Research Article - Onkologia i Radioterapia ( 2023) Volume 17, Issue 11
Assessment of different methods of head fixation for leksell gamma knife patients
Tabarek Ali Al-Nuwab*, Mustafa S Al-Musawi and Moneer K Faraj2Department of Radiotherapy, Baghdad University, Baghdad, Iraq
Tabarek Ali Al-Nuwab, Department of Radiotherapy, Al-Mustansiriyah University, Baghdad, Iraq, Email: Laser_mu@yahoo.com
Received: 05-Jun-2023, Manuscript No. OAR-22-101297; , Pre QC No. OAR-22-101297 (PQ); Editor assigned: 07-Jun-2023, Pre QC No. OAR-22-101297 (PQ); Reviewed: 21-Jun-2023, QC No. OAR-22-101297; Revised: 25-Aug-2023, Manuscript No. OAR-22-101297 (R); Published: 01-Sep-2023
Abstract
Introduction: Families of disorders known as cancer are characterized by uncontrolled cell development and have the ability to spread or metastasis throughout the body. An essential and crucial part of cancer treatment is radiation therapy. High energy radiation is used to the cancerous tissues during radiation therapy to destroy the cancerous cells. Various intracranial targets have been treated with stereotactic radiosurgery with the leksell gamma knife for many years.
Purpose: The most recent leksell Gamma Knife (GK) generation supports both frame based and frameless techniques. In current study search the appropriate material to made anew fixation tool to solve the problem found in the others fixation tool used in gamma knife.
Materials and methods: Thirty patients with Trigeminal Neuralgia (TN) underwent GK radiosurgery employing the GK version 11.3.1 (Icon) elekta. In the present research, the decision for 3D mask fixation or thermoplastic mask was made on a case by case basis with patients' preferences taken into consideration. The 3D mask's material is checked to make sure it won't cause problems with treatment before it is put on the patients. The elekta spherical phantom is used with an ionization chamber device (PTW Semi flex 3D 31021) applied to it in order to assess the dose rate for each fixation tool.
Results: The ionization devices (PTW Semi flex 3D 31021) was used to compare dose rate for the 3D mask and thermoplastic. The dose rate for the 3D mask and thermoplastic are 0.0131, so that's a significant difference at level ≤ 0.05.
Conclusion: The 3D masks provide same results of thermoplastic for dose rate according to the test of ionization chamber that used in current study.
Keywords
Leksell gamma knife; Cancer; Ionization chamber device; 3D mask; Ionization
Introduction
Cancer is a class of diseases characterized by uncontrolled cell growth and can spread or metastasize throughout the body. In recent years, remarkable progress has been made toward the understanding of proposed hallmarks of cancer development, care and treatment modalities. Radiation therapy or radiotherapy is an essential and integral component of cancer management, mostly conferring a survival benefit. Radiation therapy destroys cancer by depositing high energy radiation on the cancer tissues [1]. The leksell Gamma Knife (GK) has been used for decades in the treatment of various intracranial targets using stereotactic radiosurgery [2]. The single fraction frame based treatment regimen poses a challenge in treating tumors ≥ 4 cm in maximum dimension due to the substantial risk of normal tissue toxicity such as radionecrosis. The advent of the gamma knife icon treatment system with integrated Cone Beam Computed Tomography (CBCT) and a High Definition Motion Management (HDMM) system has extended gamma knife treatment options to single or multi-fractional treatment regimens using frameless mask based immobilization and it may be used for large tumor volumes and cases involving a postoperative surgical cavity.
The inherent ability of the integrated CBCT system to localize the acquired image in stereotactic space enables rigid co registration with planning images Magnetic Resonance Imaging (MRI) or CT, thereby eliminating the need for a stereotactic head frame. The HDMM system monitors a patient's intra fractional motion, in which an infrared marker placed on the patient's nose is used as an external surrogate to track the intracranial target motion [3].
Materials and Methods
Different brain tumors patients received GK radiosurgery using the GK version 11.3.1 (Icon) elekta. For therapy, patients were immobilized in the traditional Leksell head frame, the thermoplastic mask, or the 3D mask. After the patients diagnoses and being forwarded to the gamma knife treatment, a Magnetic Resonance Imaging (MRI) model, achieve 3 tesla, manufactured by Philips, was used to acquire three-dimensional detailed anatomical images for the tumor. Then the Cone Beam Computed Tomography (CBCT) mounted to the gamma knife device is used to acquire the bone and solid structures of the head. According to the fixation tool utilized, in current study split patients into three groups, each consisting of ten patients. The first group fixed patients using a head frame, the second group fixed patients with a thermoplastic mask and the third group fixed patients with a 3D mask.
