Research Article - Onkologia i Radioterapia ( 2021) Volume 15, Issue 7
Dosimetric comparison of FF and FFF beams in VMAT treatment plans of head and neck cancers
Silpa Ajay Kumar1*, Musthafa MM2, Suja CA1, Resmi KB1, Lisha Jose1, Geetha Muttath1 and Shahirabanu KP12Department of Physics, University of Calicut, Calicut University, Kerala, India
Silpa Ajay Kumar, Department of Radiation Oncology, Malabar Cancer Centre, Thalassery Kerala, India, Email: shilpa.ajith@gmail.com, shilpa_kurup@yahoo.co.in
Received: 16-Jun-2021 Accepted: 13-Jul-2021 Published: 19-Jul-2021
Abstract
Background: Currently we are using flattened beams for Volumetric Modulated Arc Therapy (VMAT) for head and neck treatments. The purpose of this study is to find whether there is any dosimetric benefits of FF beams in VMAT head & neck cancer treatments over FFF beams and vice versa.
Aim: To compare dosimetric parameters of VMAT plans with FF and FFF beams in head and neck cancers.
Materials and methods: Dosimetric data of fifty cases, Planned with FF and FFF beams, of oral cavity cancers were retrieved from the Monaco treatment planning system (version 5.2). Flattened and FFF beam plans are quantitatively compared in terms of Planning Target Volumes (PTV) Coverage, conformity index, homogeneity index, the Organ at Risk (OAR) sparing, peripheral dose and the Monitor Units (MU).
Results and Discussion: Comparable dose distributions were observed for FFF and FF VMAT plans. There was no significant difference noticed for organ at risk doses, like the spinal cord, oesophagus and parotid, of the two plans. However, FFF VMAT plans provided the lowest mean doses for OARs; no statistical significance was observed in the case of peripheral dose distribution. FF VMAT plans showed comparatively higher homogeneity and conformity with statistically significant D98 and D50 values. Monitor Units of the fifty cases were evaluated and were observed to be significantly higher for FFF plans.
Conclusion: This study of comparison of treatment planning for oral cavity cases demonstrates that FF and FFF treatment plans were in general of comparable quality. This is important in the sense that FFF need lesser delivery time there by saving the machine heating and treatment cost.
Keywords
FF, FFF, VMAT, treatment plan, head and neck plan
Introduction
Cancers of the head and neck are generally reported with delayed diagnosis and worse outcomes [1]. The majority of cases are presented with locally advanced disease necessitating multimodality treatment. Among the head and neck cancers oral Cavity cancers are prominent one. About 70% of the reported cases of head and neck cancers are found to be oral cavity cancer. Radiotherapy remains to be an integral part of many oral cavity treatments and established as an important part of the overall management of many of these tumours.
Bremsstrahlung distributions from photon beams generated from the high z target are mainly forward peaked and conical in shape. Flattening filters are introduced in the beam path to make it uniform. Flattened beams are widely used in radiotherapy. Modern radiotherapy techniques utilize fluence modifying techniques, such as Intensity-Modulated Radiation Therapy (IMRT) and Volumetric Modulated Arc Therapy (VMAT) [2]. The ability to generate intensity-modulated beams, using a multi-leaf collimator in combination with inverse planning, facilitates the use of FFF beams to generate a more conformal distribution, irrespective of the shape of the beam, which makes the flattening filter less important. Also as pointed out by Xiao et al. [3], neither patients nor targets are flat and Flattening Filter-Free (FFF) fields may be useful for moderate or even large targets. In this study, we are checking the usefulness of FFF beams in cases of comparatively larger head and neck targets.
Head and neck cancers are challenging due to the involvement of multiple critical Organs at Risk (OARs). VMAT and IMRT are prevalent treatment techniques for head and neck cancers due to their dosimetric advantages along with the preservation of nearby critical organs, with improved survival and quality of life. The clinical application of FFF beams has been investigated in many studies, which concentrated in Characteristics of FFF beams and its feasibility in planning and delivery [4-7]. Modern radiotherapy machines are facilitated with FFF beams. VMAT and IMRT plans using FFF beams has several potential advantages, such as increased dose rate, reduced collimator scatter, reduced head leakage, and reduced out-of-field doses to the patient [8-13]
Huang et al. [9], Nicolini et al. [10] and Sun et al. [12] studied the cases of Oesophageal cancers planned with FFF beams and observed significant reduction in OAR doses for FFF plans compared to FF plans. Cashmore et al. reported leakage and peripheral dose reduction for thyroid, lungs, ovaries and testis plans planned using FFF beams [13-15]. Vassiliev et al. studied the case of lung cancer and opined that FFF beams mitigate dose loss at tumour periphery and that the current clinical practice fails to capture this under dosing at the tumour periphery or possible ways to mitigate it [16, 17]. The authors are of the opinion that a higher energy selection could have improved the peripheral dose sparing of FFF beams due to the spectral distribution property [17,18]. Spruijt et al. [18] reported that the OAR doses for breast IMRT is comparable when using FF and FFF beams. Further, lower Delivery time was reported in most of the studies [19,20].
