Research Article - Onkologia i Radioterapia ( 2026) Volume 20, Issue 2
Field-Size Dependent Practical Limits of IBA CC01 and CC04 Chambers in Small-Field Dosimetry on Elekta Versa HD
Ouafae CHFIK1*, EL Mahjoub CHAKIR2, Mohamed OUALI ALAMI3, Khalid EL OUARDY4, Mohamed elghalmi5, Yassine HERRASSI6 and Khalid NABAOUI72Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco
3Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco
4Departement of Radiotherapy, Akdital clinic Khouribga, Morocco
5Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco
6Part Consult, Casablanca, Morocco
7Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomi, Morocco
Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco
Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco
Ouafae CHFIK, Faculty of Sciences, Kenitra, Morocco, Physics of Materials and Subatomic, Morocco, Email: ouafae.chfik@uit.ac.ma
Received: 01-Feb-2026, Manuscript No. OAR-26-187090; , Pre QC No. OAR-26-187090 (PQ); Editor assigned: 04-Feb-2026, Pre QC No. OAR-26-187090 (PQ); Reviewed: 20-Feb-2026, QC No. OAR-26-187090; Revised: 25-Feb-2026, Manuscript No. OAR-26-187090; Published: 28-Feb-2026
Abstract
To establish field-size dependent practical limits for the IBA CC01 and CC04 ionization chambers in small-field dosimetry on an Elekta Versa HD linear accelerator.
The study was based on an experimental dataset acquired in a water phantom and compared with Monaco Golden Beam Data (GBD) for 6 MV FFF and 10 MV FFF photon beams. Square fields ranging from 1×1 to 5×5 cm² were investigated at SSD = 90 cm, using the 10×10 cm² field as the machine-specific reference. The evaluated dosimetric parameters included percentage depth dose, lateral beam profiles, point-dose response at 10 cm depth, gamma analysis, and corrected TPR20/10. Chamber usability was assessed in terms of practical clinical acceptability across the investigated field-size range.
For both energies, measured dose per monitor unit increased progressively with field size, from 0.693 cGy/MU at 1×1 cm² to 1.000 cGy/MU at 10×10 cm² for 6 MV FFF, and from 0.664 to 1.000 cGy/MU for 10 MV FFF. Agreement with GBD remained strong, with point-dose differences ranging from −1.95% to +0.11% for 6 MV FFF and from −1.54% to +0.16% for 10 MV FFF. Minimum gamma pass rates at 2%/2 mm were between 99.2% and 99.6%. Corrected TPR20/10 values increased with field size and were systematically higher for 10 MV FFF than for 6 MV FFF. The combined dosimetric analysis indicated that detector-related limitations were most pronounced in the 1×1 and 2×2 cm² fields, where volume averaging and positioning sensitivity become more important.
CC01 is the preferred chamber for the smallest investigated fields, particularly for output-factor and profile measurements. CC04 becomes clinically reliable from about 3×3 cm² upward, where detector-related effects are less pronounced. This work provides a clinically useful framework for detector selection during commissioning and quality assurance of stereotactic small fields on Elekta Versa HD.
Keywords
Small-Field Dosimetry; Elekta Versa HD; IBA CC01; IBA CC04; Output Factor; Beam Profile; PDD; FFF Beam; Practical Limits
INTRODUCTION
Small photon fields have become an essential component of modern radiotherapy, particularly in stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT), where highly conformal dose distributions and steep dose fall-off outside the target are required [1][2]. In these techniques, geometric precision and dosimetric accuracy are critical because even small errors in beam data acquisition or detector response can propagate into clinically relevant dose uncertainties [3][4][5][6]. The accurate characterization of small fields is therefore a prerequisite for reliable beam commissioning, treatment planning system modeling, and patient-specific quality assurance [3][4]. Despite their clinical importance, small fields remain among the most challenging beam conditions in external photon radiotherapy dosimetry. As field size decreases, the assumptions that are usually valid for conventional reference dosimetry progressively break down. In particular, loss of lateral charged-particle equilibrium, partial occlusion of the radiation source, reduced head and phantom scatter, and steep dose gradients across the field make detector response increasingly dependent on detector geometry and measurement methodology [4][5][7]. These effects are strongest in very small fields and explain why detector choice cannot be separated from the physical characteristics of the beam being measured [4][5].
