≤ 1 mm |
Yes |
| Light field vs. radiation field (M) | Gantry 0°, Collimator 0°, SSD 100 cm; 10 × 10 | Gafchromic film + PMMA | 0.5 mm | ≤ 2 mm |
Yes |
| Couch (M) | Gantry 0°, SSD 100 cm | Spirit level | V: 0.2 mm; Lat/Long: 0.2 mm; Rot: 0.3° | V: ± 2 mm; Lat/Long: ± 2 mm; Rot: ≤ 0.5° |
Yes |
| Lasers (M, S) | Gantry 0°, Collimator 0°, 10 × 10 | Dedicated phantom | 1 mm | ≤ 2 mm |
Yes |
| MLC leaves (S) | Gantry 0°, Collimator 0°, SSD 100 cm | XOMAT-V film + densitometer + graph paper | 0 mm (measured); 0.1 mm (resolution) | Centering ≤ 1 mm; Accuracy and repeatability ≤ 1 mm |
Yes |
| MLC leaves (A) | Gantry 0°, Collimator 0°, SSD 100 cm | XOMAT-V film + densitometer + graph paper | 0 | Acceptance test |
Interleaf leakage (acceptance); alignment and orthogonality ± 1°; bank sag ≤ 1 mm |
Tab. 2. Mechanical quality control of the linear accelerator (Monthly/ Semiannual/Annual).
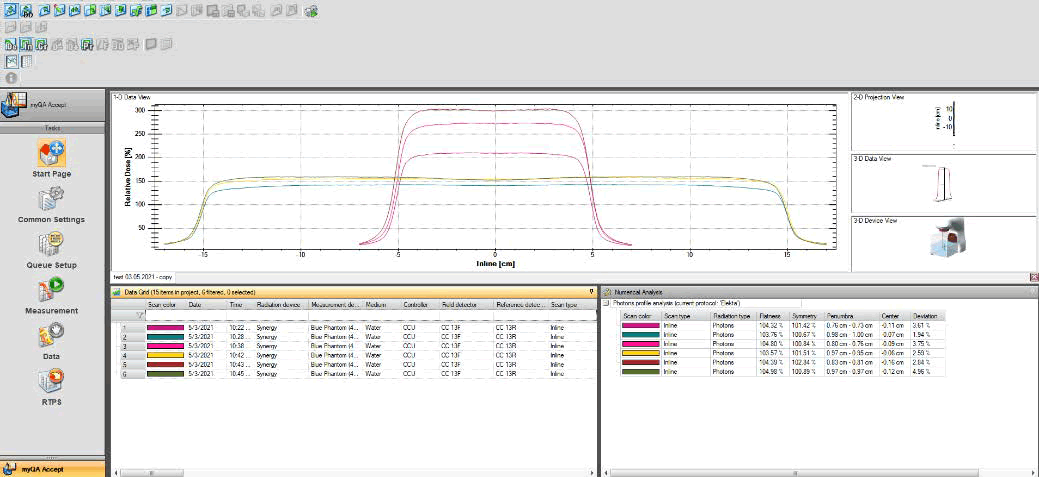
A complete dosimetric QA plan was developed to meet international guidelines (IAEA TRS-398 and AAPM TG-51/TG- 142). It included daily, monthly, and yearly check-ups to verify the stability of the beam, the output, and the energy of the beam. For daily QA includes photon and electron output constancy (± 3%) measured using a calibrated ionization chamber and a solid phantom. Monthly QA included output verification with tighter limits (±2%), beam symmetry and flatness assessment (± 2%), energy constancy checks using TPR20/10 for photons and R50 for electrons (± 2%), and verification of output factors for clinically relevant field sizes. Annual QA involved absolute dose calibration in water under reference conditions (10 × 10 cm² field size, SAD 100 cm) following IAEA TRS-398, along with full beam data verification (PDD curves, TPR measurements, beam profiles, and output factors), with an absolute calibration tolerance of ±1%. Overall, dosimetric quality control demonstrated stable performance for both modalities: Tables 3 and 5 shows that electron beam quality indices (R80/R50) for 9–18 MeV matched acceptance values and profiles satisfied symmetry/uniformity requirements, while photon beam quality remained unchanged with D (10 cm) =67.34% (6 MV) and 77.99% (18 MV) and TPR20/10=0.683 (6 MV) and 0.775 (18 MV) in Figure 5, the photon profiles also showed adequate uniformity and symmetry for standard and large fields, and weekly routine output checks confirmed no clinically relevant output drift (Table 4).