However, fewer studies were conducted using FFF beams for Head and neck cancers, which is inadequate for a reliable statistics. Studies done with larger target shows less homogeneity for FFF plans. Also these studies reported that the FFF beams resulted in similar plan qualities and dosimetric parameters when compared to FF beams, while no OAR sparing was reported [14, 15]. Further, to the best of our knowledge, there is no reported study on comparison of FF and FFF plans for oral cavity region in our study, we aim to compare the dosimetric effects during treatment delivery using Flattened and Unflattened (FFF) beams in head and neck oral cavity cancers.
Materials and Methods
Patient selection
Dosimetric data of 50 patients already treated for Head and neck cancer (planned with FF and FFF beams) were randomly retrieved from the Monaco treatment planning system. CT simulations were performed using a GE 4DCT machine (OPTIMA 580). Slice thickness of 2.5 mm were reconstructed and transferred to MIM contouring work station (version 6.8.6). Contouring of target volumes and OARs were performed by Radiation Oncologist. Contoured structures were transferred to the MONACO treatment planning system for Treatment planning.
Flattened and FFF beam plans were quantitatively compared in terms of coverage of Planning Target Volume (PTV), conformity index, homogeneity index, the Organ at Risk (OAR ) doses, peripheral dose and the Monitor Units (MU).
Radiation therapy planning
FF and FFF Plans were generated using the Monaco treatment planning system (version 5.2, Elekta Medical Systems Pvt. Ltd) for 6MV. The maximum dose rate was set to 600 MU/min for FF and 1400 MU/min for FFF. VMAT technique was used for planning. The optimization was performed inversely using the same plan parameters such as position of isocenter, beam angle, arc number and field size. Doses were calculated using Monte Carlo (MC) algorithm with 3% of statistical uncertainty per control point and 3 mm of voxel grid size. All original VMAT plans used single full arc of 360° gantry rotation from -180° to 180° in the clockwise direction and with a couch angle of 0 degrees. To exclude the bias of treatment plan skills of different individuals, in the final results, all treatment plans were designed by the same person. The planning objectives are tabulated in Table 1.
| Structures | Planning Objectives |
|---|---|
| PTV60 | V60 Gy≥95% |
| PTV54 | V54 Gy≥95% |
| Spinal Cord | Max 50Gy(full end cross section) |
| Parotid | D50% <30 Gy, Dmean< 26 Gy |
| Oesophagus | V95Gy<33% |
| Brainstem | Entire brainstem<54 Gy, V59Gy<1-10CC |
| Eye | Mean<35Gy,Max 54Gy |
| Lens | Max7Gy |
| Chiasm/Optic Nerves | Max 55Gy |
| Mandible | Max 70Gy, V75<1CC |
| Normal Tissues | As low as possible |
PTV=Planning Target Volume;VxGy=Volume receiving at least x-Gy dose
Table 1: Second optimized technique
| N | Mean | Std. Deviation | p-value | |
|---|---|---|---|---|
| FF | 50 | 307.1 | 149.332 | 0.85 |
| FFF | 50 | 303 | 147.441 |
N-Number of studied cases, FF-Flattening Filter, FFF-Flattening Filter-Free beams
Table 2: Statistical data of the high dose PTVs (Target volume covering 95% of the prescribed dose) for all studied cases
| FF Mean(SD) | FFF Mean(SD) | p Value | |
|---|---|---|---|
| Monitor Units | 1008.70 (161) | 1280.70 (169) | 0.0001 |
| Conformity Index (CI) | 0.54 (0.087) | 0.55 (0.131) | 0.1527 |
| Homogeneity Index (HI) | 0.07 (0.022) | 0.09 (1.206) | 0.0142 |
Table 3: Comparison of Monitor Units, Conformity Index (CI), and Homogeneity Index (HI)
| Variables | FF Mean(SD) | FFF Mean (SD) | p-Value |
|---|---|---|---|
| D98%(cGy) | 5912.1(96.89) | 5911.1 (75.04) | 0.0.003 |
| D50%(cGy) | 6147.8(62.79) | 6135 (186.62) | 0.004 |
| D2%(cGy) | 6313.92 (81.15) | 6329.1 (175.07) | 0.116 |
p Value=Wilcoxon test p value between VMATFF- VMATFFF. D98%=Dose received by 98% of the PTV volume
Table 4:Comparison of PTV Doses for the FFF and FF Plans for PTV (PTV 60Gy).