These challenges are especially relevant for flattening filter-free (FFF) beams. FFF beams are widely used in stereotactic practice because they provide high dose rates, shorter treatment times, and reduced head scatter compared with flattened beams [2][8]. However, the same beam characteristics that make FFF delivery attractive also increase the need for careful dosimetric characterization, particularly when very small fields are combined with high gradients and detector-size effects [4][8]. As a result, accurate small-field dosimetry in FFF beams requires not only appropriate instrumentation but also a clear understanding of where the practical limits of a detector begin to appear [4][6].
Ionization chambers remain widely used in clinical beam data acquisition because of their stability, reproducibility, relatively straightforward handling, and traceable calibration chain [3][6]. For conventional and intermediate field sizes, they remain among the most trusted detectors in radiotherapy dosimetry [3]. Their use in very small fields, however, is more complex. The finite size of the sensitive volume can produce volume-averaging effects in regions of steep dose gradient, broaden measured penumbrae, and contribute to under-response in the smallest fields [4][5][6][7]. Consequently, an ionization chamber that performs well under standard reference conditions may become progressively less suitable as the field narrows, particularly for beam profiles and output-related measurements [4][5][6][7].
Recognition of these limitations led to the development of a dedicated small-field dosimetry formalism. The work of Alfonso et al. introduced the conceptual framework for reference dosimetry in small and nonstandard photon fields, including the detector-specific correction factor formalism that later became central to international practice [5]. Building on this foundation, the IAEA issued Technical Reports Series No. 483, the first international code of practice specifically dedicated to the dosimetry of small static fields used in external beam radiotherapy [4]. TRS-483, together with its summary publication and the recommendations of AAPM TG-155, emphasizes that detector selection in small fields must be guided by field size, detector design, beam quality, and the particular quantity being measured [4][[6][7]. In other words, there is no single detector that is ideal for all small-field tasks [4][6][7].
Within this context, the IBA CC01 and IBA CC04 ionization chambers remain clinically relevant detectors for beam data acquisition, yet their practical usability in very small fields is not identical. The CC01 chamber, with its smaller sensitive volume, is expected to be less affected by volume averaging and therefore more suitable for narrow fields and high-gradient regions, whereas the CC04 chamber, despite preserving the general advantages of ion-chamber stability and ease of use, is more susceptible to spatial averaging as field size decreases [4][6][7]. From a purely theoretical point of view, this difference is well understood. From a clinical commissioning point of view, however, the more useful question is not simply which chamber is better, but rather within which field-size range each chamber can still be used with acceptable confidence in routine practice. This is precisely the type of question encouraged by the practical orientation of TRS-483 and TG-155 [4][6].
In our previous work on Elekta Versa HD, three complementary aspects of small-field dosimetry were already investigated: first, the comparative performance of the CC01 and CC04 chambers against Golden Beam Data (GBD) [9]; second, the calculation and analysis of detector-specific correction factors [10]; and third, the influence of beam energy for 6 MV FFF and 10 MV FFF beams [11]. Those studies established the dosimetric behavior of the detectors under the investigated beam conditions , but they did not fully resolve the practical commissioning question of detector usability as a function of field size. The present study was therefore conceived as a continuation of that work, using the same experimental measurement set but addressing a different endpoint: the identification of clinically meaningful field-size thresholds for practical chamber selection.
Accordingly, the aim of this study was to define the field-size-dependent practical limits of the IBA CC01 and IBA CC04 chambers for small-field dosimetry on an Elekta Versa HD linear accelerator using 6 MV FFF and 10 MV FFF photon beams. Based on an experimental dataset including percentage depth dose (PDD), lateral beam profiles, point-dose response, gamma agreement, and corrected TPR20/10 values, the study sought to determine the field-size range in which each chamber can be considered clinically acceptable for routine use. Rather than introducing a new detector-comparison exercise, this work translates an existing commissioned dataset into a practical decision framework for detector selection in small-field beam commissioning and quality assurance. This machine-specific and detector-specific perspective is intended to provide a more directly applicable contribution to clinical practice.