With regard to the first group, the frame fixation
The patient was made ready by administering lidocaine anaesthesia in four head positions and after the frame was screwed into place, the frame cap fit. This procedure was carried out in order to ensure that the patient's head or the frame would not collide with the interior of the gamma knife during treatment.
Regarding the patient who has a thermoplastic fixation
First, the patient's mask is prepared, which is a thermoplastic mask is made of Poly Methyl Methylate Acrylate (PMMA); a stereotactic mask is custom fit to the patient’s face. It is used during imaging and treatment to hold the head perfectly still; the patient lies with their head secured in an appliance attached to the treatment bed. A sheet of the plastic mask is heated to a warm temperature in an oven and then placed across the face, covering the forehead, eyes, cheeks and chin. The mask is fixed to the gamma knife device with plastic clips prepared for this purpose, after which it usually waits ten minutes for the material to harden. The patient marker is attached to the patient’s nose. Moreover, an infrared camera is operated, directed from the base of the gamma knife bed.
Regarding the patient who has a 3D mask fixation
We need the patient to come at least one day before treatment.
The patient's head is placed on the base of the gamma knife device after placing the appropriate pillow and taking the dimensions of the distance from the patient's forehead, cheek, and lower jaw to the base of the gamma knife device, and calculating the required dimensions for the purpose of fixing the mask to the gamma knife device. A special ruler was manufactured to measure the dimensions mentioned above by a 3D printer to intent to facilitate and speed up the measurement and make it more accurate. This system includes a scanner and a computer that contains a 3D drawing program with a 3D printer. A scanner is taken for the patient's face, taking measurements from the patient's cheek to the base of the gamma knife, and entering them into the three dimensional drawing computations, the mask is printed from a PLA material, and it usually takes 4:30 an hour without the need for any supporting materials for the print, and it needs the equivalent of two hundred grams only. On the day of treatment, the mask is placed directly on the patient's head to fix it during treatment without any other prior preparations, such as a water basin and other things that are applicable in the thermoplastic mask. After that, a pointer is placed on the patient's nose, which is a small circular piece made of adhesive, and an infrared camera is operated, directed from the base of the gamma knife bed (Figure 1).
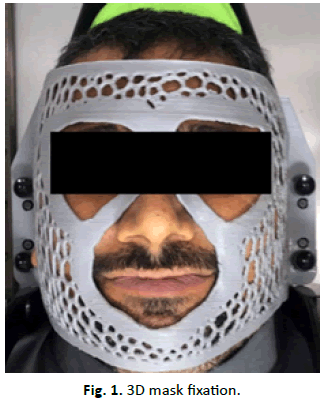
Figure 1: 3D mask fixation.
The system continuously tracks patient movement during treatment with non-rigid fixations. If large movements are detected, sources are moved to an off position and the operator is alerted, as shown in Figure 2. A gating function resumes the treatment if the patient returns to the treatment position within a specified time.
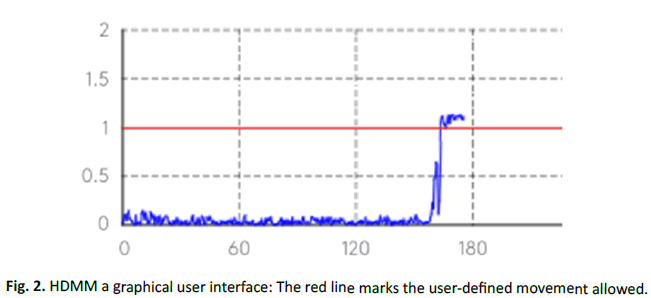
Figure 2: HDMM a graphical user interface: The red line marks the user-defined movement allowed.
For all groups, the curved shape that appeared during the treatment session was taken and analysed from the curve into digital data through the digitizer system. Before applying the 3D mask on the patients, some examination is done to ensure that the material of the 3D mask doesn't effect on the treatment. This is done by using an ionization device. An ionization chamber device (PTW Semiflex 3D 31021) was applied to the Elekta spherical phantom to evaluate the dose rate for the 3D mask and thermoplastic mask fixation tool; the Elekta spherical phantom consists of two hemispheres; the two hemispheres are held together with the help of two small Lucite® pegs and corresponding holes for the pegs in the peripheral area of the hemispheres. The slot in the central area of the phantom is used to put the sample of mask fixation tool (3D mask and thermoplastic mask) and put the head of the ionization chamber between the samples of fixation tool inside the slot in the central area of the phantom. For every fixation tool, record five measurements of the dose rate in (2 min, 4 min, 6 min, 8 min and 10 min.) At 23.2ºC and KTP=1.0018.