Treatment plan evaluation
Homogeneity index and conformity index are calculated as
Homogeneity index (HI)=(D2%-D98%)/D50 where D2%, D98% and D50% are dose to 2% , 98% and 50% volume of the PTV respectively.
Conformity index (CI)=(TVPI) 2/(PI × TV),
Where TVPI is the volume of target covered by the prescription isodose line (95%), PI is the volume of tissue covered by the prescription isodose line (95%) and TV is the total target volume. The coverage volumes of 45Gy, 30Gy, and 20Gy outside targets (V45Gy, V30Gy, and V20Gy) were used to compare the peripheral dose. OAR dose of the spinal cord, oesophagus, and parotids was also evaluated from Dose Volume Histogram (DVH) (Table 1).
Statistical Analysis
To determine the statistical significance of the differences among the techniques, the Mann-Whitney U test was performed, with a p-value of <0.05 considered to be significant, using SPSS version 20 software.
Results
Adequate coverage of target volume has been obtained for all the fifty cases, evaluated in this VMAT plan, on using FF and FFF beams. Dose distributions of the two plans (FF and FFF), for a typical case, are shown in Figure-1. Result of statistical analysis of High dose PTVs, for all the cases under study, is given in Table 2. It is observed that dosimetric differences in FF and FFF plans are not statistically significant for the target volume covering 95% of the prescribed isodose. The average DVHs for the PTVs are plotted in Figure 2. Similarly, the result of statistical analysis of Monitor Units, Conformity index and Homogeneity index, for both FFF and FF plans, are given in Table 3. It is seen that the MU shows significant difference for FF and FFF with p=0.0001, while no substantial differences were observed in homogeneity, or conformity.
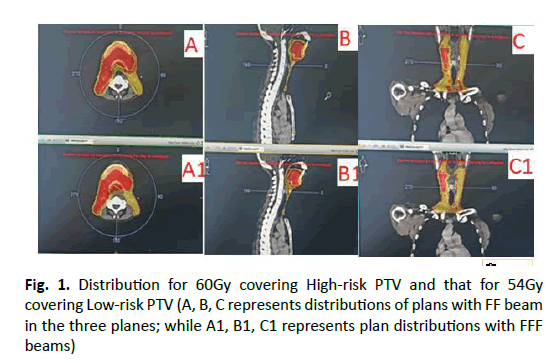
Figure 1: Distribution for 60Gy covering High-risk PTV and that for 54Gy covering Low-risk PTV (A, B, C represents distributions of plans with FF beam in the three planes; while A1, B1, C1 represents plan distributions with FFF beams)
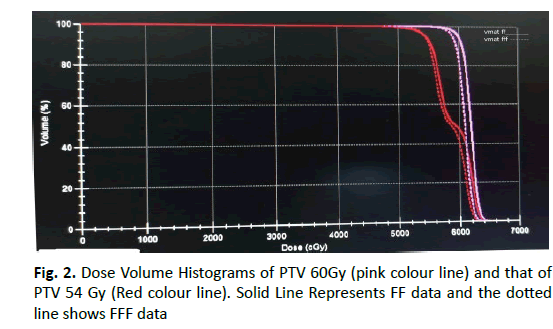
Figure 2: Dose Volume Histograms of PTV 60Gy (pink colour line) and that of PTV 54 Gy (Red colour line). Solid Line Represents FF data and the dotted line shows FFF data
Results of statistical analyses of D98%, D50% and D2% are given in Table 4. From the table it can be seen that of D98% and D50 % indicates that the dosimetric differences between FF and FFF plans are statistically significant, with a p-value of 0.003 and 0.004 respectively. While the analysis of D2% gives a p-value of 0.116 and hence it is statistically insignificant.