Materials and Methods
Data source and beam configuration
The present analysis used a grouped Monaco commissioning dataset covering four beam–detector combinations: 6 MV FFF/CC01, 6 MV FFF/CC04, 10 MV FFF/CC01, and 10 MV FFF/CC04. For each configuration, experimentally measured water-phantom data acquired with the clinical dosimetry system were compared with Monaco Golden Beam Data (GBD) in absolute comparison mode, and agreement was evaluated using global 2%/2 mm gamma criteria. The dataset also included corrected TPR20/10 values.
All data were obtained on an Elekta Versa HD linear accelerator equipped with an Agility multileaf collimator. Square field sizes of 1 × 1, 2 × 2, 3 × 3, 4 × 4, 5 × 5, and 10 × 10 cm² were analyzed at an SSD of 90 cm. Percentage depth dose (PDD) and lateral beam profile comparisons were performed at depths of 1.6, 3, 5, and 10 cm.
Detectors and study endpoint
The two detectors investigated in this study were the IBA CC01 ionization chamber, with a nominal sensitive volume of 0.01 cm³, and the IBA CC04 ionization chamber, with a nominal sensitive volume of 0.04 cm³ [12][13]. The primary objective of the study was not simply to establish a detector ranking, but to determine the practical field-size range in which each chamber can be used with sufficient confidence in routine small-field dosimetry. A detector was considered practically acceptable within a given field-size range when the overall evidence from point-dose agreement with Golden Beam Data (GBD), gamma analysis, and the expected impact of detector volume averaging supported reliable clinical use without major interpretive limitation.
The analysis was based on experimental measurements acquired in a Blue Phantom water tank using an electrometer. The evaluated quantities included point-dose response at 10 cm depth, percentage difference relative to GBD, minimum gamma pass rates, and field-size trends in corrected TPR20/10. In addition, the percentage depth dose (PDD) curves and lateral beam profiles was interpreted in relation to the measured data and the known influence of detector sensitive volume in high-dose-gradient small fields.
Data extraction and statistics
Measured and reference point doses per monitor unit at a depth of 10 cm were extracted for each investigated field size and photon energy. For each configuration, the relative difference between measured and reference dose was calculated as.
Where Dmeas is the experimentally measured dose per monitor unit and Dref is the corresponding reference dose per monitor unit from Golden Beam Data (GBD) [9–11]. Minimum gamma pass rates were also recorded from the comparison between experimental and reference distributions using a global gamma criterion of 2%/2 mm, as provided in the commissioning comparison dataset [3,9–11].
Corrected tissue-phantom ratio values, TPR20,10, were derived from the same experimental dataset and analyzed according to field size and beam energy. The interpretation of these data was performed together with the point-dose deviations, gamma agreement, percentage depth dose (PDD) behavior, and lateral profile characteristics in order to identify clinically meaningful field-size limits for chamber usability [4,6,7].
The statistical approach was primarily descriptive because the objective of the study was not hypothesis testing between independent populations, but the practical interpretation of an already established commissioning dataset. Accordingly, results were summarized in terms of field-size trends, percentage deviations, and agreement metrics, and were used to define detector-specific thresholds for routine clinical applicability [9–11].