Results and Discussion
In current study discuss to made new material for fixation tool, according to the various study as discuss below the frame and the thermoplastic mask has some disadvantage. Mario A. Grimm and Ulrich Koppen compare mask versus frame fixation during gamma knife treatment for brain metastases; a total of 197 lesions (169 FF and 28 MF) were treated in 76 patients (59 FF and 17 MF). 187 lesions were treated with SRS and 10 with FSRT. The median dose was 22 Gy in both groups, and the median follow-up was 9.3 months; the authors found that gamma Knife treatment with MF does not result in worse outcomes or increased rates of radionecrosis [4]. Jean Regis, Louise Merly and Anne Balossier compared mask based versus frame based gamma knife ICON Radiosurgery in Brain Metastases and found that the Pain Scale Assessment (PSA) at the beginning of the GKS procedure was not different between the 2 groups. At the end of the radiosurgery itself (just after a frame or mask removal) and 1 h after the mean pain scale was higher in patients treated with the frame (p<0.05 and p<0.001, respectively) finally, the authors found single dose mask based GKS can be done with comfort and a safety efficacy comparable to frame based GKS [5]. In this studies show the first problem found in mask fixation tool it cause a pain for patients during and after treatment session. Nicolas massager and Cecile render studied acute skin allergy to thermoplastic masks used for patient immobilization during radiation therapy and founds that thermoplastic masks used for head immobilization during radiosurgery and radiotherapy procedures can induce an allergic reaction that may threaten the proper continuation of the irradiation therapy [6]. In this study show the second problem for fixation tool in gamma knife for thermoplastic mask it cause allergy for some patients these two problem motivation us to made new material for fixation to solve these problems. After determine the problem in the current study the next step search to find the new material to make a new mask without need heated as in the thermoplastic. R. Auras study the Processing technologies for polylactic acid and the properties of this material and found that PLA is a highly versatile biodegradable polymer that can be tailor made into different resin grades for processing into a wide spectrum of products (Tables 1 and 2). From the environmental viewpoint, the compostable characteristics of PLA are well suited for many applications where recycling, reuse and recovery of products are not feasible. Since the raw materials for PLA are based on agricultural feedstock, the increased demand for PLA resins will create a positive impact on the global agricultural economy [7]. Sarah Burleson, Jamie Baker, An Ting Hsia, and Zhigang X use 3D printers to create a patient specific 3D bolus for external beam therapy and found the PDD measurements and CT data concluded that the correct Hounsfield unit to use for our clear PLA printing material is 260 (Table 3). This was further confirmed by the dose plane comparison, which models a real treatment. Considering these results, Sarah Burleson, Jamie Baker, An Ting Hsia and Zhigang X are confident that we can accurately model this printing material in our treatment planning system for all energies in photon and electron beams [8]. In this study have been making 3D made from polylactic acid material as a fixation tool during treatment sessions in a gamma knife (Figures 3 and 4).
| Time (minutes) | Air | 3D mask | Thermoplastic mask | Difference between air and 3D mask | Difference between air and thermoplastic mask |
|---|---|---|---|---|---|
| 2 | 9.8 | 6.813 | 5.722 | 1.091 | 6.813 |
| 4 | 20 | 13.61 | 11.43 | 2.18 | 13.61 |
| 6 | 30 | 20.41 | 17.14 | 3.27 | 20.41 |
| 8 | 39 | 27.19 | 22.84 | 4.35 | 27.19 |
| 10 | 49 | 34 | 28.56 | 5.44 | 34 |
Tab. 1. The difference between the Air with the 3D mask and thermoplastic mask for the charge (nC) readings.
| Time (minutes) | Air | 3D mask | Thermoplastic mask | Difference between air and 3D mask | Difference between air and thermoplastic mask |
|---|---|---|---|---|---|
| 2 | 5.718 | 3.966 | 3.33 | 1.752 | 2.388 |
| 4 | 11.46 | 7.922 | 6.653 | 3.538 | 4.807 |
| 6 | 17.176 | 11.879 | 9.976 | 5.297 | 7.2 |
| 8 | 22.898 | 15.826 | 13.294 | 7.072 | 9.604 |
| 10 | 28.59 | 19.789 | 16.623 | 8.801 | 11.967 |
Tab. 2. The difference between the air with the 3D mask and thermoplastic mask for the dose rate (Gy/min) readings over time.
| Air and 3D mask | Air and thermoplastic mask | 3D Mask and thermoplastic mask | |
|---|---|---|---|
| Dose rate (Gy/min) | 0.0133* | 0.0131* | 0.0131* |
| Charge (nC) | 0.0132* | 0.0132* | 0.0136* |
| Note: *Significant difference at p-value ≤ 0.05 | |||
Tab. 3. The significance of the air difference with the 3D mask and thermoplastic mask for the dose rate (Gy/min) readings and charge (nC) over time.