| Modality | Parameter | Energy/Field | Acceptance ( The reception) |
Routine QC ( Control) |
| Electrons | R80 (mm) | E9 (10 × 10 applicator) | 33.9 | 35.4 |
| E12 (10 × 10 applicator) | 46.33 | 47.67 | ||
| E15 (10 × 10 applicator) | 60.51 | 59.41 | ||
| E18 (10 × 10 applicator) | 69.44 | 70.02 | ||
| Photons | D (10 cm) (%) | X6 (10 × 10 field) | 67.34 | 67.34 |
| TPR20/10 | X6 (10 × 10 field) | 0.683 | 0.683 | |
| D (10 cm) (%) | X18 (10 × 10 field) | 77.99 | 77.99 | |
| TPR20/10 | X18 (10 × 10 field) | 0.775 | 0.775 |
Tab. 3. Electron beam quality indices (R80) measured during acceptance and routine quality control (SSD=100 cm, applicator 10 × 10 cm²).
| Energy | Applicator | Direction | Metric | Acceptance | Routine QC |
| E9 | 10×10 | A–B | Dmax (%) | 100.99 | 100.99 |
| Symmetry −(50–90%) | 5.5 | 5.5 | |||
| Symmetry +(50–90%) | 5 | 5 | |||
| E9 | 10×10 | G–T | Dmax (%) | 101.21 | 101.21 |
| Symmetry −(50–90%) | 5 | 5 | |||
| Symmetry +(50–90%) | 4.5 | 4.5 | |||
| E15 | 10×10 | A–B | Dmax (%) | 100.45 | 100.45 |
| Symmetry −(50–90%) | 6.2 | 6.2 | |||
| Symmetry +(50–90%) | 6.2 | 6.2 | |||
| E15 | 10×10 | G–T | Dmax (%) | 101.24 | 101.24 |
| Symmetry −(50–90%) | 5.7 | 5.7 | |||
| Symmetry +(50–90%) | 5.4 | 5.4 |
Tab. 4. Electron profile QA.
| Field (cm²) | Direction | Metric | X6 Acceptance | X6 Routine QC | X18 Acceptance | X18 Routine QC |
| 10 × 10 | G–T | Homogeneity (%) | 104.67 | 104.72 | 105.46 | 105.42 |
| Symmetry (%) | 101.25 | 101.3 | 100.67 | 100.73 | ||
| 10 × 10 | A–B | Homogeneity (%) | 104.71 | 104.82 | 105.85 | 105.82 |
| Symmetry (%) | 100.33 | 100.25 | 100.84 | 100.79 | ||
| 30 × 30 | G–T | Homogeneity (%) | 104 | 104.12 | 102.45 | 102.41 |
| Symmetry (%) | 100.64 | 100.59 | 100.46 | 100.51 | ||
| 30 × 30 | A–B | Homogeneity (%) | 103.78 | 103.7 | 103.44 | 103.54 |
| Symmetry (%) | 100.53 | 100.48 | 100.67 | 100.68 | ||
| 20 × 20 | G–T | Homogeneity (%) | 105.78 | 105.9 | 103.32 | 103.38 |
| Symmetry (%) | 100.65 | 100.7 | 101.18 | 101.12 | ||
| 20 × 20 | A–B | Homogeneity (%) | 100.16 | 106.13 | 104.15 | 104.1 |
| Symmetry (%) | 101.28 | 101.34 | 101.79 | 101.87 |
Tab. 5. Electron beam profile uniformity and symmetry results for different energies and applicators
Fig. 5. Photon beam profile measurements acquired in a water phantom, illustrating lateral dose distributions for different field sizes and depths, analyzed using the beam data acquisition software during routine dosimetric quality control of the medical linear accelerator.
