Case Reports - Onkologia i Radioterapia ( 2022) Volume 16, Issue 1
A rare case of paediatric oropharyngeal branchial cyst
Mohammed Alqarny*Mohammed Alqarny, Otolaryngology head and neck surgery, Department of Surgery, College of Medicine, University of Bisha, Saudi Arabia, Email: maalgarni@ub.edu.sa
Received: 04-Jan-2022, Manuscript No. M- 51254; Accepted: 19-Jan-2022, Pre QC No. P-51254; Editor assigned: 06-Jan-2022, Pre QC No. P-51254; Reviewed: 13-Jan-2022, QC No. Q-51254; Revised: 19-Jan-2022, Manuscript No. R-51254; Published: 27-Jan-2022
Abstract
Branchial cleft cysts are congenital epithelial cysts formed on the lateral part of the neck due to a lack of obliteration of the second branchial cleft during embryonic development. This is a case of a second branchial cyst anomaly in an 18-month-old girl who gave a brief history of acute intermittent upper airway obstruction and difficulty feeding. Paediatric oropharyngeal branchial cysts presenting as acute upper airway obstruction, stridor, and feeding difficulties are rare. Here we presented such a case. We also highlighted the importance of MRI in diagnosing the type and extension of the lesion. We also showed that cold-type dissection following bipolar electro cautery could produce good results in reducing the risk of complications and recurrence.
Keywords
branchial cleft cysts, paediatrics, congenital
Introduction
Branchial cleft cyst anomalies arise from the first through fourth pharyngeal clefts. These anomalies arise from incomplete closure of branchial clefts that would otherwise close to form several neck structures [1-3]. The second branchial cleft cyst anomaly is the most common and accounts for 95% of all branchial cyst anomalies. This cystic anomaly usually occurs on the anterior and medial aspect of the sternocleidomastoid muscle [4, 5]. However, these cysts also occur in unusual locations such as the oropharynx in rare cases. Moreover, most cysts are slow-growing and generally asymptomatic unless they press on surrounding structures, causing symptoms such as dysphagia [6].
This is a second branchial cyst anomaly in an 18-month-old girl who gave a brief history of acute intermittent upper airway obstruction and difficulty in feeding.
Case Report
This is an 18-month-old girl who presented to the emergency room. According to the parents, the girl had no apparent symptoms and was physically healthy. The chief complaints were acute onset intermittent dyspnea and stridor. In addition, the girl had difficulty feeding for the same duration.
Initial mouth and throat examination revealed a mass on the posterolateral oropharyngeal wall posterior to the left tonsil. The patient underwent additional investigation modalities, including a CT and a non-contrast MRI of the head and neck. Both examinations confirmed the presence of a cystic mass in the lateral pharyngeal wall posterior to the tongue associated with the palatopharyngeal muscle, without spinal or intracranial extension (Figure 1A and Figure 1B).