RESULTS
Point-dose response versus field size
For both beam energies, the measured dose per MU at 10 cm depth increased monotonically with field size. For 6 MV FFF, the measured response rose from 0.693 cGy/MU at 1×1 cm² to 1.000 cGy/MU at 10×10 cm². For 10 MV FFF, the corresponding increase was from 0.664 to 1.000 cGy/MU. These data confirm the expected output loss in the smallest fields and the progressive restoration of conventional dosimetric behavior as field size increases. Measured-versus-GBD differences remained small across the dataset. For 6 MV FFF, the point-dose difference ranged from −1.95% to +0.11%. For 10 MV FFF, the range was −1.54% to +0.16%. The largest negative deviations occurred in the smallest fields, whereas values near zero were reached from 4×4 cm² upward [Table 1], [Figure 1].
| Field size | 6 MV measured | 6 MV GBD | 6 MV diff (%) | 10 MV measured | 10 MV GBD | 10 MV diff (%) |
|---|---|---|---|---|---|---|
| 1×1 | 0.693 | 0.70578 | -1.81 | 0.664 | 0.67437 | -1.54 |
| 2×2 | 0.826 | 0.84006 | -1.67 | 0.83 | 0.83733 | -0.88 |
| 3×3 | 0.874 | 0.88177 | -0.88 | 0.888 | 0.89935 | -1.26 |
| 4×4 | 0.905 | 0.90402 | 0.11 | 0.922 | 0.92175 | 0.03 |
| 5×5 | 0.93 | 0.94164 | -1.24 | 0.94 | 0.9512 | -1.18 |
| 10×10 | 1 | 1.01993 | -1.95 | 1 | 0.99841 | 0.16 |
Table 1: Measured and GBD-calculated point dose per MU at 10 cm depth
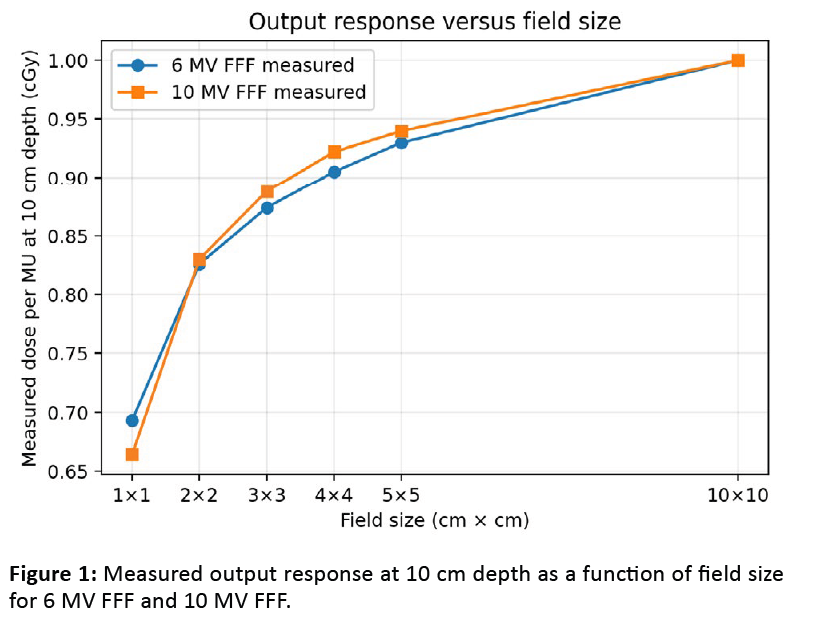
Figure 1: Measured output response at 10 cm depth as a function of field size for 6 MV FFF and 10 MV FFF.
TPR20/10 trends
The corrected TPR20/10 values showed the expected energy separation, with higher values for 10 MV FFF than for 6 MV FFF at all field sizes. For 6 MV FFF, corrected TPR20/10 ranged from 0.438 at 1×1 cm² to 0.469 at 10×10 cm². For 10 MV FFF, the corresponding values ranged from 0.446 to 0.504. The rise in corrected TPR20/10 with increasing field size is consistent with increasing beam quality stability and reduced small-field perturbation effects [Table 2], [Figure 2].