The findings show that the electrical, mechanical and dosimetric measurements all met their respective tolerance criteria with no deviations beyond action levels. The system’s safety interlocks, geometric accuracy and beam characteristics were shown to be consistent; thus providing assurance of the system’s robustness, stability and reliability of the beam characteristics being delivered. Through the combined test results, the operational integrity and clinical readiness of the accelerator for routine use in radiotherapy has been shown to be established.
Discussion
The effective operation of all the electrical safety systems that were reviewed in this investigation provides evidence of the structural soundness of the accelerator's safety system and its conformity to internationally recognised QA procedures. The emergency stop buttons, door interlock devices, beam-off devices, anticollision devices and audio and video monitors are all considered safety barriers and are fundamental to preventing the accidental irradiation of individuals. As outlined in the International QA guidelines, the frequency and systematic verification of these devices is strongly emphasised due to the potential for major patient safety issues and radiation safety issues should any of these devices fail [13]. The immediate termination of the beam observed during testing during simulated fault conditions confirms that there is strong support from multicenter QA audits showing that strict compliance with interlocks testing will reduce the chance of accidental exposure incidents and improve the reliability of operations.
Excellent geometric stability of the method of mechanical quality control was demonstrated, because there was no measurable mechanical isocenter deviation and the optical distance indicator was accurate to within a sub-millimetric range. The very small angular deviations of the gantry and collimator further confirm that the structure and angularity of the entire treatment unit are structurally sound and rotationally stable. The results also compare well with previously published institutional QA series data, which report typical mechanical isocenter deviations of 0.5 to 1 mm and angular deviations of 0.3 to 0.5° for machines that are in good working order [14]. This level of geometric precision has been proven to be crucial to the delivery of IMRT and VMAT techniques since various research studies have documented that exceeding tolerance levels for rotational and/or translational errors narrow margins for target coverage and/or increase doses to organs at risk.
The satisfactory agreement of the field size, jaw position, beam axis coincidence, and light-radiation field agreements evaluated in this assessment is consistent with previously reported performance data from clinics that have employed TG-142-based Quality Assurance (QA) programmes. Additionally, satisfactory MLC performance is corroborated by the literature for MLC position accuracy being consistently ≤ 1mm in order to decrease dose calculation-delivery errors associated with these modulated treatments [15].
From a dosimetric perspective, the stability of photon and electron beam quality indices demonstrates long-term constancy of beam energy and penetration characteristics. Electron R80 and R50 values remained unchanged across the tested energy range, while photon beam parameters, including D (10) and TPR20/10, were consistent with commissioning data. Comparable longitudinal studies have reported similar stability over multi-year periods when systematic QA protocols are applied, with output variations typically remaining within ± 1–2% under controlled conditions [16]. The absence of clinically significant output drift in the present study is therefore consistent with international experience and supports the reliability of the commissioned beam model used in the treatment planning system. Maintaining such stability is essential to ensure compliance with the overall ± 5% dose accuracy objective recommended by the ICRU for external beam radiotherapy [17], which requires combined control of calibration, beam quality, geometry, and patient setup.
Overall, the findings are consistent with published evidence demonstrating that structured, guideline-driven QA programs can maintain high levels of machine performance and dosimetric accuracy over time. Although limited to a single-center experience without independent external audit verification, the results are comparable to those reported in international QA audits and institutional performance studies. These data reinforce the importance of systematic implementation of international recommendations in ensuring long-term treatment quality and patient safety, as advocated by organizations such as the IAEA and professional medical physics bodies [18].