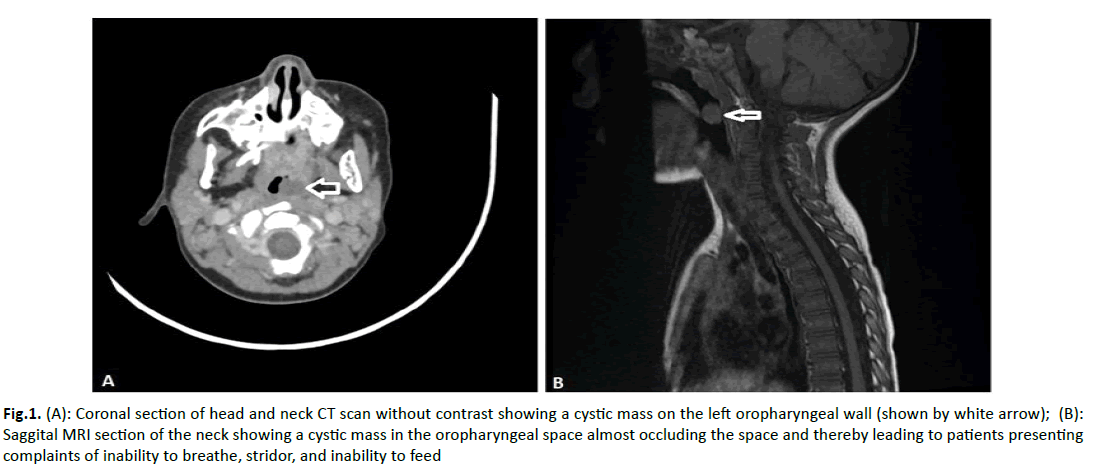
Figure 1: (A): Coronal section of head and neck CT scan without contrast showing a cystic mass on the left oropharyngeal wall (shown by white arrow); (B): Saggital MRI section of the neck showing a cystic mass in the oropharyngeal space almost occluding the space and thereby leading to patients presenting complaints of inability to breathe, stridor, and inability to feed
Parental consent was obtained for the procedure. Using the transoral approach, we removed the cyst safely. A cold dissection technique was used to achieve better surgical outcomes and minimize postoperative complications like bleeding.
Intra-operative bleeding was stopped with bipolar electrocautery. A 1 × 1 cm cyst filled with thick fluid was resected. Complete resection was achieved, and no tracts were noted.
The girl was extubated and transferred to paediatrics. In addition, she was treated with antibiotics. She also received 4 ml IV of dexamethasone every 8 hours.
The patient progressed clinically and developed no immediate or short-term surgical complications such as bleeding after being extubated transferred to a general paediatric ward, where she remained for one day. She remained stable and was discharged on the second postoperative day with treatment with oral antibiotics.
Histopathological examination revealed that the inner wall of the cyst was lined with squamous epithelium. There was lymphatic infiltration beneath the epithelium, confirming the diagnosis of the branchial cleft cyst (Figure 2).
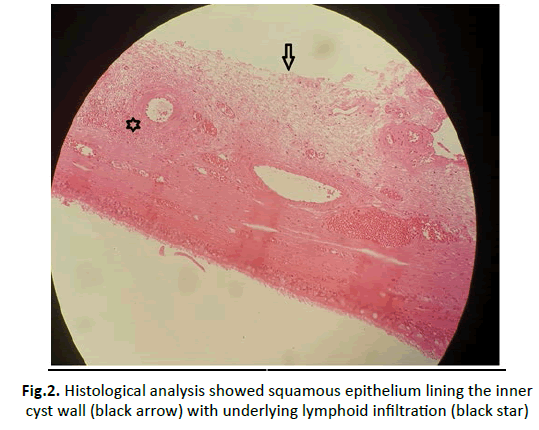
Figure 2: Histological analysis showed squamous epithelium lining the inner cyst wall (black arrow) with underlying lymphoid infiltration (black star)
During a six-month follow-up, the patient experienced no complications from the surgery or recurrence of the cyst or symptoms.
Discussion
The second branchial cyst anomaly is the most common branchial cyst anomalies [4, 5]. These anomalies generally present on the anterior or medial aspect of the sternocleidomastoid muscle, presenting as a sinus, cyst, or fistula [4, 5]. In children, cystic anomalies are most common, usually unilateral [4], as occurred in our case. However, it is unusual for them to appear on a path other than sternocleidomastoid. Here we present a rare case where the second branchial anomaly presented as a cystic mass located in the posterolateral aspect of the oropharynx behind the left tonsil.
The symptoms of the branchial anomaly depend on the type of abnormality (fistula, sinus, or cyst) and location. In most cases, the cysts are usually benign, and the mean age of presentation is 29.8 years [7]. Also, symptoms are slowly progressing, and it takes an average of 9.8 months for them to become evident [7]. Our case is unique because the cyst presented in a young girl who was 18 months old, and the symptoms had an acute onset (less than three days). Finally, most cysts present as dysphagia [6]. There have been cases where large cysts can cause upper airway obstruction [8]. Still, it is an unusual presentation, as occurred in our case.