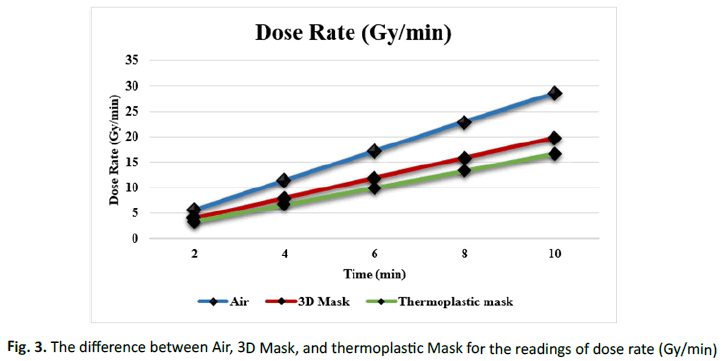
Figure 3: The difference between Air, 3D Mask, and thermoplastic Mask for the readings of dose rate (Gy/min).
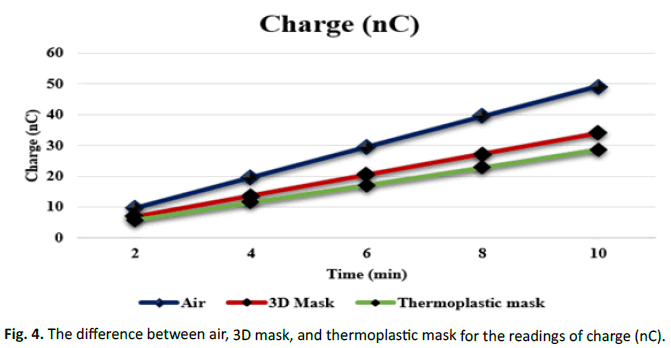
Figure 4: The difference between air, 3D mask, and thermoplastic mask for the readings of charge (nC).
Conclusion
The 3D mask provide same results of thermoplastic for dose rate according to the test of ionization chamber that used in current study.
References
- Fiorino C, Guckenberger M, Schwarz M, van der Heide UA, Heijmen B. Technology driven research for radiotherapy innovation. Mol Oncol. 2020; 14:1500-1513.
[Crossref] [Google Scholar] [PubMed]
- Duggar WN, Morris B, He R, Yang C. Total workflow uncertainty of frameless radiosurgery with the gamma Knife Icon cone beam computed tomography. J Appl Clin Med Phys. 2022; 23:13564.
[Crossref] [Google Scholar] [PubMed]
- Han EY, Diagaradjane P, Luo D. Validation of PTV margin for gamma knife Icon frameless treatment using a pseudo patient prime anthropomorphic phantom. J Appl Clin Med Phys. 2020; 21:278-285.
[Crossref] [Google Scholar] [PubMed]
- Grimm MA, Koppen U, Stieler F. Prospective assessment of mask versus frame fixation during gamma knife treatment for brain metastases. Radiother Oncol. 2020; 147:195-199.
[Crossref] [Google Scholar][PubMed]
- Regis J, Merly L, Balossier A. Mask based versus frame based gamma knife ICON radiosurgery in brain metastases: a prospective randomized trial. Stereotact Funct Neurosurg. 2022; 100:86-94.
[Crossref] [Google Scholar] [PubMed]
- Massager N, Renier C, Devriendt D. Acute skin allergy to thermoplastic mask used for patient immobilization during radiation therapy: A case report. J Med Case Rep. 2018; 12:1-2.
[Crossref] [Google Scholar] [PubMed]
- Lim LT, Auras R, Rubino M. Processing technologies for poly (lactic acid). Prog Polym Sci. 2008; 33:820-852.
- Burleson S, Baker J, Hsia AT, Xu Z. Use of 3D printers to create a patient specific 3D bolus for external beam therapy. J Appl Clin Med Phys. 2015; 16:166-178.
[Crossref] [Google Scholar] [PubMed]