Patient-focused QA procedures will also help ensure that gynecologic external beam radiotherapy can be safely and precisely delivered to patients, as our previously published works have shown. Specific patient-focused QA begins at the simulation stage by verifying that patients can reproduce their positions reproducibly and by providing them with the necessary immobilization devices. During simulation, it is important for patients to adhere strictly to the bladder and rectal preparation guidelines to minimize any pelvic organ motion that may occur between treatment fractions. Prior to the first fraction of treatment, laser alignment and reference marking will be checked for accuracy; these two procedures will include ensuring the accuracy of laser alignments and reference markings. Before planning approval, delineation of treatment targets and organs at risk will be peer-reviewed to minimize variability in delineation and avoid excessive normal tissue irradiation. The following parameters will be evaluated when evaluating a treatment plan to verify adherence to performance/directive criteria: The prescribed dose, planning target volume coverage, ability to contain hotspots, and compliance with the dose to the bladder, rectum, bowel and femoral heads. Prior to initiating treatment, an independent Monitor Unit calculation will be performed to aid in the verification of the accuracy of the dose delivered [19]. During treatment, Image-Guided Radiotherapy (IGRT), typically using daily or scheduled using Electronic Portal Imaging Device (EPID), or Cone Beam Computed Tomography (CBCT)is implemented to assess setup accuracy and apply necessary couch corrections, with systematic documentation and periodic review of setup shifts.
Weekly on-treatment chart reviews further ensure protocol adherence, monitor anatomical changes, and identify cases requiring adaptive replanning [20]. Together, these clinical and workflow (Figure 6) quality assurance measures translate machinelevel dosimetric and geometric accuracy experimentally validated in cervical cancer pelvic treatments using a female anthropomorphic phantom and Optically Stimulated Luminescence Dosimeters (OSLDs) [21] into individualized, safe, and reproducible radiotherapy delivery for patients with gynecological malignancies.
As Figure 6 shows, the conceptual model showing the integration of technical, geometric, and dosimetric quality control measures across successive levels of the radiotherapy workflow. The approach ensures that validated machine performance is progressively translated into accurate treatment planning and safe delivery for cervical cancer pelvic radiotherapy.
Fig. 6. Multilevel quality assurance framework linking machine performance to clinical precision in pelvic radiotherapy for cervical cancer.
Conclusion
By systematically linking technical precision to patient positioning and dose verification, this approach enhances the reliability of high-precision techniques such as IMRT and VMAT in pelvic radiotherapy. Rigorous multilevel QA therefore directly supports treatment safety, optimizes tumor control, and reduces normal tissue toxicity, underscoring its essential role in modern cervical cancer radiotherapy.
Authorship Contribution Statement
Ahlam Azalmad’s areas of expertise include conceptualization, methodology, investigation, data curation, formal analysis, visualization, writing original draft, writing review and editing, materials, and verification. Mohamed Hilal contributed to resources, data curation, project management, supervision, and writing review and editing.
Funding
No funding was received for this study.
Ethics Approval
Not applicable. This study did not involve human or animal participants.
Declaration of Competing Interest
The authors declare that they have no competing financial or nonfinancial interests.
References
- Shirato H, Le QT, Kobashi K, Prayongrat A, Takao S, et al. Selection of external beam radiotherapy approaches for precise and accurate cancer treatment. J Radiat Res. 2018; 59:i2-i10.
[Crossref] [Google Scholar] [PubMed]
- Youn Y, Schulz JB, Stolen E, Farrey K, Muresan E, et al. Linear accelerator (linac) downtime analysis assisted with a large language model (LLM). J Appl Clin Med Phys. 2025; 26:e70400.
[Crossref] [Google Scholar] [PubMed]
- Krauss R, Balik S, Cirino E, Hadley A, Hariharan N, et al. AAPM Medical Physics Practice Guideline 8.b: Linear accelerator performance tests. J Appl Clin Med Phys. 2023; 24:e14160.