| Field size | 6MV FFF | 10MV FFF |
|---|---|---|
| 1×1 | 0.43819 | 0.44592 |
| 2×2 | 0.44106 | 0.47805 |
| 3×3 | 0.41956 | 0.47291 |
| 4×4 | 0.43308 | 0.47967 |
| 5×5 | 0.45557 | 0.48118 |
| 10×10 | 0.46897 | 0.50386 |
Table 2: Corrected TPR20/10 values obtained from the experimental dataset for 6 MV FFF and 10 MV FFF beams
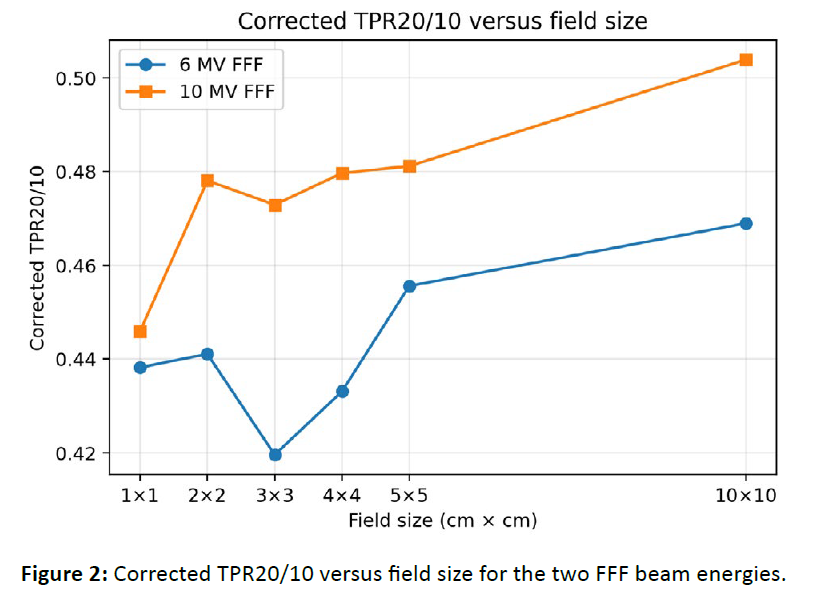
Figure 2: Corrected TPR20/10 versus field size for the two FFF beam energies.
Gamma agreement and profile/PDD consistency
Gamma analysis showed excellent agreement between the experimental dataset and the Golden Beam Data (GBD). The minimum gamma pass rates using the 2%/2 mm criterion were 99.4% for 6 MV FFF with CC01, 99.6% for 6 MV FFF with CC04, 99.2% for 10 MV FFF with CC01, and 99.6% for 10 MV FFF with CC04. Such findings indicate that the measured beam data were globally consistent and in very good agreement with the reference dataset. However, high overall gamma agreement does not eliminate the need to distinguish detector performance in the smallest fields. The greatest sensitivity to detector volume and positioning was observed in the 1×1 and 2×2 cm² range, where steep dose gradients make chamber response more dependent on sensitive volume. In this field-size region, the larger CC04 chamber is more prone to penumbra broadening and partial underestimation of the central-axis dose peak, whereas the smaller CC01 chamber better preserves sharp profile features [Figure 3].
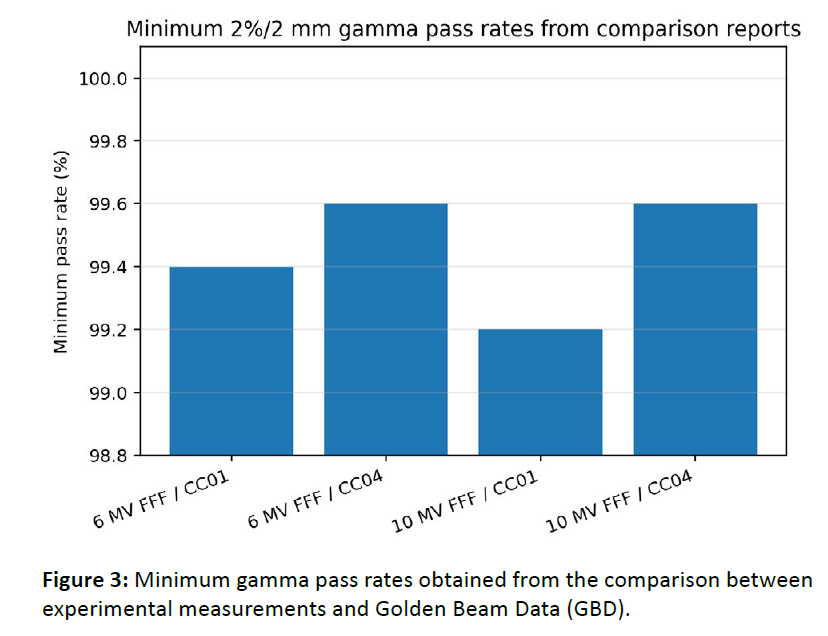
Figure 3: Minimum gamma pass rates obtained from the comparison between experimental measurements and Golden Beam Data (GBD).