The coverage volumes receiving 45 Gy, 30 Gy, and 20 Gy outside target volume (V45Gy, V30Gy, and V20Gy) were used to compare the peripheral dose. Result of the statistical analysis of peripheral dose is shown in Table-5. The mean doses for FFF beams shows slightly lesser value compared to FF beams. However, no statistical significance was observed.
| Variables | FF Mean(SD) | FFF Mean (SD) | P-Value |
|---|---|---|---|
| V45(cGy) | 1375.72(299) | 1356.80(308) | 0.79 |
| V30(cGy) | 2212.34(461) | 2157.48(487) | 0.652 |
| V20(cGy) | 2723.68(591) | 2698.80(586) | 0.793 |
P-Value=Wilcoxon test p-value between VMATFF- VMATFFF. VD=the percentage volume of the PTV at the prescribed dose and D was the prescribed dose
Table 5: Dosimetric Parameters for the FFF and FF Plans
Figures 3 represent the DVH for the three organs at risk, namely, Esophagus, Spinal cord and Parotid respectively. The doses to the critical organs were comparable in both plans. The result of the statistical analysis on dose to OARs is given in Table 6. Here also it is seen that there is no significant difference of doses to organs at risk, due to FF and FFF plans.
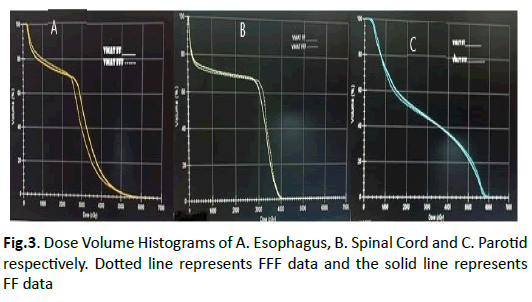
Figure 3: Dose Volume Histograms of A. Esophagus, B. Spinal Cord and C. Parotid respectively. Dotted line represents FFF data and the solid line represents FF data
Discussion
Esophagus, Spinal cord and Parotid respectively. The doses to the critical organs were comparable in both plans. The result of the statistical analysis on dose to OARs is given in Table 6. Here also it is seen that there is no significant difference of doses to organs at risk, due to FF and FFF plans.
| FF Mean(SD) (cGy) | FFFMean (SD) (cGy) | p-Value | |
|---|---|---|---|
| Spinal Cord | 4329.66(4468.10) | 4486.06(4571.92) | 0.149 |
| Esophagus | 2771.18(285.02) | 3316.20(3858.89) | 0.71 |
| Parotid | 3356.36(3468) | 3382.86(3930) | 0.581 |
Table 6: Comparison of OAR Doses among FFF and FF plans
Present analyses show that, in the case of Oral Cavity Cancer, there is no significant changes for PTV mean dose and dose coverage. Also there are no substantial differences in homogeneity and conformity indices for FF and FFF plans. Still, it is a good indication that FFF VMAT plans provide comparable results with FF VMAT plans.
Though the calculated dose to the periphery was slightly less for FFF beam plans, it was not statistically significant. This may be due to the fact that the PTV for oral cavity is relatively larger and hence the effect of conical nature of the beam may produce a radial variation of dose over the target volume. This is in line with the observations of Zhuang et al. [15] for nasopharyngeal carcinoma and Gasic et al. [14] for, Prostate, lung and Larynx.
Unlike oesophageal cases reported with reduced OARs [9- 10,12], we observed statistically not significant OAR mean dose value for FFF-VMAT plans than FF-VMAT plans, except that there is a slight reduction in the mean doses of all treated cases. This may be due to the FFF property in reducing the out-of-field dose by reducing the collimator scatter, electron contamination and head leakage as reported by Kry et al. [20].
Monitor Units (MU) obtained in FFF -VMAT plans were higher than FF-VMAT plans. This can be due to the modulation required in the case of FFF Beams to deliver uniform doses in large volume tumours, which will result in increased Monitor units. However due to the increase in dose rate the overall beam delivery time can be reduced.
Conclusion
In the current era, VMAT techniques with flattened beams are commonly utilized for the treatment of head and neck cancers. This treatment planning comparison study of oral cavity cases demonstrates that FF and FFF treatment plans are, in general, comparable in quality. Hence for moderately larger PTV, FFF plans are beneficial from the point of view of treatment time and energy conservation. Further studies with optimization of different planning parameters are desired to be performed with higher accuracy and over wide range of cases, to confirm the clinical significance of FFF beams for large PTV Volumes. However advantages like reduction in treatment time, immobilization time and out of field dose make the FFF technique beneficial in Radiotherapy treatment.
Declaration of Competing Interest
The authors have no relevant conflicts of interest to disclose. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Kumar M, Nanavati R, Modi TG, Dobariya C. Oral cancer: Etiology and risk factors: A review. J Can Res Ther. 2016;12:458-631.