The anatomical location of the mass is important to be determined and its relation to the surrounding structures. A thorough history and clinical examinations are crucial. Relevant investigations like CT and MRI should complete the assessment. MRI is especially important as it gives the exact location of the mass. It provides the character of the mass, whether it is homogenous, cystic, or infected. Most importantly, MRI can determine the extension of the mass and its relation to the underlying anatomical structures. This can facilitate in determining the most appropriate surgical intervention [9].
The choice of surgical approach depends on the lesion's location, size, extension, and vascular status. Transoral and transcervical are the main approaches used for resecting branchial cysts [10]. As in our case, the cystic mass was inside the oropharynx, so the transoral approach was the most appropriate. We used the cold dissection technique followed by bipolar cautery to completely resect the cystic mass as the cyst did not show any spinal or intracranial extension. We did not notice any recurrence of the cystic mass or complications related to the surgical operation or even a 6-months follow-up.
Genuine branchial cysts are covered with stratified squamous epithelium on the inside in 90% of cases. Beneath the epithelium lies the infiltration of lymphocytes [11]. Similar histopathology was noticed during the histopathological analysis of the cystic mass we resected.
Conclusion
In conclusion, branchial cystic masses are usually benign, slowgrowing and present along sternocleidomastoid. Paediatric oropharyngeal branchial cysts presenting as acute upper airway obstruction, stridor, and feeding difficulties are rare. Here we presented such a case. We also highlighted the importance of MRI in diagnosing the type and extension of the lesion. We also showed that cold-type dissection following bipolar electrocautery could produce good results in reducing the risk of complications and recurrence.
Conflicts of Interest
No conflict was alleged in this case.
References
- Patel S, Bhatt AA.Thyroglossal duct pathology and mimics. Insights Imaging. 2019;6:1-12.
- Bahakim A, Francois M, Van Den Abbeele T.Congenital Midline Cervical Cleft and W-Plasty: Our Experience. Int J Otolaryngol. 2018;2018:1-6.
- Lee DH, Yoon TM, Lee JK, Lim SC. Clinical study of second branchial cleft anomalies. J Craniofac Surg. 2018;29:e557-e560.
- Shenoy NS, Tiwari C, Gandhi S, Dwivedi P, Shah H. Anomalies of branchial cleft: our experience and review of literature. Intern Surg J. 2017;4:3234-3237.
- Tambat RM, Golasangi NA, Siddesh GB, Suhas P, Shrestha Y, et al.Type I second branchial cleft cyst in an adult patient. Intern Surg J. 2021;8:3217-3219.
- Jung SC, Oh HJ, Do NY, Park JH. Unusual presentation of second branchial cleft cyst: case reports and literature review. Korean J Otorhinolaryngol Head Neck Surg. 2016;59:140-144.
- Pupic-Bakrac J, Pupic-Bakrac A, Novakovic J, Skitarelic N. Congenital neck masses. J Craniofac Surg. 2021;32:1417-1420.
- Brown J, Carvey M, Hage R. Case of a large oropharyngeal cyst. Cureus. 2019;11:e5843.
- Shin JH, Lee HK, Kim SY, Park HW, Khang SK, et al. Parapharyngeal second branchial cyst manifesting as cranial nerve palsies: MR findings. Am J nNeuroradiol. 2001;22:510-512.
Google Scholar Cross Ref
- Saussez S, De Maesschalk T, Mahillon V, Filleul O, Louryan S.Second branchial cyst in the parapharyngealspace: a case report. Auris Nasus Larynx. 2009;36:376-379.
- Choo MJ, Kim YJ, Jin HR.A case of second branchial cleft cyst with oropharyngeal presentation. J Korean Med Sci. 2002;17:564-566.