Field-size dependent practical limits
Integration of the point-dose trends, gamma analysis, corrected TPR20/10 behavior, and the measured PDD/profile characteristics allowed a practical three-zone detector-selection framework to be established. For the 1×1 cm² field, CC01 is the preferred chamber because its smaller active volume limits volume averaging and provides better suitability for output-factor evaluation and high-gradient profile measurements. For the 2×2 cm² field, CC01 remains the preferred option, whereas CC04 should be considered conditionally acceptable, provided that its lower spatial fidelity and greater susceptibility to averaging effects are taken into account during interpretation. For field sizes from 3×3 to 5×5 cm², both CC01 and CC04 are clinically acceptable for routine commissioning and quality-assurance measurements. In this field-size range, agreement with GBD remains strong, corrected TPR20/10 values are more stable, and the dosimetric influence of detector size becomes less pronounced than in the smallest investigated fields [Table 3].
| Field size | CC01 usability | CC04 usability | Interpretation |
|---|---|---|---|
| 1×1 cm² | Preferred | Not recommended | CC01 is preferred for output-factor and profile measurements in the smallest field. |
| 2×2 cm² | Preferred | Conditional use | CC04 may be used with caution, but CC01 remains the safer choice. |
| ≥3×3 cm² | Acceptable | Acceptable | Both chambers are suitable for routine commissioning and quality assurance. |
Table 3: Field-size dependent practical usability of the IBA CC01 and CC04 ionization chambers for small-field dosimetry on Elekta Versa HD
DISCUSSION
The most important finding of the present study is not that one chamber is universally superior to the other, but that the practical usability of each chamber changes with field size. This distinction is clinically relevant because a detector may remain acceptable in moderately small fields yet become progressively less reliable in the very-small-field regime, where loss of lateral charged-particle equilibrium, source occlusion, reduced scatter contribution, and steep dose gradients increasingly influence detector response [1-7]. In this context, detector selection should be guided not only by overall agreement metrics but also by the physical suitability of the detector for the specific field size and measurement task [4, 6, 7, 14, 15].
The measured point-dose response decreased as field size contracted, with the largest reduction observed between the reference field and the smallest investigated fields. This behavior is consistent with established small-field dosimetry theory. As the field narrows, geometric occlusion of the photon source, reduced head and phantom scatter, and the absence of full charged-particle equilibrium contribute to a decrease in dose per monitor unit and to an increased sensitivity of the measurement to detector size and positioning [1-7]. The present results therefore follow the expected physical trend for narrow megavoltage photon beams.
Agreement between measured data and Golden Beam Data (GBD) remained very good overall, with deviations remaining within a clinically acceptable range. This supports the internal consistency and practical credibility of the commissioning dataset. However, the question of practical detector usability is more subtle than simple global agreement. Even when point-dose differences remain small, a detector with a larger sensitive volume may be less appropriate in the smallest fields because spatial averaging can smooth high-gradient regions, broaden the apparent penumbra, and partially mask local dosimetric features that are important for beam modeling and commissioning [4,6,7,14,15]. For this reason, good average agreement should not be interpreted as proof of equal detector suitability across all field sizes.
The gamma analysis supports this interpretation. Very high global 2%/2 mm pass rates were observed for both chambers, indicating strong overall agreement with the reference dataset. Nevertheless, gamma pass rate alone is not sufficient to establish detector equivalence in very small fields. The gamma formalism becomes less discriminating in steep-gradient regions because it is strongly influenced by the distance-to-agreement component, and high pass rates may therefore coexist with limited spatial resolution of the detector response [16, 17]. In small-field commissioning, gamma results should consequently be interpreted together with detector size, profile sharpness, and output sensitivity rather than being used as the sole criterion for detector selection [14–17].