[Crossref] [Google Scholar] [PubMed]
- Manjali JJ, Krishnatry R, Palta JR, Agarwal JP. Quality and safety with technological advancements in radiotherapy: An overview and journey narrative from a low and middle-income country institution. JCO Glob Oncol. 2022; 8:e2100367.
[Crossref] [Google Scholar] [PubMed]
- Kirkby C, Ghasroddashti E, Angers CP, Zeng G, Barnett E. COMP report: CPQR technical quality control guideline for medical linear accelerators and multileaf collimators. J Appl Clin Med Phys. 2018; 19:22-28.
[Crossref] [Google Scholar] [PubMed]
- Park K, Choi W, Keum K, Lee H, Yoon J, et al. Mechanical quality assurance using light field for linear accelerators with camera calibration. Phys Med. 2016; 32:120-126.
[Crossref] [Google Scholar] [PubMed]
- Rahman MM, Shamsuzzaman M, Sarker M, Jobber A, Mia M, et al. Dosimetric characterization of medical linear accelerator photon and electron beams for the treatment accuracy of cancer patients. Tsinghua Sci Technol. 2021; 3:41-59.
- International Atomic Energy Agency. Absorbed dose determination in external beam radiotherapy: An international code of practice for dosimetry based on standards of absorbed dose to water. 2000.
- Klein EE, Hanley J, Bayouth J, Yin FF, Simon W, et al. Task Group 142 report: Quality assurance of medical accelerators. Med Phys. 2009; 36:4197-4212.
[Crossref] [Google Scholar] [PubMed]
- European Society for Radiotherapy and Oncology. Guidelines for the verification of intensity modulated radiotherapy. 2008.
- International Electrotechnical Commission. Medical electrical equipment—Part 2-1: Particular requirements for the basic safety and essential performance of electron accelerators in the range 1 MeV to 50 MeV. 2020.
- International Commission on Radiation Units and Measurements. Prescribing, recording, and reporting photon-beam intensity-modulated radiation therapy (IMRT) (ICRU Report 83). J ICRU. 2010; 10.
- Hanley J, Dresser S, Simon W, Flynn R, Klein EE, et al. AAPM Task Group 198 Report: An implementation guide for TG 142 quality assurance of medical accelerators. Med Phys. 2021; 48:E830–E885.
[Crossref] [Google Scholar] [PubMed]
- Rao AK, Palanisamy M, Subrahmanyam GV, Swathi SP, Mani T. Investigation of radiation isocenter accuracy of linear accelerator: New approach of comprehensive evaluation of gantry, couch, and collimator isocenters. J Med Phys. 2025; 50:160-163.
[Crossref] [Google Scholar] [PubMed]
- Canadian Partnership for Quality Radiotherapy. Technical quality control guidelines for medical linear accelerators. 2018.
- Healy B, Butler D, Oliver C. TRS-398 Revision 1: Changes and Recommendations. Australian Radiation Protection and Nuclear Safety Agency. 2024.
- International Commission on Radiation Units and Measurements. Determination of absorbed dose in a patient irradiated by beams of X or gamma rays in radiotherapy procedures (ICRU Report 24). 1976.
- International Atomic Energy Agency. Comprehensive audits of radiotherapy practices: A tool for quality improvement. 2007.
- Azalmad A, Nhila O, Hilal M. Optimizing cervical cancer radiotherapy: Dosimetric comparison of 3D-CRT, IMRT, and VMAT: Experience at a single oncology center. J Obstet Gynecol Cancer Res. 2026; 11:192-200.
[Crossref]
- Azalmad A, Hilal M, Elmaadaoui Y. Advancing precision in cervical cancer radiotherapy: Assessing setup errors and adjusting PTV margins. J Obstet Gynecol Cancer Res. 2025; e722347.
- Azalmad A, Mohamed A, Hilal M. Experimental measurement of entrance skin dose in IMRT and VMAT for cervical cancer in the pelvic region using a female phantom and optically stimulated luminescence dosimeters. Oncol Radiother. 2025; 19:1-8.