- Dai X, Zhao Y, Liang Z, Dassaratha M, Wangb L, et al. Volumetric-modulated arc therapy for oropharyngeal carcinoma: a dosimetric and delivery efficiency comparison with static-field IMRT. Phys Med. 2015;31:54-59.
- Xiao Y, Kry SF, Popple R, Yorke E, Papanikolaou N, et al. Flattening filter-free accelerators: a report from the AAPM Therapy Emerging Technology Assessment Work Group. J Appl Clin Med Phys. 2015;16:5219.
- Pönisch F, Titt U, Vassiliev ON, Kry SF, Mohan R. Properties of un-flattened photon beams shaped by a multileaf collimator. Med Phys, 2006,33:1738-1746.
- Scorsetti M, Alongi F, Castiglioni S, Clivio A, Fogliata A, et al. Feasibility and early clinical assessment of Flattening Filter Free (FFF) based Stereotactic Body Radiotherapy (SBRT) treatments. Radiat Oncol. 2011;6:113.
- Georg D, Knoos T, McClean B. Current status and future perspective of flattening filter free photon beams. Med Phys. 2011;38:1280-1293.
- Mani KR, Bhuiyan MA, Rahman MS, Azharur I. Open beam dosimetric characteristics of True Beam medical linear accelerator With Flattening Filter (WFF) and Flattening Filter Free (FFF) beam. Pol J Med Phys Eng. 2018;24:79-89.
- Nicolini G, Ghosh-Laskar S, Shrivastava SK, Banerjee S, Chaudhary S, et al. Volumetric modulation arc radiotherapy with flattening filter-free beams compared with static gantry IMRT and 3D conformal radiotherapy for advanced esophageal cancer: A feasibility study. Intern J Radiat Oncol Biol Phys. 2012;84:553-560.
- Huang Y, Siochi RA, Bayouth JE. Dosimetric properties of a beam quality-matched 6 MV unflattened photon beam. J Appl Clin Med Phys. 2012;13:3701.
- Subramanian S, Thirumalaiswamy S, Srinivas C, Gandhi GA, Kathirvel M, et al. Chest wall radiotherapy with volumetric modulated arcs and the potential role of flattening filter free photon beams. Strahlenther Onkol. 2012;188:484-490.
- Yan Y, Yadav P, Bassetti M, Du K, Saenz D, et al. Dosimetric differences in flattened and flattening filter-free beam treatment plans. J Med Phys. 2016;41:92-99.
- Sun WZ, Chen L, Yang X, Wang B, Deng XW, et al. Comparison of treatment plan quality of VMAT for esophageal carcinoma with flattening filter beam versus flattening filter-free beam. J Cancer. 2018; 9:3263-3268.
- Cashmore J, Ramtohul M, Ford D. Lowering whole-body radiation doses in pediatric intensity-modulated radiotherapy through the use of unflattened photon beams. Int J Radiat Oncol Biol Phys. 2011;80:1220-1227.
- Gasic D, Ohlhues L, Brodin NP, Fog LS, Pommer T, et al. A treatment planning and delivery comparison of volumetric modulated arc therapy with or without flattening filter for gliomas, brain metastases, prostate, head/neck, and early-stage lung cancer. Acta Oncol. 2014;53:1005-1011.
- Zhuang M, Zhang T, Chen Z, Lin Z, Li D, et al. Advanced nasopharyngeal carcinoma radiotherapy with volumetric modulated arcs and the potential role of flattening filter-free beams. Radiat Oncol. 2013; 8:120.
- Vassiliev ON, Kry SF, Chang JY, Balter PA, Titt U, et al. Stereotactic radiotherapy for lung cancer using a flattening filter-free Clinac. J Appl Clin Med Phys. 2009;10:2880.
- Vassiliev ON, Titt U, Pönisch F, Kry SF, Mohan R, et al. Dosimetric properties of photon beams from a flattening filter free clinical accelerator. Phys Med Biol. 2006;51:1907-17.
- Spruijt KH, Dahele M, Cuijpers JP, Jeulink M, Rietveld D, et al. Flattening filter free vs flattened beams for breast irradiation. Int J Radiat Oncol Biol Phys. 2013;85:506-513.
- Popple R, Thomas EM, Prendergast BM, Clark GM, Dobelbower MC, et al. Effects of flattening filter-free and volumetric-modulated arc therapy delivery on treatment efficiency. J Appl Clin Med Phys. 2013;14:155-166
- Kry SF, Vassiliev ON, Mohan R. Out-of-field photon dose following removal of the flattening filter from a medical accelerator. Phys Med Biol . 2010;55:2155-2166.