The corrected TPR20, 10results behaved as expected, with consistently higher values for 10 MV FFF than for 6 MV FFF across the investigated field sizes, reflecting the greater penetrating power of the higher-energy beam. However, this energy dependence did not substantially modify the practical ranking of the two chambers. In the present dataset, the limiting factor was primarily the interaction between field size and detector volume rather than beam energy alone. This observation is in line with TRS-483 and TG-155, which emphasize that detector suitability in small fields depends mainly on detector geometry, perturbation behavior, and the quantity being measured [4, 6, 7].
From a practical commissioning perspective, the present results support a field-size-dependent interpretation of chamber usability. For field sizes from 3 × 3 cm² to 5 × 5 cm², both CC01 and CC04 appear suitable for routine PDD, profile, and output-related measurements because agreement with reference data remains strong and detector-induced distortion is limited. At 2 × 2 cm², both chambers may still be clinically usable, but CC01 is preferable because its smaller sensitive volume is better adapted to the narrower field and steeper gradients. At 1 × 1 cm², CC01 should be preferred among the two investigated ionization chambers, whereas CC04 should be used with caution, particularly when the clinical task requires accurate penumbra representation or highly resolved output characterization. This interpretation is consistent with the broader small-field literature, which shows that volume averaging becomes increasingly problematic as detector cavity size approaches a non-negligible fraction of the radiation field [4,6,7,14,15].
This field-size-based interpretation also clarifies the distinct contribution of the present manuscript relative to the earlier studies from the same project. The first study addressed comparative agreement with GBD, the second focused on detector-specific correction factors, and the third examined beam-energy effects [9–11]. The present work extends that sequence by translating the existing commissioning dataset into a practical decision framework for detector selection in routine small-field beam commissioning and quality assurance. In that sense, the study is less concerned with detector comparison as an endpoint in itself and more focused on detector usability under clinically relevant measurement conditions.
The main limitation of the study is that the analysis was performed from an already established commissioning dataset rather than from a complete reprocessing of raw scan data. As a result, some highly detailed descriptors, such as systematically recalculated penumbra widths at every depth and field size, were not derived again in the present work. Nevertheless, the available dataset was sufficiently comprehensive to identify the key practical trends, and those trends are physically coherent with established small-field dosimetry theory and published recommendations [4,6,7,14,15]. Accordingly, the conclusions remain clinically meaningful, particularly because the study objective was to define practical chamber-selection thresholds rather than to re-estimate every beam parameter from first principles.
Conclusion
This study showed that the practical usability of the IBA CC01 and CC04 chambers in small-field dosimetry depends mainly on field size. Both chambers were suitable for fields of 3 × 3 cm² and larger, whereas CC01 was preferable at 2 × 2 cm² and remained the more appropriate chamber at 1 × 1 cm². In contrast, CC04 should be used more cautiously in the smallest field sizes, particularly for profile and output measurements. These results provide a simple and clinically useful framework for detector selection in small-field commissioning and quality assurance.
References
- Taylor ML, Kron T, Franich RD. A contemporary review of stereotactic radiotherapy: Inherent dosimetric complexities and the potential for detriment. Acta Oncol. 2011; 50:483–508.
[Crossref], [Google Scholar], [PubMed]
- Guckenberger M, Baus WW, Blanck O, Combs SE, Debus J, Engenhart-Cabillic R, et al. Definition and quality requirements for stereotactic radiotherapy: Consensus statement from the DEGRO/DGMP Working Group Stereotactic Radiotherapy and Radiosurgery. Strahlenther Onkol. 2020; 196:417–420.
[Crossref], [Google Scholar], [PubMed]
- Das IJ, Cheng CW, Watts RJ, Ahnesjö A, Gibbons J, Li XA, et al. Accelerator beam data commissioning equipment and procedures: Report of the TG-106 of the Therapy Physics Committee of the AAPM. Med Phys. 2008; 35:4186–4215.
[Crossref], [Google Scholar], [PubMed]
- International Atomic Energy Agency. Dosimetry of small static fields used in external beam radiotherapy: An IAEA-AAPM international code of practice for reference and relative dose determination. Vienna: International Atomic Energy Agency; 2017. (Technical Reports Series No. 483).
- Alfonso R, Andreo P, Capote R, Huq MS, Kilby W, Kjäll P, et al. A new formalism for reference dosimetry of small and nonstandard fields. Med Phys. 2008; 35:5179–5186.
[Crossref], [Google Scholar], [PubMed]
- Das IJ, Francescon P, Moran JM, Ahnesjö A, Aspradakis MM, Cheng CW, et al. Report of AAPM Task Group 155: Megavoltage photon beam dosimetry in small fields and non-equilibrium conditions. Med Phys. 2021; 48:e886–e921.
[Crossref], [Google Scholar], [PubMed]
- Palmans H, Andreo P, Huq MS, Seuntjens J, Christaki K. Dosimetry of small static fields used in external photon beam radiotherapy: Summary of TRS-483. Med Phys. 2018; 45:e1123–e1145.
[Crossref], [Google Scholar], [PubMed]
- Xiao Y, Kry SF, Popple R, Yorke E, Papanikolaou N, Stathakis S, et al. Flattening filter-free accelerators: A report from the AAPM Therapy Emerging Technology Assessment Work Group. J Appl Clin Med Phys. 2015; 16:5219.
[Crossref], [Google Scholar], [PubMed]
- Alami MO, Al Ibrahmi EM, Chfik O, Chakir EM, El Ouardy K, Herrassi Y, et al. Small-field dosimetry on Elekta Versa HD: Comparative evaluation of IBA CC01 and CC04 chambers against golden beam data. Oncol Radiother. 2025; 19:1–8.
- Alami MO, Al Ibrahmi EM, Chfik O, Chakir EM, El Ouardy K, Herrassi Y, et al. Calculation and analysis of small-field dosimetric correction factors (K) for IBA CC01 and CC04 chambers in Elekta Versa HD 6 MV FFF and 10 MV FFF beams. Oncol Radiother. 2025; 19:1–7.
- Chfik O, Chakir EM, Alami MO, El Ouardy K, Elghalmi M, Herrassi Y. Beam energy effects in small-field dosimetry for 6 MV FFF and 10 MV FFF on Elekta Versa HD. Oncol Radiother. 2026; 20:1–10.
- IBA Dosimetry. Product catalog 2022. Schwarzenbruck: IBA Dosimetry; 2022.
- Le Roy M, Delaunay F, Bocquet M, Minkiewicz O. Assessment of small volume ionization chambers as reference dosimeters in high-energy photon beams. Phys Med Biol. 2011; 56:5635–5647.
[Crossref], [Google Scholar], [PubMed]
- Casar B, Mendez I, Huq MS, Andreo P. Output correction factors for small static fields in megavoltage photon beams for seven ionization chambers in two orientations—perpendicular and parallel. Med Phys. 2020; 47:300–319.
[Crossref], [Google Scholar], [PubMed]
- Parwaie W, Refahi S, Ardekani MA, Farhood B. Different dosimeters/detectors used in small-field dosimetry: Pros and cons. J Med Signals Sens. 2018; 8:195–203.
[Crossref], [Google Scholar], [PubMed]
- Miften M, Olch A, Mihailidis D, Moran J, Pawlicki T, Molineu A, Li H, et al. Tolerance limits and methodologies for IMRT measurement-based verification QA: Recommendations of AAPM Task Group No. 218. Med Phys. 2018; 45:e53–e83.
[Crossref], [Google Scholar], [PubMed]
- Low DA, Harms WB, Mutic S, Purdy JA. A technique for the quantitative evaluation of dose distributions. Med Phys. 1998; 25:656–661.
[Crossref], [Google Scholar], [PubMed]



